Tutorial: We have all seen enamel caries, you know the ones everyone use to call “Board Lesions”. Until recently, they have been one of those carious lesion you saw and filled, but may have felt like they were too close to call once you got into filling it. Then around the dental community we started hearing about studies were teeth with these incipient carious lesion had been remineralized and this set forth a whole new way of looking at incipient lesions, especially in children. Now a “Board Lesion” is no longer a board lesion, well at least in Florida.
This is a very interesting development in caries control that has caught on in some dental offices and not in others. The question is can you remineralize incipient carious lesions in the mouth. I think the studies have shown the answer to be , yes. However, can you remineralize carious lesions in little Johnny’s mouth who doesn’t even stand in the same room as his toothbrush? Good question. This is why we try to turn the whole family from the dark side by introducing the parents to xylitol sugar and non-alcoholic fluoride mouthwash. We even put the whole protocol into a PracticeWorks note that can be quickly entered into the patients chart without any trouble at all.
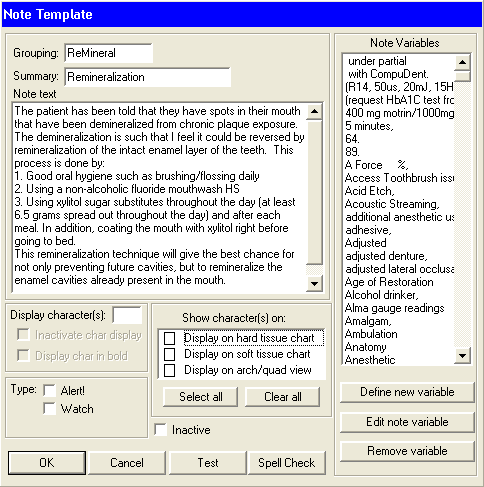
It is done with a simple note without any variables at all. Purely an informational note. We actually have a some few purely (and partially) informational notes that I’d like to share with you right now:
Remember the two ways to get into the “Note” section to write a note?
Press “Define new” if you want to write a new note.
Notice that this note has no variables, therefor, when you go to test it you get this message.
Zoom is very popular in certain dental practices. We find it to be a hassle and the dental assistants don’t like doing it. The results have been mixed from great to not at all affective. This is why we put this disclaimer on each of our Zoom patient’s charts:
<Consent> <HlthHx> The patient has been informed that this is an elective procedure designed by the manufacturer of ZOOM whitening products to whiten natural tooth structure. Natural tooth structure from one person to the next is highly variable. Therefore, there is no guarantee or warranty for this products’ ability to whiten teeth to the expectations of the patient. The patient has been further informed that the fee charged for this procedure is for chair time and not the product so therefore the same charge will be charged for any number of teeth whitened (from 1-20 teeth). Generally this product is only placed as far back as the 2nd premolars. It will not whiten restored teeth if the restoration extends to the facial of the tooth. It is best if the patient has had a recent cleaning and that the patient brushes and flosses on a regular basis. Side effect of this procedure can be gingival sensitivity, extreme cold sensitivity, and sunburn. After the treatment the patient is to avoid red wines, red meats or other staining foods. They are to use the ZOOM after -treatment tray with whitening product 2 weeks after the in office bleach to finish the whitening process. If they wish to purchase additional whitening touch-up products they may do so at the front desk.ZOOM whitening is NOT considered a permanent whitening solution and if the patient has whitened their teeth to match restore tooth shades, then they will be obligated to continue to whiten their teeth throughout their life to keep their natural tooth shade the same as their restored teeth.The patient was also informed that there are alternative ways to whiten teeth. Those are take home trays, and permanent veneers/crowns/bridges. Only the latter are considered a permanent whitening solution.
The two variables on top could just as easily have been placed in plain text like the rest of the note.
Everyone has heard of the connection between cardiovascular disease and periodontal disease so this note is entered on each perio patient:
The variables <smoking>, <weight>, <HBP2>, <Refer> are optional and have to do more with the contributing factors for heart disease.
And this note below is also entered into the chart.
These variables are just “Check-box” and list what the general treatment plan is for treating this particular perio patient with.
