Dental patients are extremely fortunate to live in an era that more and more dentists are providing dental implants. No longer do we have to settle for a fixed or removable partial denture or complete denture to replace a single tooth or multiple teeth.
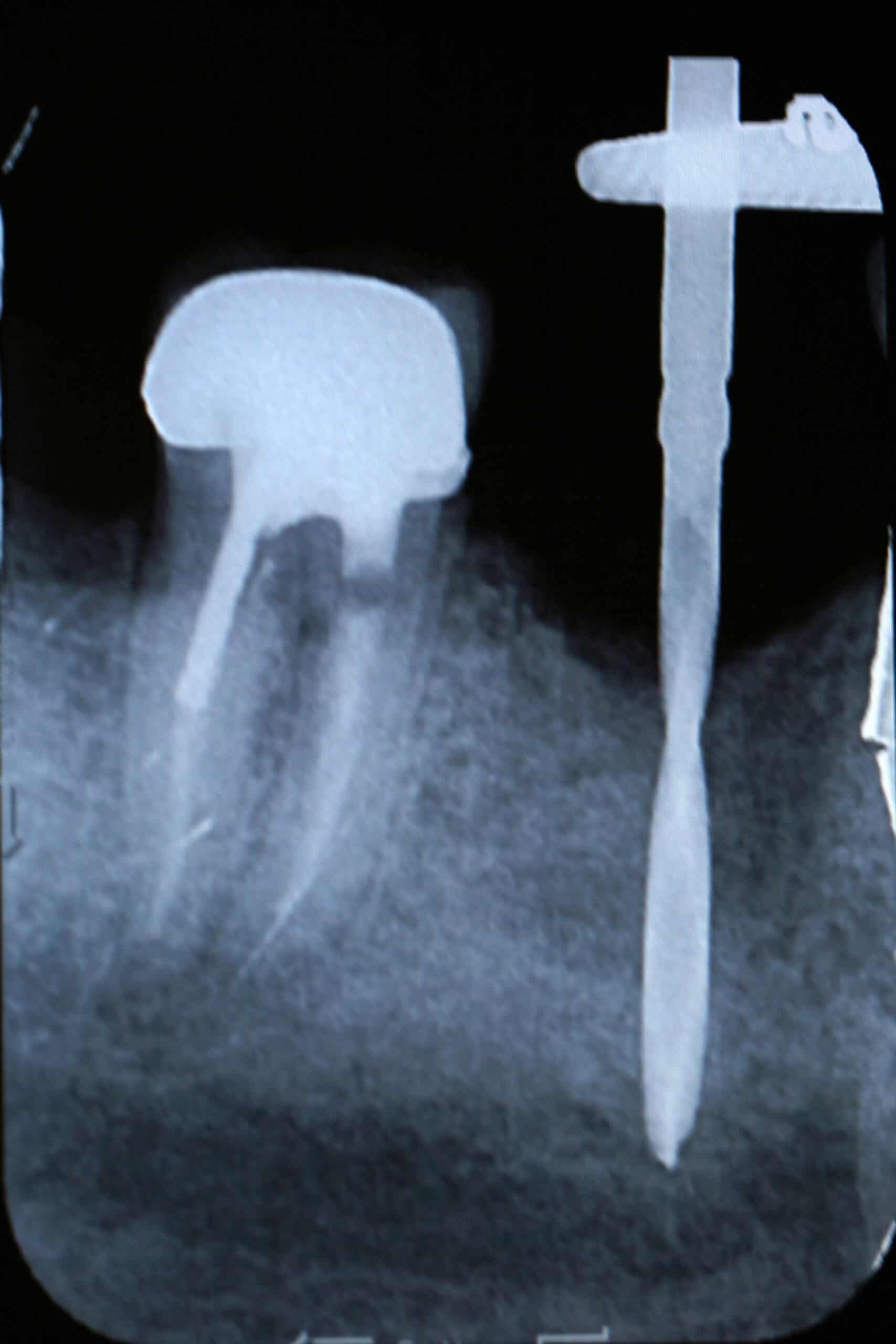
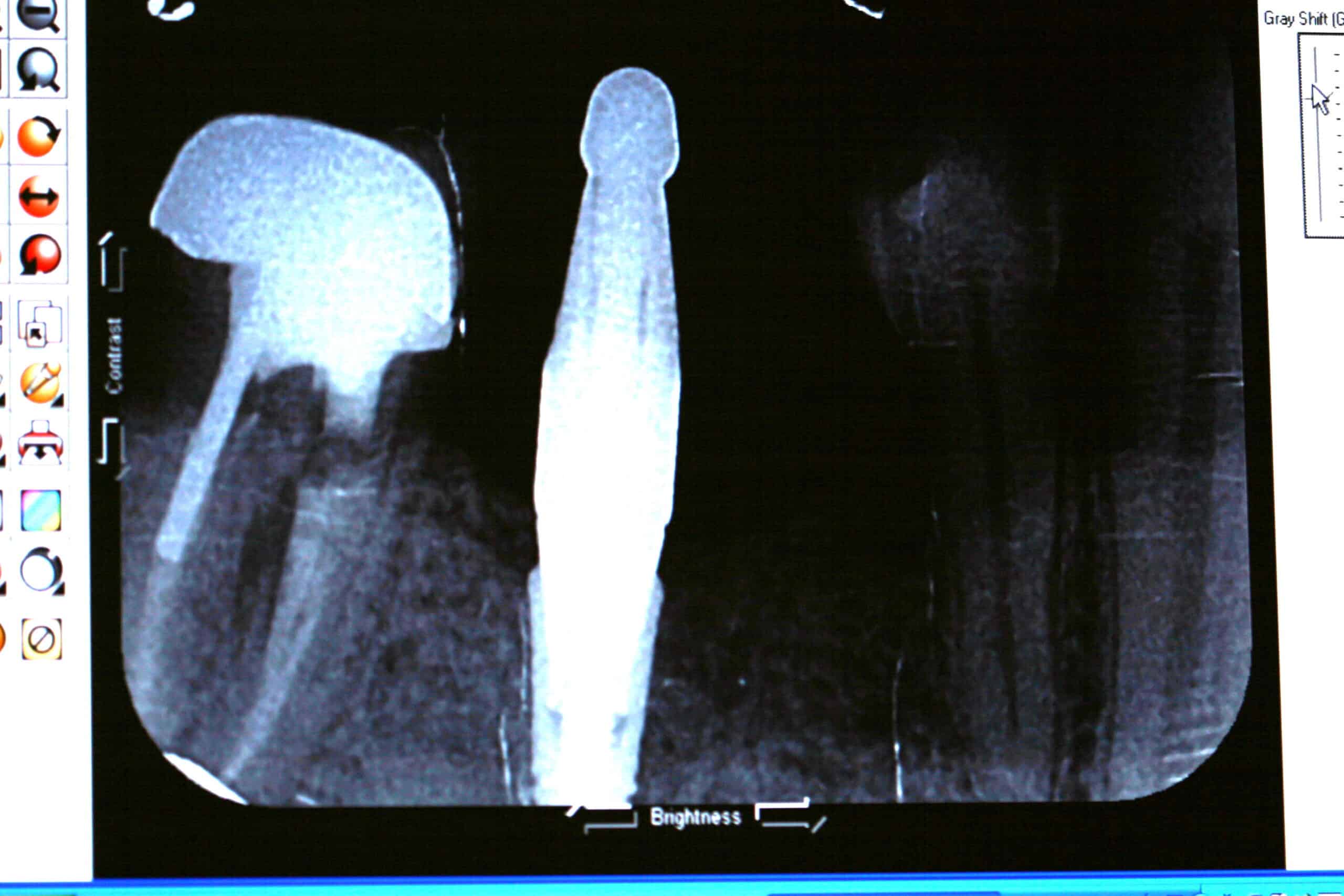
51 y/o/w/m with chief complaint of swelling on facial of #30. Health history was unremarkable. Noted failing endodontic filling, periodontal disease (perio probing 12+mm on facial furcation without purulence), large periapical pathosis, with possible vertical root fracture. It was given a hopeless prognosis, and slated for extraction with a bone graft for future implant placement.
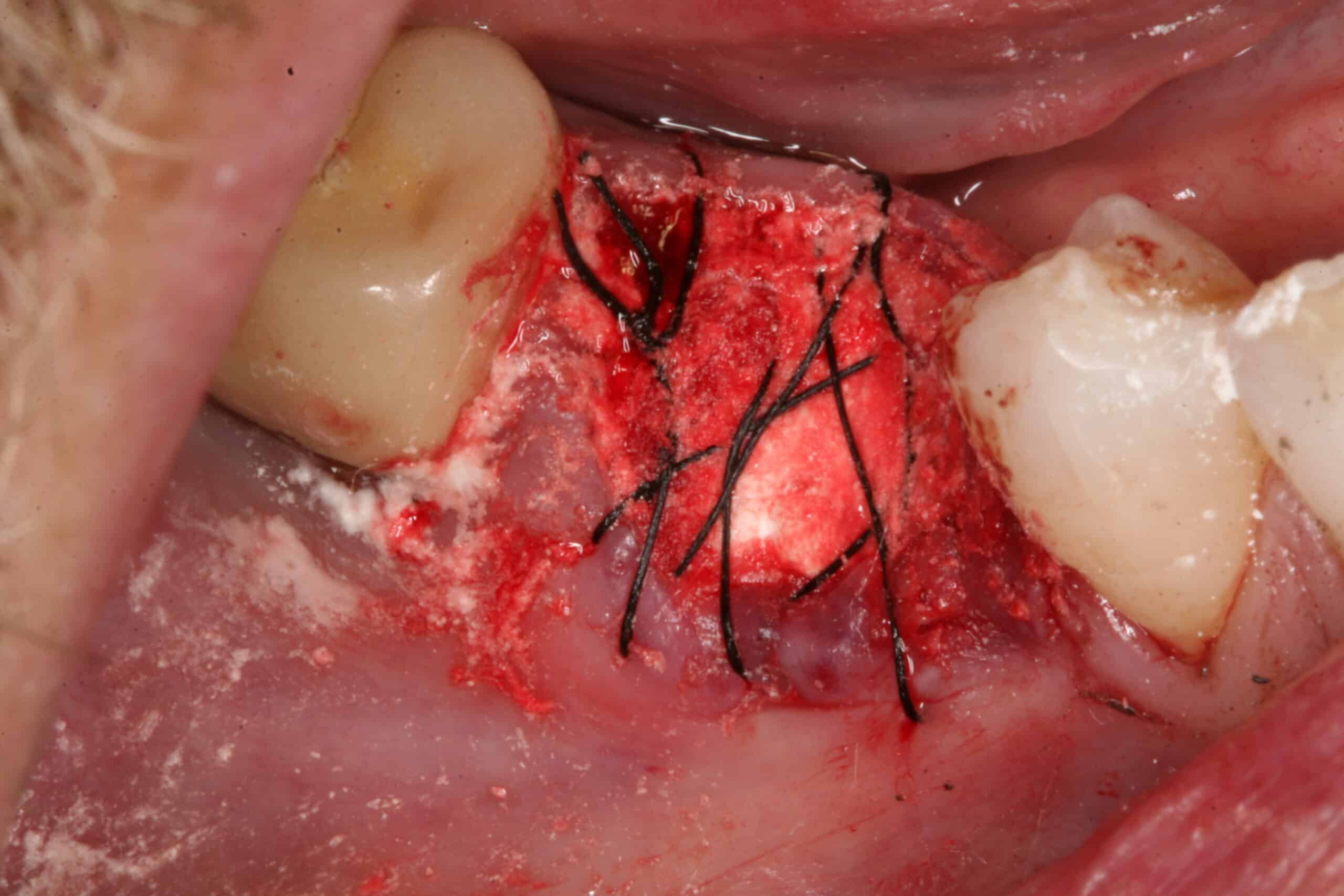
Extraction note as it appears in the chart are in BOLD: (Note: The bottom of this socket is bare bone because the granulation/cyst peeled out very nicely)
This tooth was extracted c/o patient request, periodontal disease, failing ENDO, abscess, non-restorable, Reviewed health history, Explained the informed consent to the patient and prompted question, pt decide to have socket graft(s), surgical extraction, 5 wall boney defect, sectioned roots, decorticated, DynaBlast, sterilized calcium sulfate, CollaTape, secondary closure, 5.0 black silk suture, Oral Hygiene Instructions, Treatment was tolerated well. Topical anesthetic 20% lido/4% Tetra/2% phenylephrine with 1 carpule (36mg/1.7ml) of mandibular nerve block, additional anesthetic used 1 carpule (68mg/1.7ml) 4% Articaine w/1:100000 epi infiltration, Blood Pressure 124/80, Pulse 73. Next Visit: Post-op
The patient was informed that immediately after the extraction their tongue/lips maybe numb. This is the time to stay quiet, keep your blood pressure down by limiting physical exertions, and try not to disturb the forming clot(s). Do not eat food until your lips/tongue are un-numb or you can cause severe trauma by chewing the lips and tongue. Do not drink carbonated beverages such as cokes or beer as this may fizz out the forming clot(s). Alcoholic beverages are to be avoided because they can dissolve out the clot and can cause your pain medication to be much stronger than it is intended. Combinations of narcotics and alcohol have lead to respiratory arrest and death. Leave the gauze in your mouth for 30-45 minutes. Bite on it firmly but do not chew it. The gauze is supposed to get wet with blood and saliva so don’t “milk the clot” by changing it frequently. This will disrupt the clot formation and cause continued bleeding.
