You want to renovate your kitchen so you call in a carpenter. You tell him you want to have one of those recessed ceilings with lights over your new kitchen counter tops. The carpenter agrees and proceeds to cut a whole in the ceiling. As chunks of the ceiling fall down, sunlight suddenly streams onto those beautiful counter tops! The carpenter yells out, “Gosh lady! You didn’t tell me you had a flat top roof!” That’s the way a dentist feels when we cannot get x-rays. We really need to know what is going on inside the teeth and bone.
Since X-rays were discovered back in 1895 by Wilhelm Conrad Röntgen, X-rays have been little understood by the public at large. It is an invisible, painless beam of radiation that passes through body tissues and projects a photogram of absorbed and non-absorbed radiation on a piece of sensitive film/sensor. Remarkable to most, but worrisome to others.
Dentists use X-rays to look into mouths everyday. It is one of the main diagnostic tools used to find pathologies in teeth, and surrounding tissue/bone structure. The best case scenario is that nothing wrong is found in and around your teeth. This has been a source of contention between our office and a few patients over the years. They feel that if there has been no decay or pathology seen in years of routine radiographs, then they take it upon themselves to refuse these regular x-ray surveys. This is seen as tolerable in our office as long as it doesn’t stretch longer than 2½ to 3 years. Any longer than that and it becomes supervised neglect between the doctor and the patient. Unfortunately in the eyes of the law, the neglect falls onto the doctors shoulders, and they are the ones who are held responsible for any undiscovered pathologies even if the patient did sign a refusal form stating they didn’t want the x-rays in the first place. It would be equivalent to needing major surgery and not having a chest X-ray just because you told your surgeon you didn’t want the chest X-ray. That would not fly in the medical profession, and it doesn’t fly in the dental profession either.
Collimation:
 The collimator is the “barrel” of the X-ray “gun”. It is a lead lined tube that helps prevent radiation scatter. When X-rays are made inside the X-ray head, the radiation comes out in all directions. By shooting the X-ray “beam” down a lead lined tube, the scattered X-rays can be aimed and prevented from hitting everyone around the room. It also focuses the beam where it is wanted and limits the exposure. The ideal length of this tube is about 20-40cm, but longer distances are best. If you do not get the film positioned directly in the path of the X-ray beam you will not expose the whole film. To the right is a phosphorus plate that has a “cone cut”. Cone cut is where the collimator was not aimed at the film properly and no radiation was available to expose the film. I actually had to pose this cone cut on my human skull that I studied in dental school because my staff uses a tool called the XCP to position the films properly and cone cuts are very rare in our office with that and/or similar devices. (Because these phosphorus “films” are reusable, once they are bent and the phosphorus layer is cracked, it shows up on every plate as a cracked white line afterwards until the plate is discarded).
The collimator is the “barrel” of the X-ray “gun”. It is a lead lined tube that helps prevent radiation scatter. When X-rays are made inside the X-ray head, the radiation comes out in all directions. By shooting the X-ray “beam” down a lead lined tube, the scattered X-rays can be aimed and prevented from hitting everyone around the room. It also focuses the beam where it is wanted and limits the exposure. The ideal length of this tube is about 20-40cm, but longer distances are best. If you do not get the film positioned directly in the path of the X-ray beam you will not expose the whole film. To the right is a phosphorus plate that has a “cone cut”. Cone cut is where the collimator was not aimed at the film properly and no radiation was available to expose the film. I actually had to pose this cone cut on my human skull that I studied in dental school because my staff uses a tool called the XCP to position the films properly and cone cuts are very rare in our office with that and/or similar devices. (Because these phosphorus “films” are reusable, once they are bent and the phosphorus layer is cracked, it shows up on every plate as a cracked white line afterwards until the plate is discarded).
This is how a collimator helps prevent scatter radiation to the rest of the body and why organs like the thyroid gland are safe from dental X-ray scatter.
Leaded Apron:
Leaded aprons are usually equipped with thyroid shields (all of ours are) that are lead lined to minimize X-ray scattered radiation. With the advent of digital sensors, which require smaller doses of radiation to receive the same or better information than from the old fashioned silver nitrate film, lead aprons have become less relevant. If all the National Council on Radiation Protection and Measure (NCRP) recommendations arefollowed, leaded aprons are actually not required. However, in our office leaded aprons are not hard to use, and are hanging where ever a X-ray is taken. For this reason it is used on every patient.