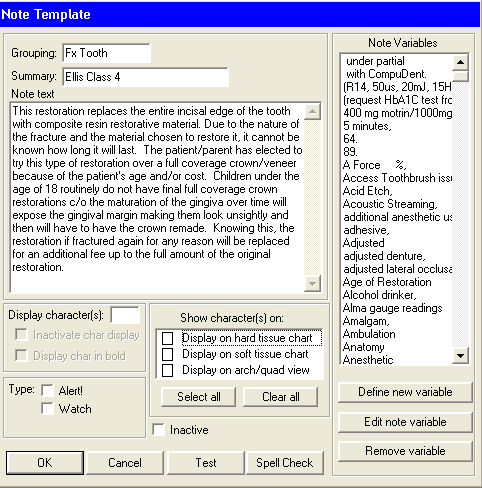
Here’s a good one for that filling with very deep decay:
Patient has been informed that this tooth has a very deep filling and is very close to the nerve. The patient is to look for symptoms of irreversible pulpitis which include prelonged sensitivity to cold (greater than a minute), prolonger sensitivity to heat (possibly releaved by cold), spontaneous pain (especially at night), or a swelling and/or draining sinus tract associated with this tooth.
A large deep filling was placed in the tooth today with the understanding that tooth may (over a period of 6 weeks) become symptomatic with discomfort and pain. If the tooth remains assymptomatic the tooth may still die and require definative treatment in the future. If irreversible pulpitis occurs (with the exception of a cracked tooth which may be non-restorable); the tooth will require endodontic treatment, post/core build up and crown to be saved. Patient is further informed that once a tooth has irreversible pulpitis, the only definative treatment alternatives are either restoring the tooth or extraction.
Have any patient on Bisphosphonates and want an extraction or implant?
Recent reports in the scientific literature have indicated a significant risk for the development of osteonecrosis (disease/destruction of jaw bone in the mouth) in patients taking intravenous bisphosphonate medications for the treatment of various cancers, osteoporosis, and other bone metabolic diseases. The complication is seen most often when the more potent forms of the medication were used intravenously or with prolonged and/or high doses given of oral medications. The concern for many patients considering dental implants or other elective oral surgical procedures is the degree of risk/benefit in taking oral bisphosphonates, such as <bisphospho> <bisphospoLen> The osteonecrosis cases that have been reported with the use of oral forms of the drug had been at higher doses for more than 2.5 years or with lower doses for more than 5 years.
We do know that the risk of osteonecrosis appears to be associated with trauma to the jaws, such as would occur with a tooth extraction or dental implant placement. But reports of spontaneous osteonecrosis of the jaws associated with these drugs are in the scientific literature as well.
It is impossible at this time to know the degree of risk for an individual patient or procedure. Due to the recent reports, we feel that we must make patients aware of this fact if they are considering extractions or dental implants.
If you are taking such drugs for the treatment of osteoporosis, it is also impossible to know whether or not discontinuing the drugs prior to your procedure will decrease or eliminate the risk for the disorder. If you have been taking high doses or even low doses for a significant time period it may be prudent to discontinue the use of these drugs for several weeks or months prior to having an elective procedure done. Literature supports that the bone density benefits derived from at least one of the bisphosphonates were still present even after discontinuing therapy for 2-3 years. We recommend that you discuss this possible complication with your prescribing physician.
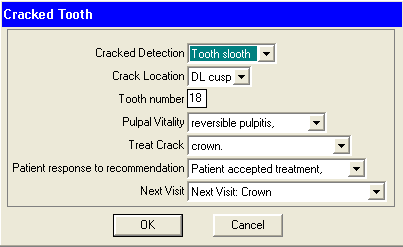
Got a cracked tooth you want to restore?
The patient shows signs of a cracked tooth. They say that their tooth hurts (jolts with discomfort) when biting on this tooth a certain way with certain foods. <slooth> confirmed on the <crackLocation>. Patient was told that tooth #<toothNum> has a crack. They were also told that a crack is a very difficult condition to diagnosis and treat. That a crack can progress through the enamel into the dentin and this will cause the biting symptoms they are experiencing. Also that if the crack progresses through the dentin it could infect the nerve causing death to the pulp chamber. They were also told that a crack can progress through the pulp chamber and through the floor of the tooth and/or down the root(s).