Generally, you can eat anything you want to eat after an extraction. Cold foods are better than hot because hot will increase the blood circulation in the mouth and may cause bleeding. Hard foods may be difficult to chew. Do not bother with food being lodged into or near the socket(s). The body will push it out on its own. Flushing it out yourself will disrupt the clot and may cause a “dry socket”.
Avoid rinsing your mouth for 24 hours and DO NOT use mouthwashes or peroxides. Many mouthrinses contain alcohol and can affect the clot.
CALL the office if you have any post-operative complications or need to ask a question about how to take care of yourself.
If prescribed an antibiotic, that them until they are all gone. Doing otherwise may cause recurrent infections and/or cause antibiotic resistent bacteria to populate your mouth.
I like to suture the membrane into place so it is not lost a day or two later. The calcium sulfate is an additional “membrane” type covering over the bone and helps promote angiogenesis.
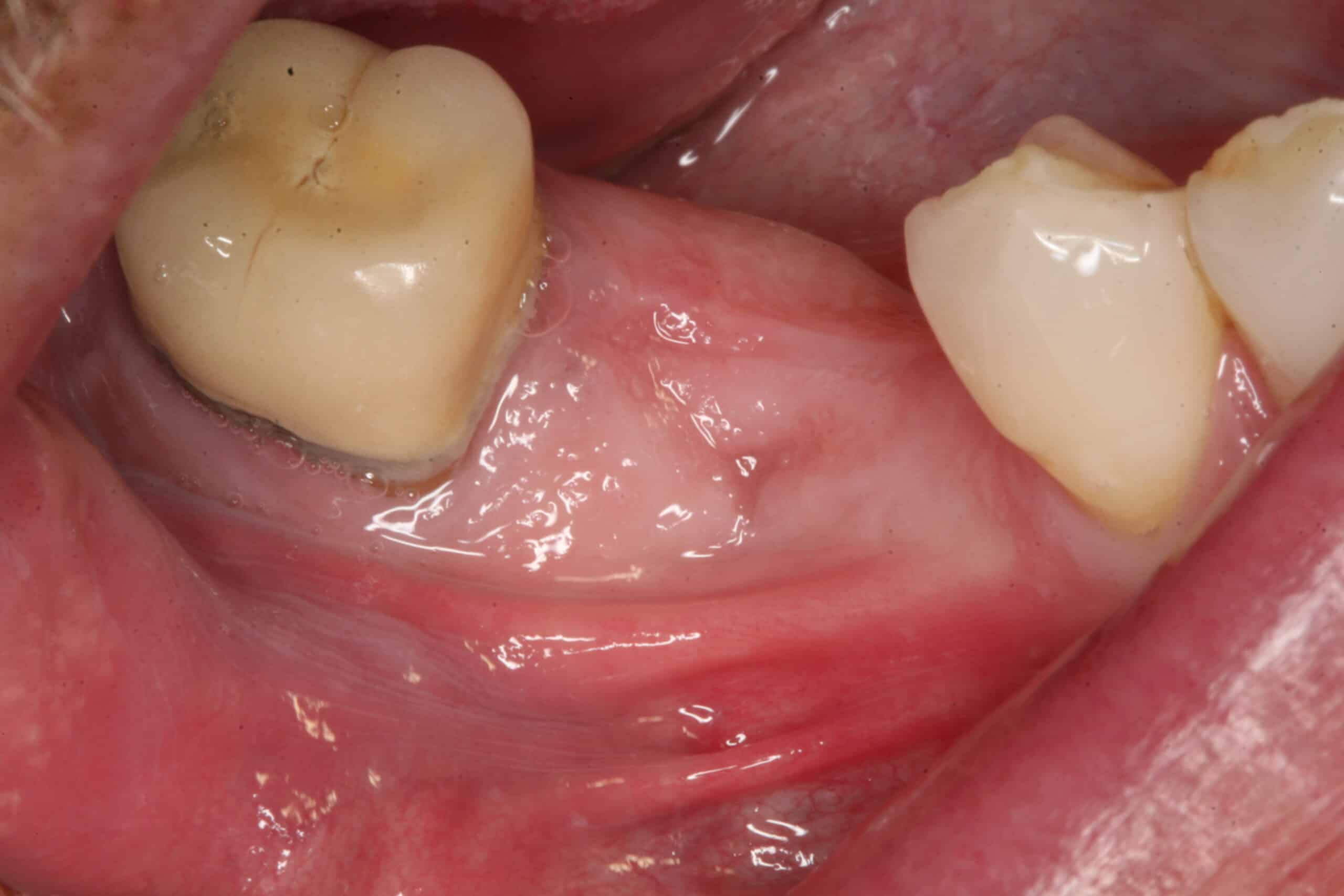
5 month post-op.
Note that the lingual plate is higher than the facial so when the implant measurement is made you may think you have more bone than you actually do on a panograph film, so be careful!