Leaded thyroid shield or collar isattached to every one of our aprons in our office, and is especially important for children and pregnant women. Some offices use just a small thyroid shield when it willnot interfere with the X-ray exposure.
List of Medical/Dental Radiation Sources:
As you look over the numbers below for the various medical (radiological) procedures that can be done to the human body, please note how low the dental exposures are compared to medical.
| Source of X-rays | Estimated Exposure (mSv) |
| Dental X-rays1 Periapical Radiograph (PA) D-speed Film1 Periapical Radiograph (PA) DigitalBitewings (4 D-speed films)Full Mouth Series (19 D-speed films)Full Mouth Series (19 digital)Panograph Panograph (digital) Cephlometric (digital) Cross Sectional Tomography Cone Beam CT (CBCT) | – – 0.00950.003250.0380.1800.060 0.019 0.093-0.310 |
| Medical X-raysTSA Airport ScanLower GI Track RadiographLower GI (Barium/Fluoroscopy follow through )Upper GI Track RadiographUpper GI (Barium/Fluoroscopy)Barium Enema (Fluoroscopy) IV Pyelogram Chest X-ray (2 views) Film Abdomen Film Pelvis Film Hip Film (unilateral) Neck Film Upper Back Film Lower Back Film Extremity (arm,leg) Skull Film DEXA Scan (bone density) Brain CT Brain/Neck CTA/CTP Neck CT Head CT scan Mammography (screening) Abdomen CT scan Abdomen CT scan (liver) Chest CT scan Chest CT (PE study) Colonography CT scan Chest/Abdomen/Pelvis CT scan Abdomen/Pelvis CT Cardiac Angiogram CT Cardiac CT (calcium scoring) Barium Enema CT scan Virtual Colonoscopy CT Neonatal Abdominal CT scan Nuclear Medicine Lung scan (Ventilation/Profusion-VQ) Cardiac stress test (Technetium) Cardiac stress test (Thallium) Liver scan (HIDA) Renal scan Whole body PET scan Bone scan Tagged WBC study Gastric Emptying Study GI Bleeding study Thyroid scan Parathyroid scan Brain scan Urea Breath test Interventional Procedures Coronary Angiogram (diagnostic) Coronary Angiogram (stent, ablation) Pulmonary Angiogram Abdominal Angiogram Head/Neck Angiogram Pelvic Vein Embolization Endoscopic retrograde Cholangiopancreatography Transjugular Interhepatic Portosystemic Shunt | – 3.6-8.8 – – |
| Natural (Earth and Atmospheric)7 hour airplane flightDenver 1 year (outerspace) Radiation ExposureUS average total radiation exposure per year | –0.0200.5103.1 |
In some countries the patients are issued a “Radiation Card” to track how much medical x-ray radiation they have received so the medical system will not overdose its patient population over time. Dental radiation is not included on these cards, probably because the doses are too low to be significant. This is why it amuses me when a medical “authority” like Dr. Oz would go on the record (TV Show) and provoke war on the dental community for taking radiographs. The simplest radiograph he would take for the heart (he is a heart surgeon) is over 10 times more radiation than dentistry’s highest radiation exposure (CBCT) and 10,000 times higher than a single dental film. All I am asking is that you, the patient, stop for one minute and put everything into perspective before refusing any dental radiographs, and that Dr. Oz reference the scientific literature before he offers advise outside of his expertise.