The patient was told that once symptoms started and continue that a crack + procrastination could equal an EXTRACTION. That the key to successful treatment of a crack is early intervention and full cuspal coverage restoration such as a crown. That if symptom of irreversible pulpitis occur that a root canal treatment will need to be preformed even after the crown has been placed. This may require going through the crown to do the root canal which will follow either by repairing the crown or replacing it. The patient was also alerted to the fact that even though a root canal and crown restoration is placed over a cracked tooth, the tooth could still show signs and symptoms of a crack and lead to continued discomfort that could end up with an EXTRACTION.
The patient was told that it is up to them to decide what treatment to follow weither it be trying to repair the crack as described above or EXTRACTION. The patient shows signs of <SignCrack> The patient has chosen to treat the symptoms of the crack with a <TrCrack> Risks, benefits and alternative discussed. <RecResp> <Next Visit>
The “Crack Detection” variable in a Multi-choice that has two entries: Tooth slooth, and visual. The “Crack Location” has: MF cusp, ML cusp, DF cusp, DL cusp. The “Tooth number” is a number variable from 1-32 with no decimal points. “Pulpal Vitality” is either reversible or irreversible pulpitis. “Treat Crack” is a multi-choice variable with three choices: “crown.”, “endo/post/crown.”, and “EXTRACTION.”. Putting in teh “Patient responce to recommendation” is: “Patient will “Think about it.”, “Patient accepts treatment,”, and “Patient declines treatment,”. And finally the add on “Next Visit:” variable.
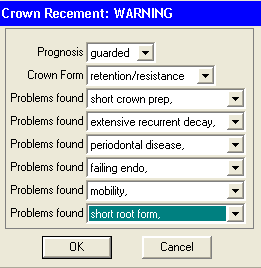
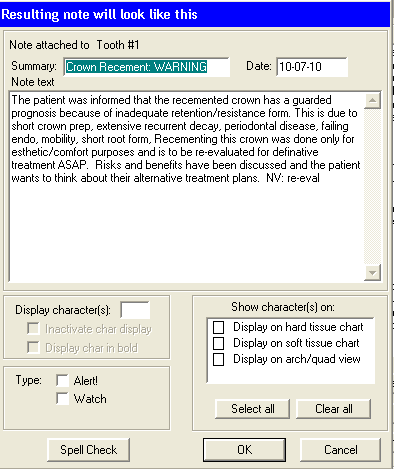
Have you ever re-cemented a crown and told the patient this crown needs to be remade because it has a non-reparable defect? How do you document this?
Delivered an ortho retainer?
Delivered post-Orthodontic retention. OHI. Told pt to wear the retainer 24/7 for the first year and at night for several years after. The patient was also informed how to clean and take care of the retainer(s). That included washing the retainer once a day with either soap and water or toothpaste with it out of the mouth. The patient was also instructed to brush and floss regularly twice or more per day. Patient told not to let dogs near the retainer unattended or to wrap it in a napkin at the dinner table/resturant or it will be thrown away with the trash and another ($) will have to be remade. The patient was furhter informed that if they do not wear their retainer(s) according to these instructions that their teeth can relapse to a crooked state and may have to have orthodontics again ($). Patient understood and accepted the responsibility.
Here’s another good one to use:
Bad breath anyone?
I have detected organoleptically what appears to be a super-infection of gram negative anaeorbic bacteria in the patient’s mouth. Explained that some of the causes included but not limited to the frequent useage of mouth washes that contain alcohols or peroxides; frequent usage of antiacids; periodontal disease; impacted teeth; caries/necrotic teeth; tonsiliths. The patient was told that gram negative anaerobes use sulfur containing amino acids from the sluffing skin of the mouth and certain kinds of foods to obtain sulfur for simple respiration within the bacteria cell. This simple respiration releases sulfur dioxide gas in the form of volitile sulfur compounds that are detected organoleptically in very low concentrations.