The patient has expressed the the desire to have dental implants. Reviewed health history, and found nothing to be complicating factors. The patient was placed in ASA 1 and accepted as a candidate for implants. Pre-op pano with 5mm measuing ball show the bone height was 15mm.Bone evaluation: Good width/height. Risks, benefits and alternative discussed.The patient was instructed to call the office if they are to having any questions. Next Visit: Implant Placement

5 mm measuring ball placed in mouth with bite registration material to help calibrate the pano distortion.
Pilot drill PA to make sure the orientation and depth is correct.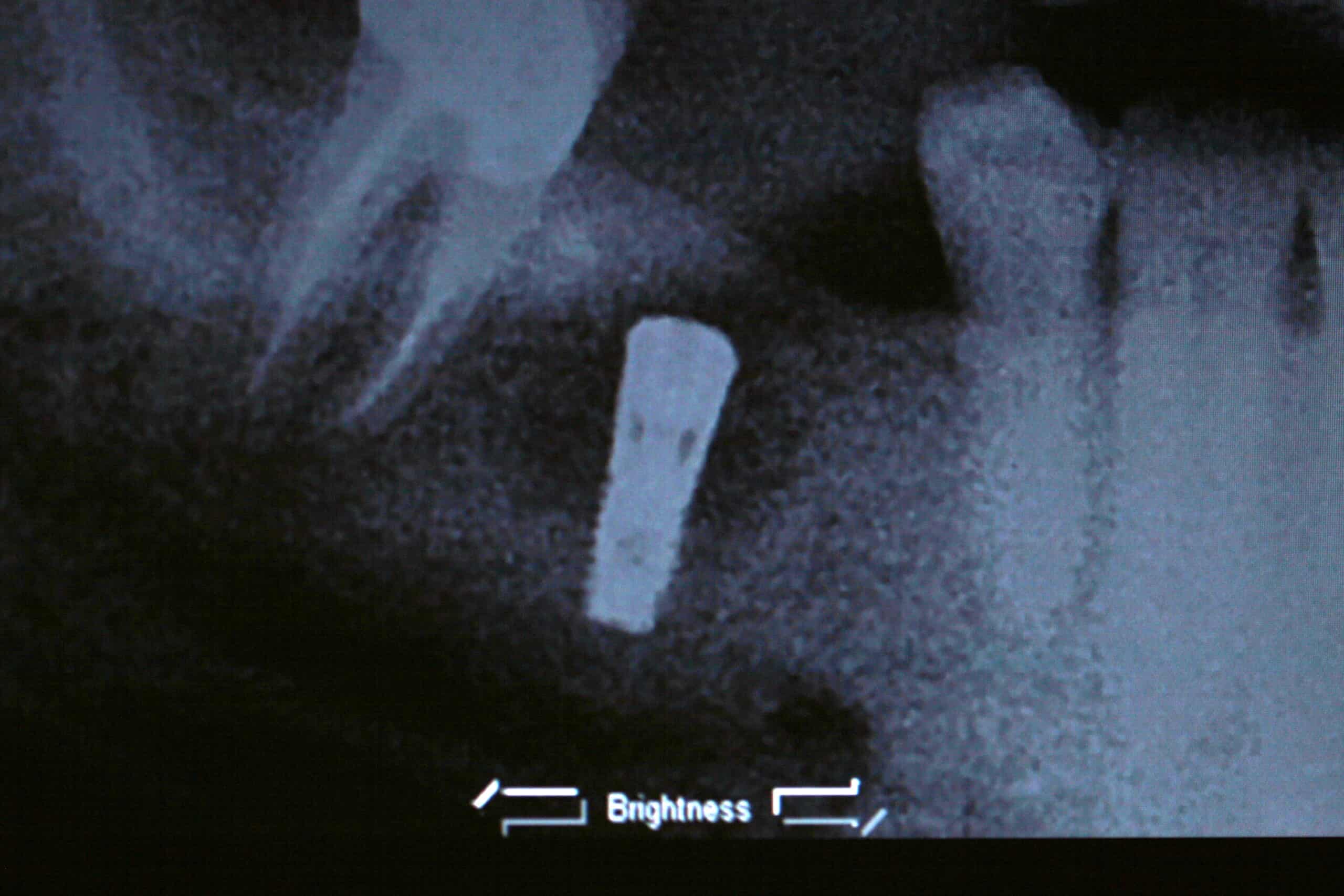
The implant looks like it is too deep, but this is because the lingual plate is higher than the facial plate.
Informed Consent, Reviewed health history, Skin/Mouth Prep-betadine & peridex, Elevated full thickness flap, sterile saline, Astra OsseoSpeed 4.5 X 11mm in #30 area, Type 3 bone, bone level implant cover screw, DynaBlast, CollaTape, 5.0 black silk suture, Mid-surgery PA, Post-op Pano, Oral Hygiene Instructions, Topical anesthetic 20% lido/4% Tetra/2% phenylephrine with 1 carpule (36mg/1.7ml) of 2% Mepivacaine/1:20,000 NeoCobefrin infiltration, Pt informed not to eat food, bite or chew on lips or tongue while anesthetic is still working. Treatment was tolerated well. Next Visit: Suture removal in 1 week
X-ray verification that the impression pin is seated correctly before the impression is made for the custom abutment. Today we skip this step by using a scanning pin and go from uncovering to placing the custom abutment and crown at one appointment.