 The Food and Drug Administration recommendations for taking routine dental x-rays are as follows:
The Food and Drug Administration recommendations for taking routine dental x-rays are as follows:
Patient who have no decay and are not at risk of decay:
- Adults should have bitewing X-rays every 2-3 years
- Teens should have bitewing X-rays every 1½-3 years
- Children should have bitewing X-rays every 1-2 years
Patient who have tooth decay and are at risk of getting more decay:
- Adults should have bitewing X-rays every 1-1½ years
- Teens should have bitewing X-rays every ½-1 years
- Children should have bitewing X-rays every 6months until decay is controlled
Unfortunately, many dental offices have their X-ray policies written by a committee of bean counters at the patient’s individual “dental insurance company”. Insurance companies write into their policies that adult patients can only have a panograph or full mouth X-ray (FMX) every 3-5 years to look for general pathology in the mouth. This policy was written ONLY for the benefit of the insurance company. This gets back to my main point of another one of my blogs, dental insurance IS NOT INSURANCE. If it were an actual insurance then it would not matter how many types of x-rays were taken over a period of time. Most patients do not receive this many panographs because they are usually only taken on a need to know basis. But if they did have to have one then it counts as their allotted FMX. This becomes a problem because a panograph film is not used to detect fine carious lesion between the teeth. It instead is used to survey “gross” vital structures such as sinuses, inferior alveolar nerve, hard to see 3rd molars, impacted teeth, tumors, TMJ, upper and lower jaws, and any other associated pathologies. A FMX is used for a complete “fine” survey of decay between and around the teeth. Then to further complicate the situation, instead of taking 4 bitewings (BW) on our patients, we take 7 vertical bitewings. Only taking 4 BW’s on the back teeth doesn’t look between the front teeth which could have decay also. When we file with the insurance companies for 7 vertical BW’s they “don’t know what to do”, and call it a FMX (a FMX is 16-18 films and a 7 vertical BW is, well, 7 films). Not knowing what to do with 7 vertical BW’s surprises me greatly since they were introduced back in the 1977 with the advent of the XCP dental film positioner. I remember learning about vertical BW surveys from the “Grandfather of Dental Radiology”, Dr. William Updegrave, when I went to a L.D. Pankey courses back in the early 1990’s. They were advocating taking a panograph and 7 vertical BW’s as a FMX. This logical type of survey almost caught on until the insurance companies came up with their current rules to squash it. Having the insurance company not understanding these subtle but significant difference between the two types of dental radiographs has resulted in countless numbers of patients having to pay for those individual radiographs themselves. But that is just what the “Dental Insurance” company planned when it wrote those rules in the first place. (This is a subject for another blog on dental insurance)
It is not generally recommended to do a Cone Beam CT (CBCT) in place of a panograph due to the increase radiation dose unless it is for the specific purpose of diagnosing pathology from a volumetric view (tumors, abscesses, growths), or to achieve an accurate relationship between vital structures such as in implant placement, impacted canines, and third molars close to the inferior alveolar nerve. It is generally wise to fit the patient to the machine and not the machine to the patient. In other words, if the field of view (FOV) of your machine only exposes a 12″X12″ picture or the whole skull, and you are only interested in one small area, it may be inappropriate to use this machine on your patient. This is the reason why I purchased the Vatech/Ewoo PaX-Duo3D which can collimate the exposure from 12cmX8.5cm with 3 step down sizes to 5cmX5cm.
“The Hypothetical Dental Patient” lifetime radiation exposure:
This is going to be a very liberal dental case:
At our office an 84 year old female could possibly receive a full mouth x-ray (FMX) every 5 years after the age of 18. She could have had 7 vertical bitewings every 1 to 1½ years which would roughly equal 217 periapical radiographs (PA). As a child, if she had bad caries, she could have had 2 to 4 bitewings every year from about 2-3 years old to 18 years of age which would be about 64 PA’s. After looking through thousands of my own charts, patient rarely have more than 3 panographs and one cone beam CT (CBCT) so let me calculate those as well. (Digital radiographs)*
- 13 FMX 0.780 mSv
- 217 PA’s 0.705
- 64 PA’s (Pedo size) 0.208
- 3 Panographs 0.057
- 1 CBCT 0.310
The total amount of radiation for the entire lifetime accumulation for an 84 year old could be as high as 2.06 mSv which is less than 8 months of background (natural) radiation that the average US citizen receives each year, or less than one screening mammography.
*(Granted an 84 years old would have been exposed to higher amounts of dental radiation in the past because of technologies of that time, but this example is to express a patient’s current concerns).
