As a general dentist I have never been hugged by so many grown men and women as I have after delivering a mini dental implant (MDI) retained lower complete denture. MDI’s can be used for many other restorative procedures, but it really works well retaining a lower complete denture to the atrophic lower ridge. I started placing MDIs after seeing my old high school next door neighbor and later dental school classmate (Boomer Sooner!) on the cover of DentalTown back in 2000. Ron Bulard, DDS started a company called Imtec  that he later sold to 3M (way to go Ronny!). While practicing in Manhattan, NYC he teamed up with a doctor/inventor named Dr. Sendax and started manufacturing the MDI’s in Ardmore, Oklahoma (where Ron’s main practice was located).
that he later sold to 3M (way to go Ronny!). While practicing in Manhattan, NYC he teamed up with a doctor/inventor named Dr. Sendax and started manufacturing the MDI’s in Ardmore, Oklahoma (where Ron’s main practice was located).
I was not placing implants at that time, just restoring them. Not sure why I wasn’t placing them, but I think it had something to do with my externship that I took between my 3rd and 4th year of dental school. I was paired with an oral surgeon who had a reputation for not placing implants, “I only take them out”, I can still remember him saying.
Oh well, after reading about Imtec in DentalTown, mini dental implants sounded like a great treatment option for my patients. So I immediately enrolled in an Imtec sponsored course put on by Dr. Todd Shatkin in Buffalo, NY. The course was amazing! Todd has since moved onto Intra-Lock MDL,  as have I, and I will touch on that later. The course included the usual gross anatomy, implant parts, and placement techniques. He used different kinds of wood to simulate the various types of bone (oak being type 1 and balsa being type 4 bone). The Imtec MDI is only 1.8mm in diameter and is made of some kind of titanium (can’t remember the exact alloy). During the course they did stress that these MDI’s can fracture if over-torqued during placement. Todd said that the first few cases a new dentist should try is immediate fixation of the lower denture with minimum of 4 MDI’s in between the two mental foramen. The dentist should then venture on to fixation of the maxillary complete denture with minimum of 5-6 MDI’s, and then finally to supporting a crown or FPD(obviously the hardest).
as have I, and I will touch on that later. The course included the usual gross anatomy, implant parts, and placement techniques. He used different kinds of wood to simulate the various types of bone (oak being type 1 and balsa being type 4 bone). The Imtec MDI is only 1.8mm in diameter and is made of some kind of titanium (can’t remember the exact alloy). During the course they did stress that these MDI’s can fracture if over-torqued during placement. Todd said that the first few cases a new dentist should try is immediate fixation of the lower denture with minimum of 4 MDI’s in between the two mental foramen. The dentist should then venture on to fixation of the maxillary complete denture with minimum of 5-6 MDI’s, and then finally to supporting a crown or FPD(obviously the hardest).
I had already ordered and received a complete surgical kit and assortment of MDI’s before the course, and wouldn’t you know it, first thing Monday morning back form Buffalo I had my very first case. It was on an 83 y/o/w/m who had a failing FPD #12X14. #12 had a very deep mesial pocket and hopeless recurrent decay. He didn’t want to have anything redone or a RPD because of his age. He just wanted it “patched-up” for the time he had left on this Earth. I was itching to put in my first MDI and thought I could tap off the FPD, extract #12 and retro-fit a MDI under the pontic to support the FPD. So that’s just what I did. This very same patient then disappeared from our practice for the next 8 years. He finally came in for a cleaning appointment, and complained to the hygienist that he didn’t like having to floss thread under his UL bridge. To my surprise during the exam I noticed that the bone had healed well in the #12 position, and the MDI under #13 pontic had good looking supporting bone around the MDI, and the whole FPD was solid as a rock. The patient was happy as long as he didn’t have to floss thread under his bridge!