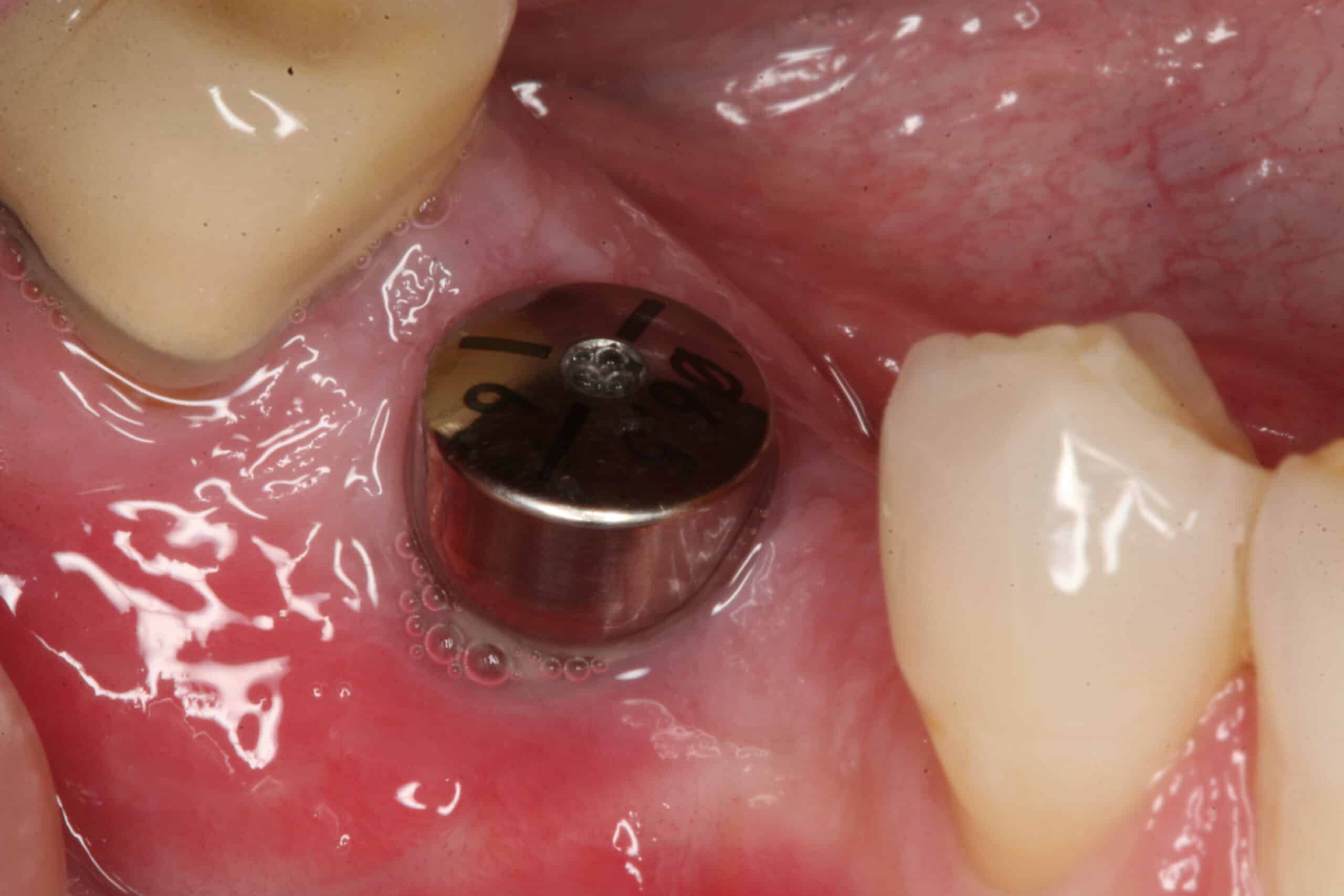
Reviewed health history, Topical anesthetic 20% lido/4% Tetra/2% phenylephrine with exposed implant with laser, Er:YAG with eye protection, (600us, 200mJ, 20Hz, R02/dry), removed healing cap, placed transfer pin(#30), implant sound good, x-ray verification, Poylvinyl Siloxane Impression, MegaBite, Opposing arch impression, healing collar Astra 4.5/5.0 6.5-6mm, Oral Hygiene Instructions, no local anesthesia, Next Visit: place CAD/CAM, iTero