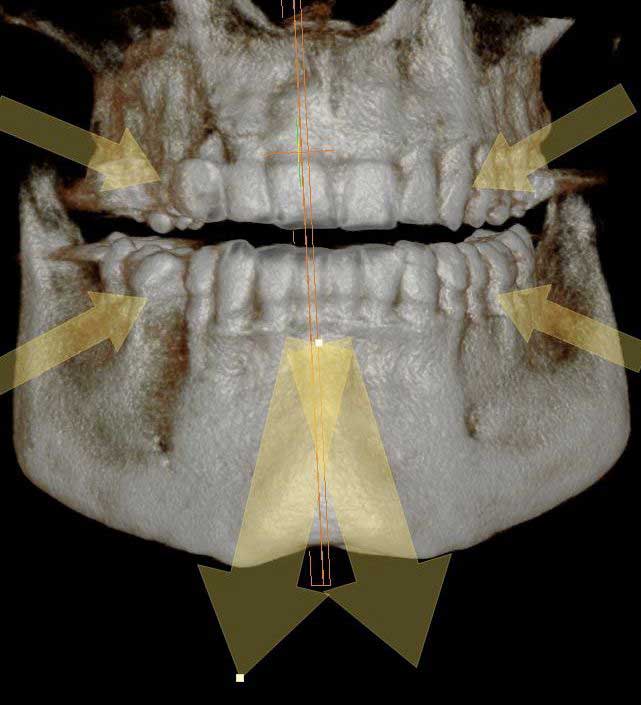 Dental X-rays are usually directed away from the the rest of the body, including the thyroid gland. The four smaller arrows show the general direction of most adult radiographs. The two larger down pointing arrows show the direction the X-ray beam has to be aimed to expose the thyroid gland.
Dental X-rays are usually directed away from the the rest of the body, including the thyroid gland. The four smaller arrows show the general direction of most adult radiographs. The two larger down pointing arrows show the direction the X-ray beam has to be aimed to expose the thyroid gland.
I hope this has helped you over come any fears you may have had regarding the safety of dental X-rays. I just hope Dr. Oz reads this someday so he too can understand the nature of dental radiographs.
References:
1. Radiat Prot Dosimetry. 2010 Apr-May;139(1-3):310-2. Quality control and patient dosimetry in dental cone beam CT. Vassileva J, Stoyanov D. Department for Radiation Protection at Medical Exposure, National Centre of Radiobiology and Radiation Protection, 132 Kliment Ohridsky blv, 1756 Sofia, Bulgaria. j.vassileva@ncrrp.org
2. Dentomaxillofac Radiol. 2008 Dec;37(8):445-52. Radiation doses in examination of lower third molars with computed tomography and conventional radiography. Ohman A, Kull L, Andersson J, Flygare L.Department of Radiology, Sunderby Hospital, SE-971 80 Luleå, Sweden. anders.ohman@nll.se
3. Health Phys. 2008 Nov;95(5):502-7. Medical radiation exposure in the U.S. in 2006: preliminary results. Mettler FA Jr, Thomadsen BR, Bhargavan M, Gilley DB, Gray JE, Lipoti JA, McCrohan J, Yoshizumi TT, Mahesh M. Radiology and Nuclear Medicine Service, New Mexico VA Health Care System, Albuquerque, NM 87108, USA. fmettler@salud.unm.edu
4. Rofo. 2008 May;180(5):396-401. [Cross-sectional imaging in dentomaxillofacial diagnostics: dose comparison of dental MSCT and NewTom 9000 DVT]. [Article in German] Coppenrath E, Draenert F, Lechel U, Veit R, Meindl T, Reiser M, Mueller-Lisse U. Institut für klinische Radiologie, Ludwig-Maximilians-Universität München. eva.coppenrath@med.uni-muenchen.de
5. Dentomaxillofac Radiol. 2008 Feb;37(2):72-9. Calculating effective dose on a cone beam computed tomography device: 3D Accuitomo and 3D Accuitomo FPD. Lofthag-Hansen S, Thilander-Klang A, Ekestubbe A, Helmrot E, Gröndahl K. Clinic of Oral and Maxillofacial Radiology, Medicinaregatan 12 C, SE-413 90 Göteborg, Sweden. sara.lofthag-hansen@vgregion.se
6. Int Endod J. 2006 Oct;39(10):827-33. Diagnostic value of computed tomography in re-treatment of root fillings in maxillary molars. Huumonen S, Kvist T, Gröndahl K, Molander A. Department of Oral and Maxillofacial Radiology at the Sahlgrenska Academy, Göteborg University/Public Dental Health Service, Göteborg, Sweden.