The patient was told to get his teeth cleaned regularly, to avoid alcohol and peroxide containing mouthwashes and to instead use a product called Smart Mouth bid. Smart Mouth contains a propietory zinc compound that blocks the up take of sulfur containing amino acids by the bacteria therefor limiting the respiration of sulfur into volitile sufur compounds which is the main cause of halitosis. NV re-eval
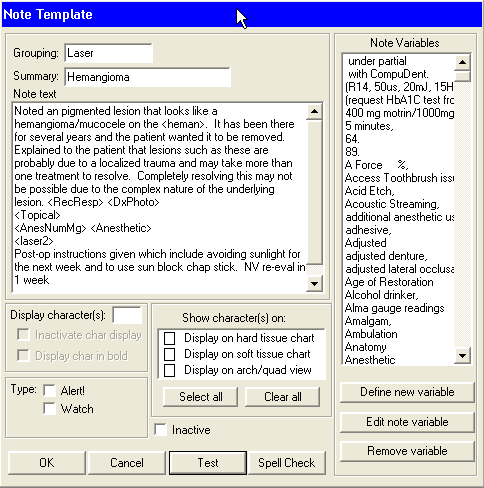
Here’s one you may not have thought about:
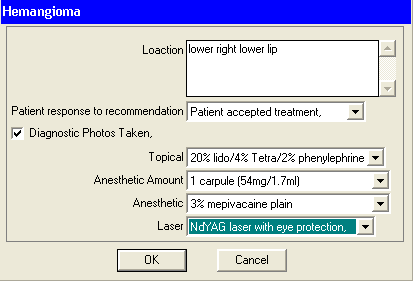
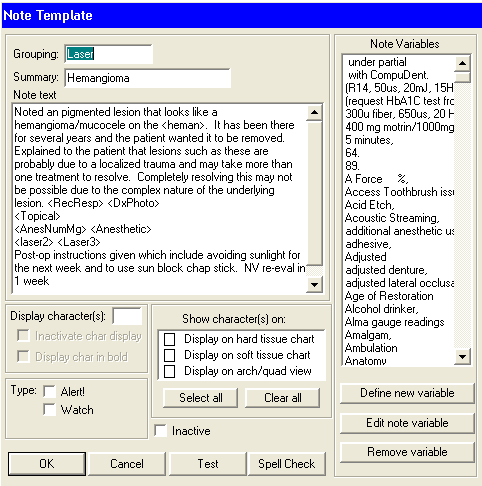
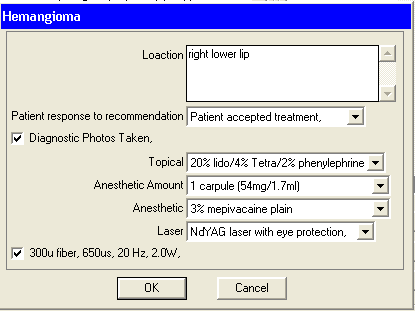
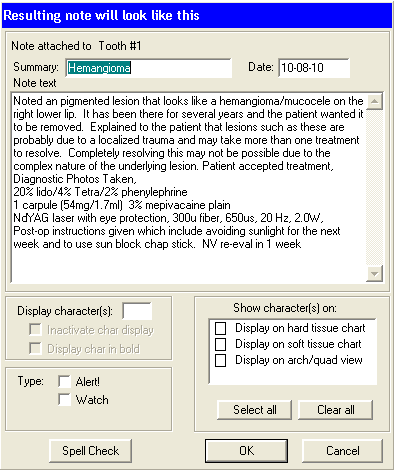
Notice the new type of variable called the “Text – multi line” used as the first variable to give you more room to explain just where this lesion is on the patient. Also looking at this note I decided to edit it to make it look more complete by adding more laser settings: 300? fiber, 650?s, 20Hz, 2.0W ( which are the settings I use on my PowerLase AT for this type lesion (see the blog on Hemangioma removal).
Made a “Check box” variable called <Laser3> and placed it right after <laser2> (with a space between) with ” 300? fiber, 650?s, 20Hz, 2.0W”.
See how easy that was to edit. I actually add to notes all day long in between patients as needed.