Healing collar is placed until the custom abutment is back from the lab.
Titanium custom abutments are micro-etched before placed in the mouth to be scanned. This breaks up the reflectivity of the shinny metal making it scan better.
X-ray verification to make sure the custom abutment is placed all the way into the implant before torquing it into place.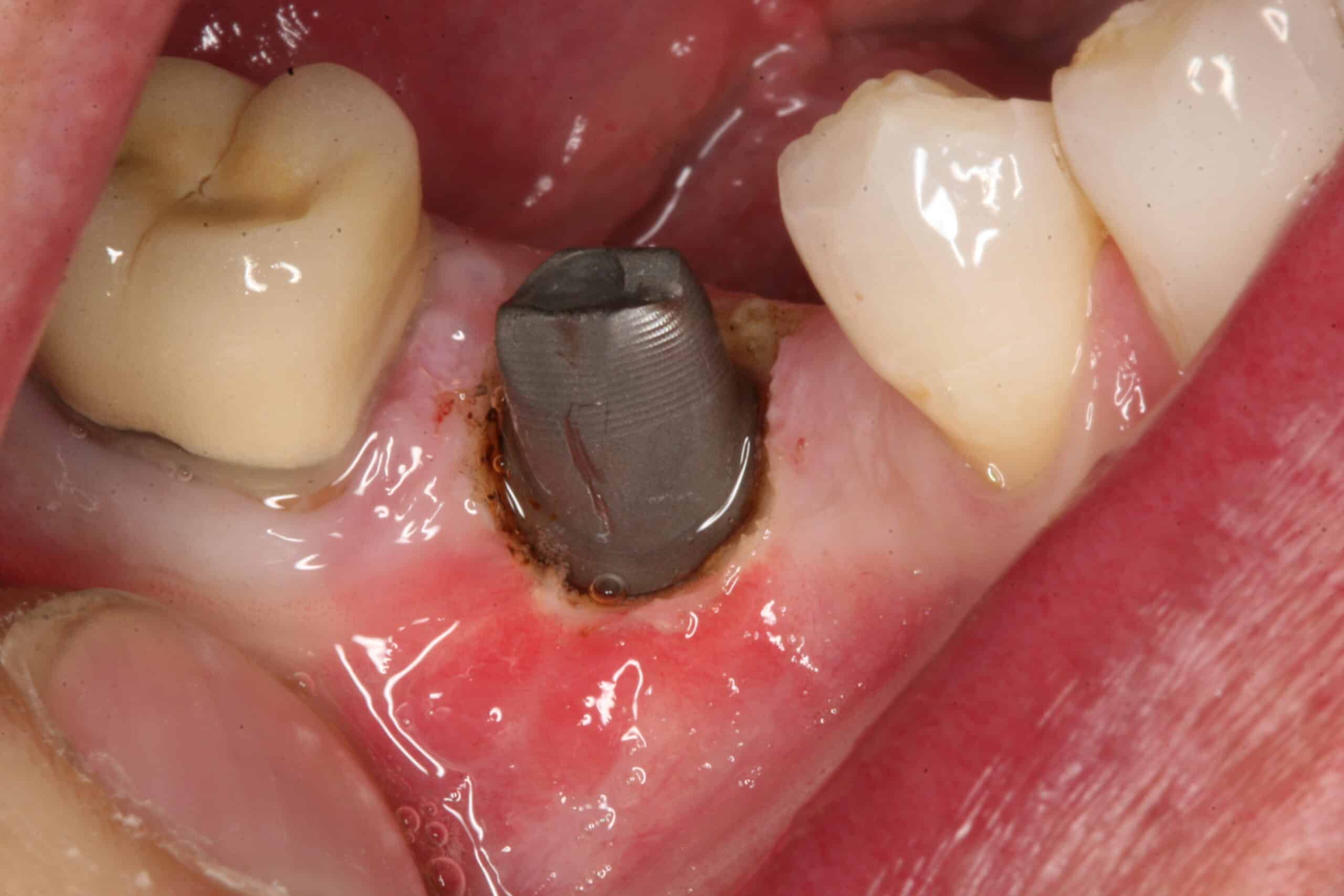
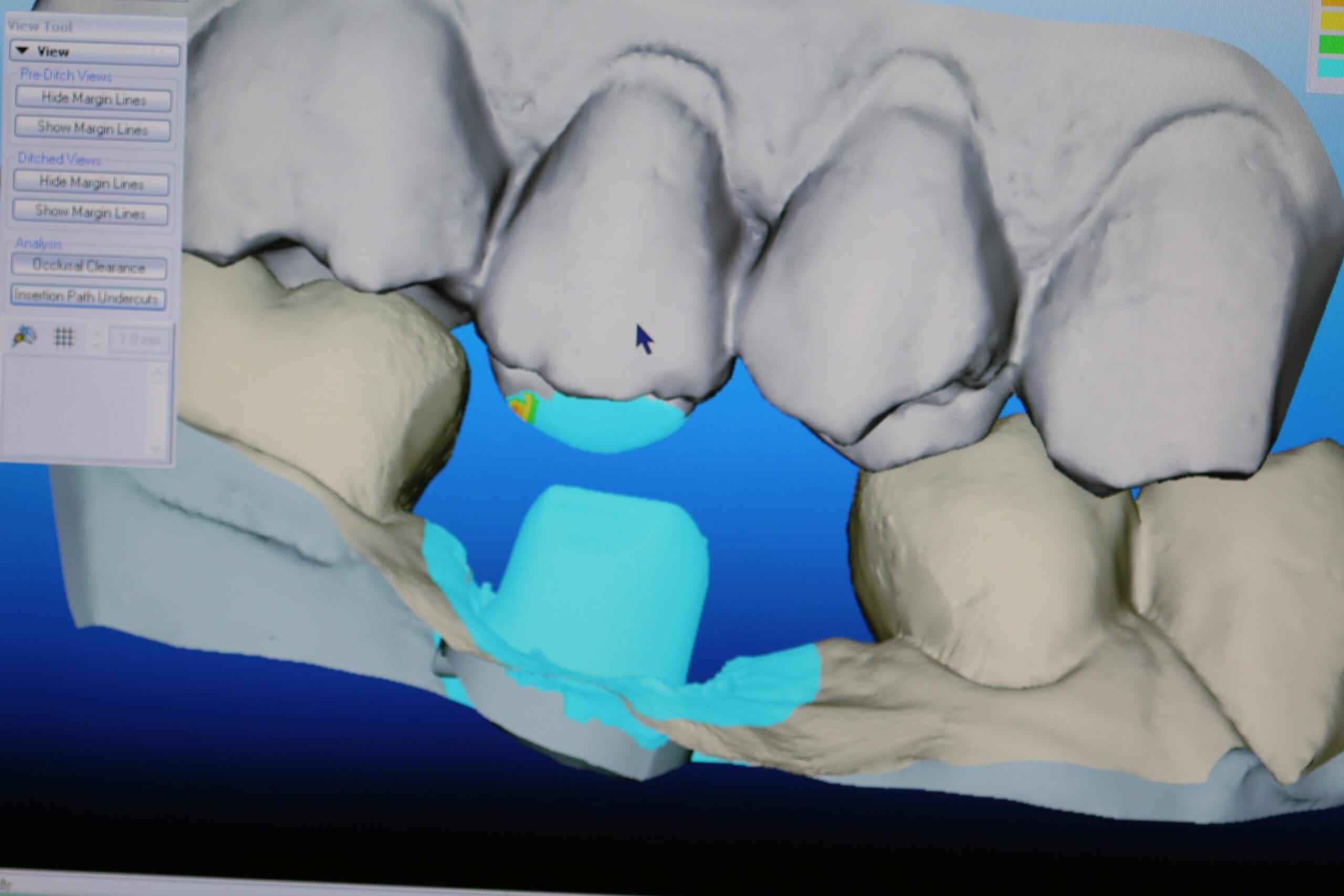
Diode laser around the neck of the custom abutment to prepare it for scanning with the iTero machine.