7. Health Phys. 2006 Aug;91(2):154-62. Medical exposure of the population from diagnostic use of ionizing radiation in luxembourg between 1994 and 2002. Shannoun F, Zeeb H, Back C, Blettner M. Ministry of Health, Directorate of Public Health, Department of Radiation Protection, Luxembourg, Luxembourg. shannoun@shannoun.com
8. Dentomaxillofac Radiol. 2006 Jul;35(4):219-26. Dosimetry of 3 CBCT devices for oral and maxillofacial radiology: CB Mercuray, NewTom 3G and i-CAT. Ludlow JB, Davies-Ludlow LE, Brooks SL, Howerton WB. Department of Diagnostic Sciences and General Dentistry, University of North Carolina School of Dentistry, Chapel Hill, NC 27599-7450, USA. jbl@email.unc.edu
9. Radiat Prot Dosimetry. 2005;115(1-4):16-22. Radiation protection standards: their evolution from science to philosophy. Dixon RL, Gray JE, Archer BR, Simpkin DJ. Department of Radiology, Wake Forest University School of Medicine, Winston-Salem, NC 27157-1088, USA. rdixon@wfubmc.edu
10. Eur J Radiol. 2005 Dec;56(3):413-7. Epub 2005 Jun 22. Dose reduction in maxillofacial imaging using low dose Cone Beam CT. Tsiklakis K, Donta C, Gavala S, Karayianni K, Kamenopoulou V, Hourdakis CJ. Department of Oral Diagnosis and Oral Radiology, School of Dentistry, University of Athens, Greece. ktsiklak@dent.uoa.gr
11. Br Dent J. 2005 May 14;198(9):565-9; discussion 557; quiz 586. A comparison of two radiographic assessment protocols for patients with periodontal disease. Jenkins WM, Brocklebank LM, Winning SM, Wylupek M, Donaldson A, Strang RM. Restorative Dentistry, Department of Periodontology, Glasgow Dental Hospital and School, 378 Sauchiehall Street, Glasgow G2 3JZ. Bill.Jenkins@northglasgow.scot.nhs.uk
12. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2003 Mar;95(3):371-7. A comparison of a new limited cone beam computed tomography machine for dental use with a multidetector row helical CT machine. Hashimoto K, Arai Y, Iwai K, Araki M, Kawashima S, Terakado M. Department of Radiology and Division os Advanced Dental Treatment, School of Dentistry and Dental Research Center, Nihon University, Tokyo, Japan. hashimoto-k@dent.nihon-u.ac.jp
13. Eur Radiol. 2002 Mar;12(3):634-7. Epub 2001 Jun 1. Radiation dose in dental radiology. Cohnen M, Kemper J, Möbes O, Pawelzik J, Mödder U. Institute of Diagnostic Radiology, Heinrich Heine University, Moorenstrasse 5, 40225 Düsseldorf, Germany. cohnen@med.uni-duesseldorf.de
14. Dentomaxillofac Radiol. 2001 Sep;30(5):255-9. Comparison of patient dose from imaging protocols for dental implant planning using conventional radiography and computed tomography. Lecomber AR, Yoneyama Y, Lovelock DJ, Hosoi T, Adams AM. Regional Medical Physics Department, Royal Victoria Infirmary, Newcastle upon Tyne, UK.
15. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2001 Jun;91(6):735-42. Comparative dose measurements by spiral tomography for preimplant diagnosis: the Scanora machine versus the Cranex Tome radiography unit. Dula K, Mini R, van der Stelt PF, Sanderink GC, Schneeberger P, Buser D. Section of Dental Radiology, Department of Oral Surgery, School of Dental Medicine, University of Bern, Bern, Switzerland. karl.dula@zmk.unibe.ch
16. Br J Radiol. 2000 Sep;73(873):1002-6. Measurement of dose in panoramic dental radiology. Williams JR, Montgomery A. Department of Medical Physics and Medical Engineering, Western General Hospital, Edinburgh, UK.
17. Rofo. 1999 Aug;171(2):130-5. [Low-dosage dental CT]. [Article in German] Rustemeyer P, Streubühr U, Hohn HP, Rustemeyer R, Eich HT, John-Mikolajewski V, Müller RD. Zentralinstitut für Röntgendiagnostik, Universität Essen. peter.rustemeyer@uni-essen.de
18. Dentomaxillofac Radiol. 1999 Jul;28(4):249-55. Use of the direct magnification technique in dental radiology. Wichmann MG, von Brenndorff AI. Department of Prosthodontics, Medical University, Hannover, Germany.
19. Ned Tijdschr Tandheelkd. 1995 Dec;102(12):484-7. [Radiation risks in dental and medical radiography]. [Article in Dutch] Geleijns J, Broerse JJ. Vakgroep Klinische Oncologie, Academisch Ziekenhuis Leiden, Interuniversitair Onderzoeksinstituut voor Radiopathologie en Stralenbescherming (IRS), Leiden.
20. Dentomaxillofac Radiol. 1995 Feb;24(1):55-8. Effective dose and risk assessment from computed tomography of the maxillofacial complex. Frederiksen NL, Benson BW, Sokolowski TW. The Baylor College of Dentistry, Dallas, Texas.
21. Swed Dent J. 1987;11(1-2):71-7. Effective dose equivalent from intraoral radiography. Stenström B, Henrikson CO, Karlsson L, Sarby B.
22. Radiation Protection in Dentistry, NCRP Report No. 145, National Council on Radiation Protection and Measurements, 2003, 191 pp. (soft cover), NCRP Publications, 7910 Woodmont Avenue, Suite 400, Bethesda, MD 20814- 3095; ISBN 0-929600-81-9; http://www.ncrp.com.
23.http://www.ncrponline.org/Publications/Reports_100-119.html
24. http://www.crcpd.org/pubs/next_docs/next99dental.pdf
26. Oral Surg Oral Med Oral Pathol. 1993 Oct;76(4):519-24. Absorbed doses with intraoral radiography. Function of various technical parameters. Hayakawa Y, Fujimori H, Kuroyanagi K. Department of Oral and Maxillofacial Radiology, Tokyo Dental College, Chiba, Japan.
27. J Am Dent Assoc. 1987 Mar;114(3):344-7. Order of magnitude dose reduction in intraoral radiography. Kircos LT, Angin LL, Lorton L.
28. Oral Surg Oral Med Oral Pathol. 1986 Dec;62(6):732-6. Efficiency of the cervical lead shield during intraoral radiography. Kaffe I, Littner MM, Shlezinger T, Segal P.
29. Swed Dent J. 1986;10(1-2):59-71. Absorbed doses from intraoral radiography with special emphasis on collimator dimensions. Stenström B, Henrikson CO, Holm B, Richter S.
30. Oral Surg Oral Med Oral Pathol. 1984 Aug;58(2):225-36. The effectiveness of the thyroid shield in dental radiology. Sikorski PA, Taylor KW.
31. Swed Dent J. 1983;7(3):85-91. Radiation shielding in dental radiography. Stenström B, Rehnmark-Larsson S, Julin P, Richter S.
32. Ont Dent. 1980 Sep;57(9):21-3. The use of the thyroid shield in dental radiography. Sikorski PA, Taylor KW.
33. “Response to University of California – San Francisco Regarding Their Letter of Concern, October 12, 2010, US Food and Drug Administration (FDA), October 12, 2010
34. Brenner DJ, Hall EJ (November 2007). “Computed tomography—an increasing source of radiation exposure”. N. Engl. J. Med. 357 (22): 2277 84. doi:10.1056/NEJMra072149.PMID 18046031.
35. Shrimpton, P.C; Miller, H.C; Lewis, M.A; Dunn, M. Doses from Computed Tomography (CT) examinations in the UK – 2003 Review
36. Frederiksen NL. X-Ray: What is the Risk? Texas Journal. 1995;112(2):68-72.