Reviewed health history, Removed healing collar, micro-etched Ti abutment to decrease reflextivity, placed CAD/CAM abutment, x-ray verification, torqued down abutment 25 Ncm, Fermit-N in screw holes and prep’d CAD/CAM abutments, H2O2, viscostat, diode laser with eye protection, iTero digital scan, virtual bite, Temp crown made and cemented with tempBond, tolerated well, OHI, Topical anesthetic 20% lido/4% Tetra/2% phenylephrine with 1 carpule (68mg/1.7ml) of 4% Articaine w/1:100000 epi
Pt informed not to eat food, bite or chew on lips or tongue while anesthetic is still working. Next visit: cement crown
The tissue has healed very well around the custom abutment after 2 weeks.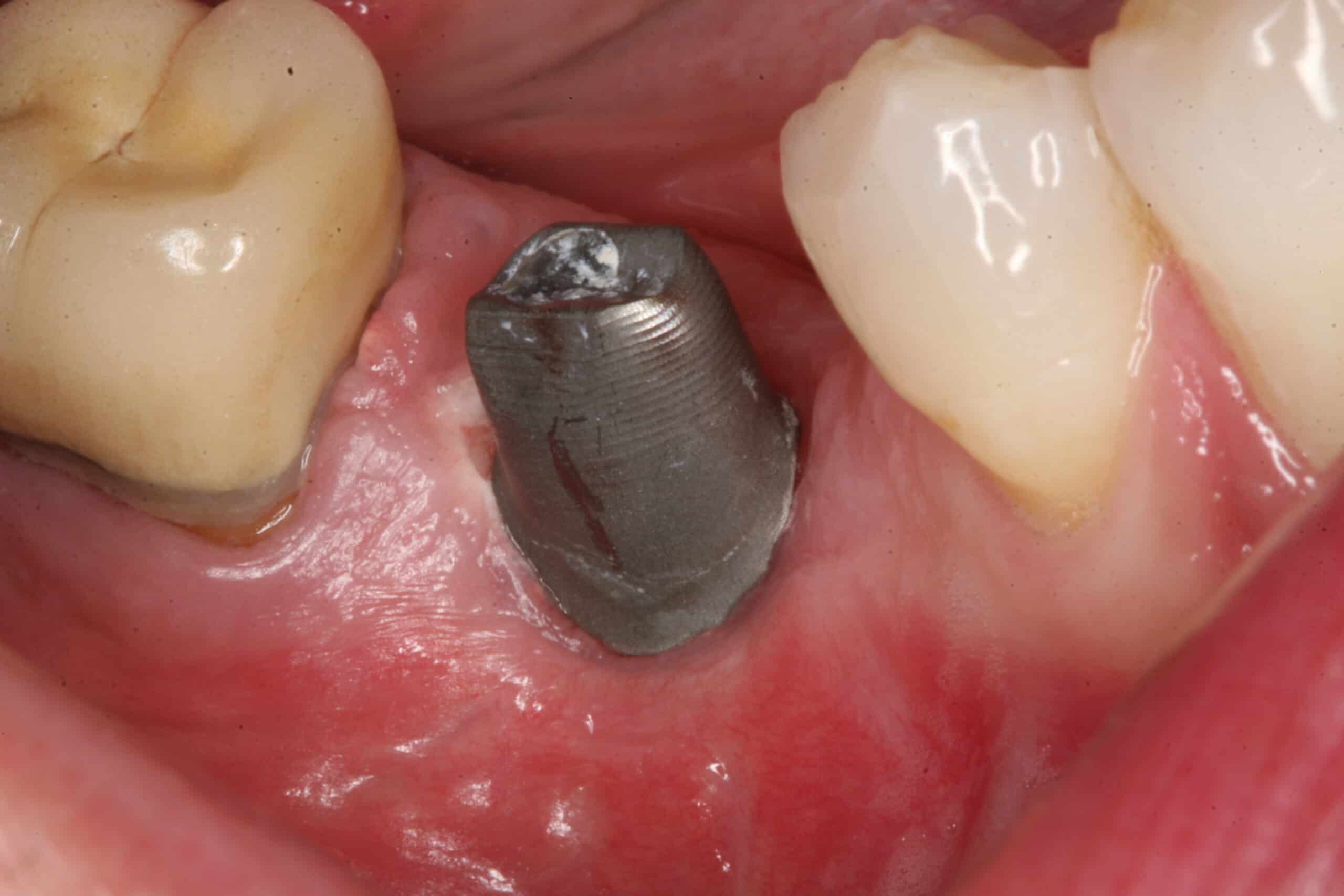
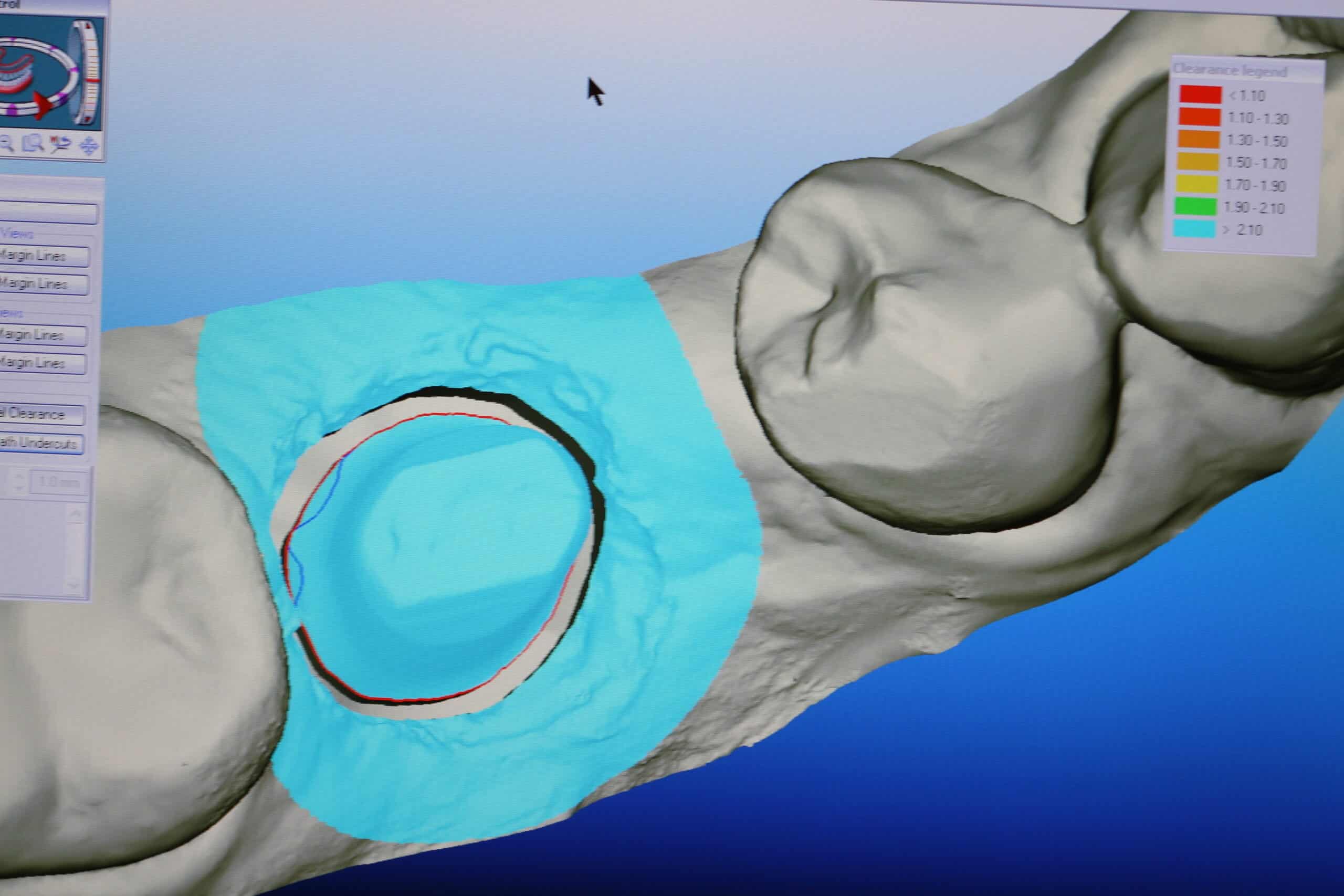
Final cementation with good interproximal and occlusal contacts at heavy grinding forces without having excessive occlusal adjustments.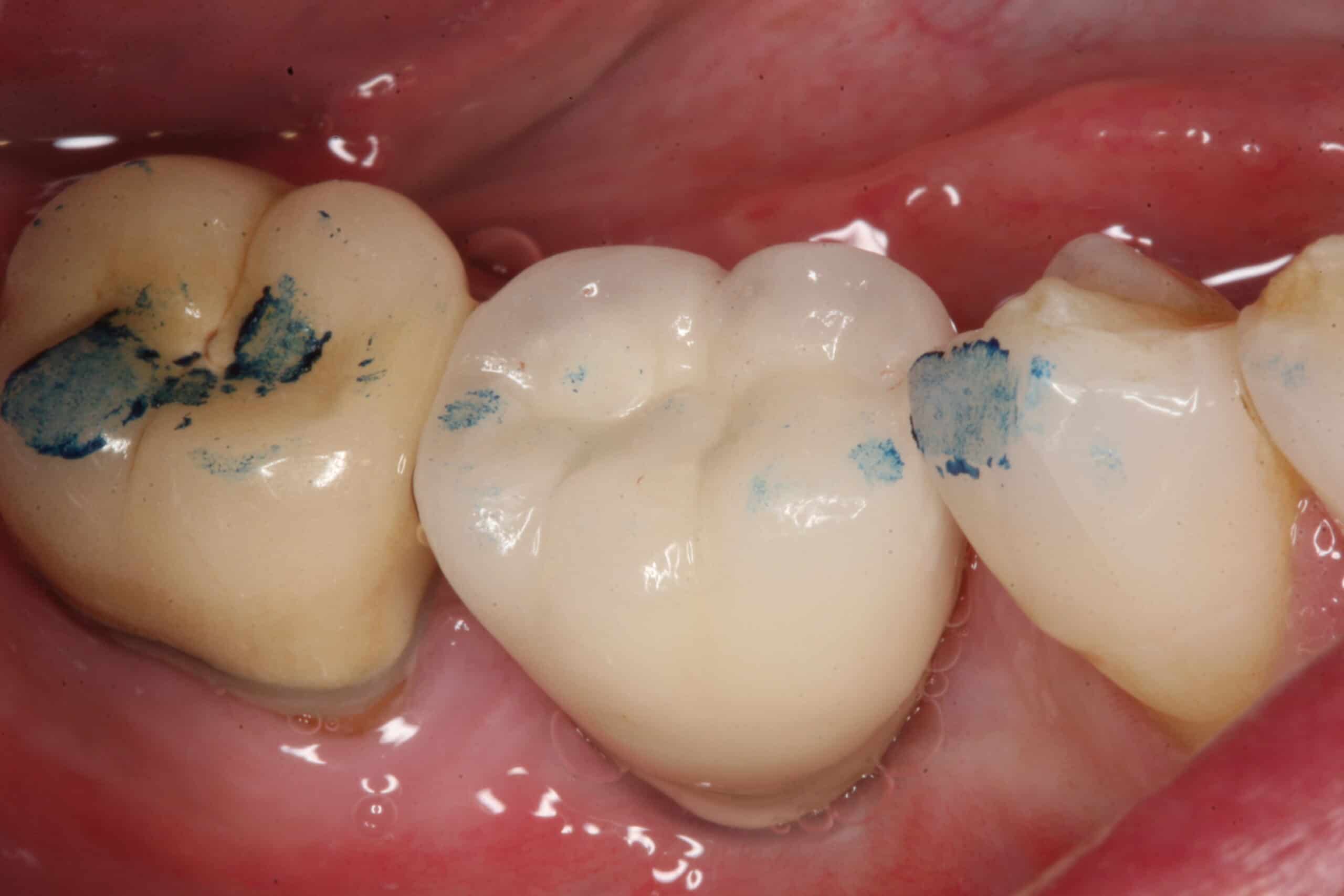
Temporary Crown was removed and abutment cleaned, Only slight occlusal adjustments needed, the patient approved the aesthetics and occlusion, Hydrogen Peroxide, Cemented Crown with Rely-X, Oral Hygiene Instructions, Next Visit: Recall
Identalloy: The manufacture certifes that the dental casting alloy provided to the laboratory is predominatly base alloy (contains less that 25% total of gold, palladium, platinum).
Alloy: EOS CoCr SP2
Manufacture: EOS of North America, Inc.
Composition: Co 63.8 wt%, W 5.4 wt%, Cr 24.7 wt%, Si 1.0 wt%, Mo 5.1 wt%.
This is at 16% maximum force. #30 is at the #3 position on this graft.
This is at maximum force.
Now when #31 finally fails he will know what to look forward to… By then we will have our CBCT installed, and will skip a step with the scanning transfer pin.