Over the next few years I placed 100’s of MDI in just about every scenario you can imagine. Some good and some not so good and had only 5-10 break off as I was placing them in hard bone. Three in one patient that was type 1 bone everywhere. I started to notice other companies coming out with their own versions of mini dental implants and Intra-Lock (MDL) had a growing reputation of being less likely to break and had more options for restoring the tiny little implants, so I switched.
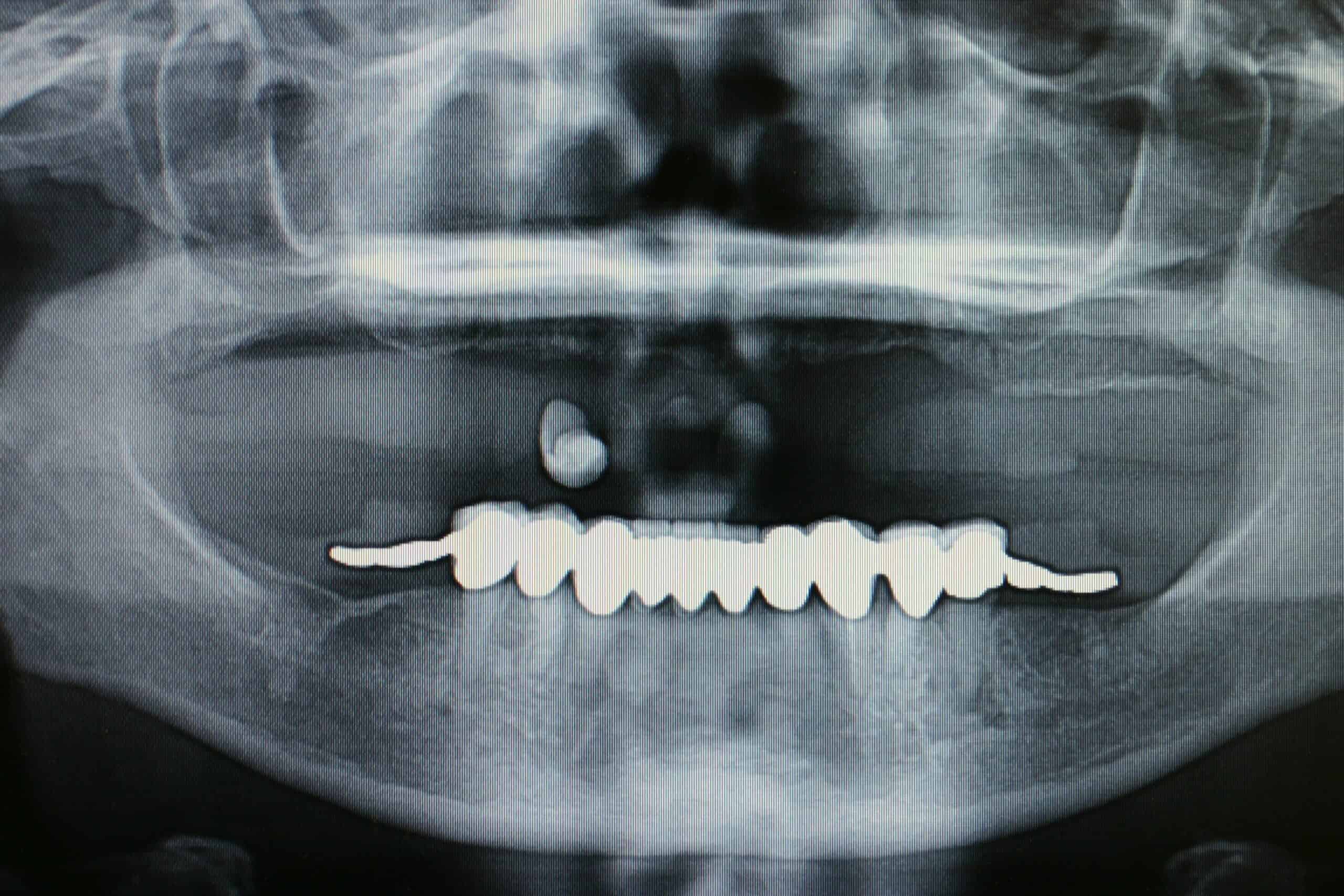
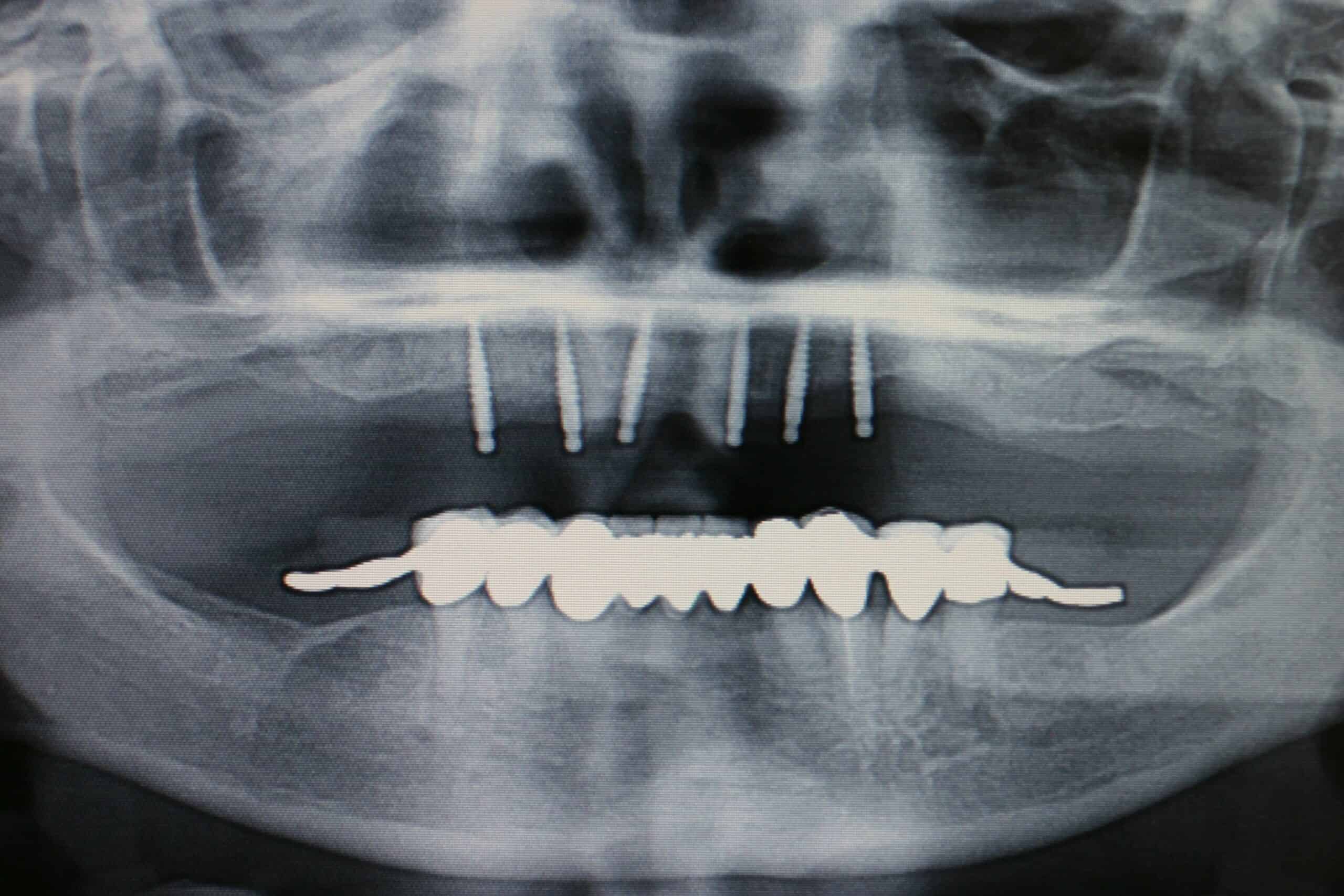
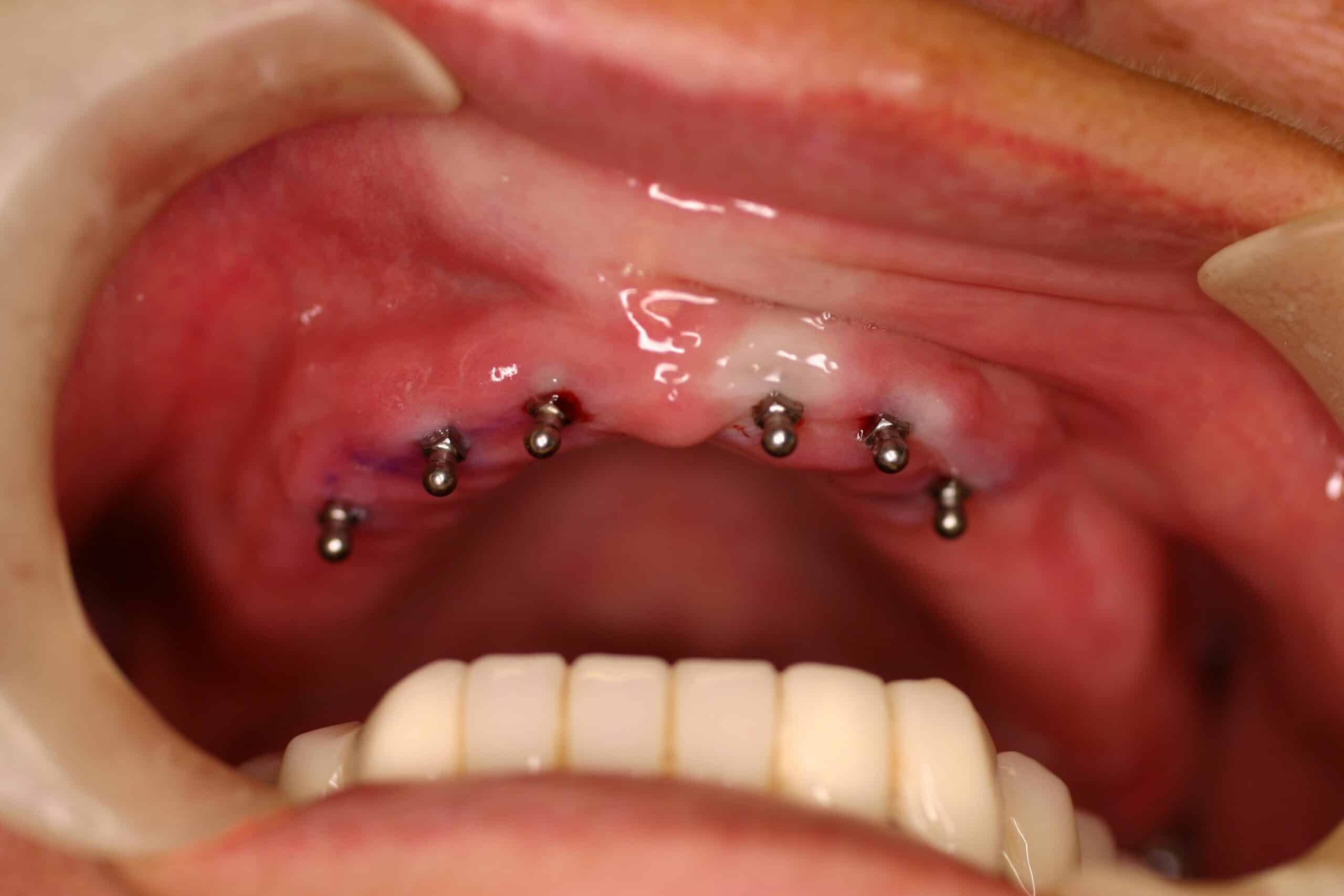
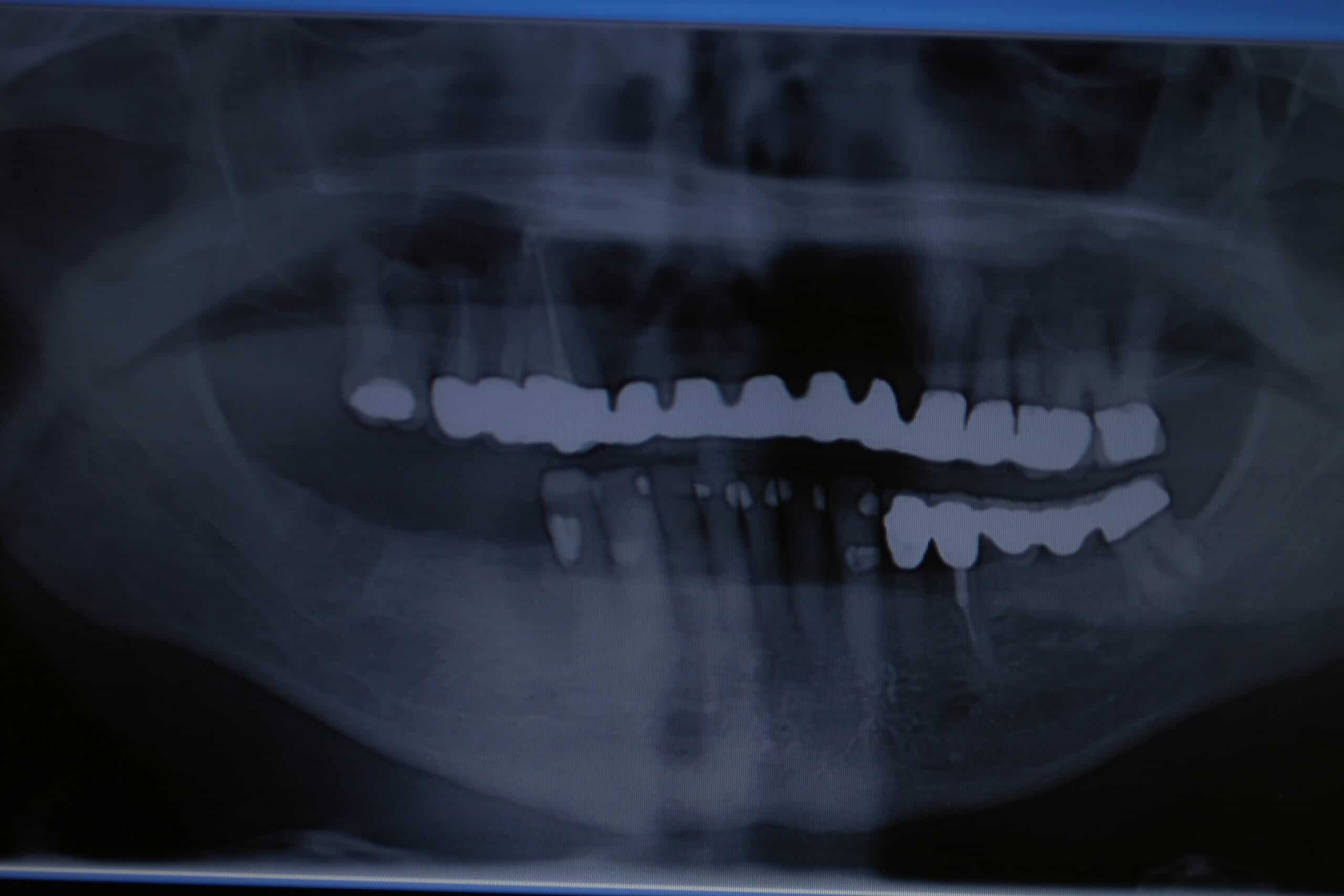
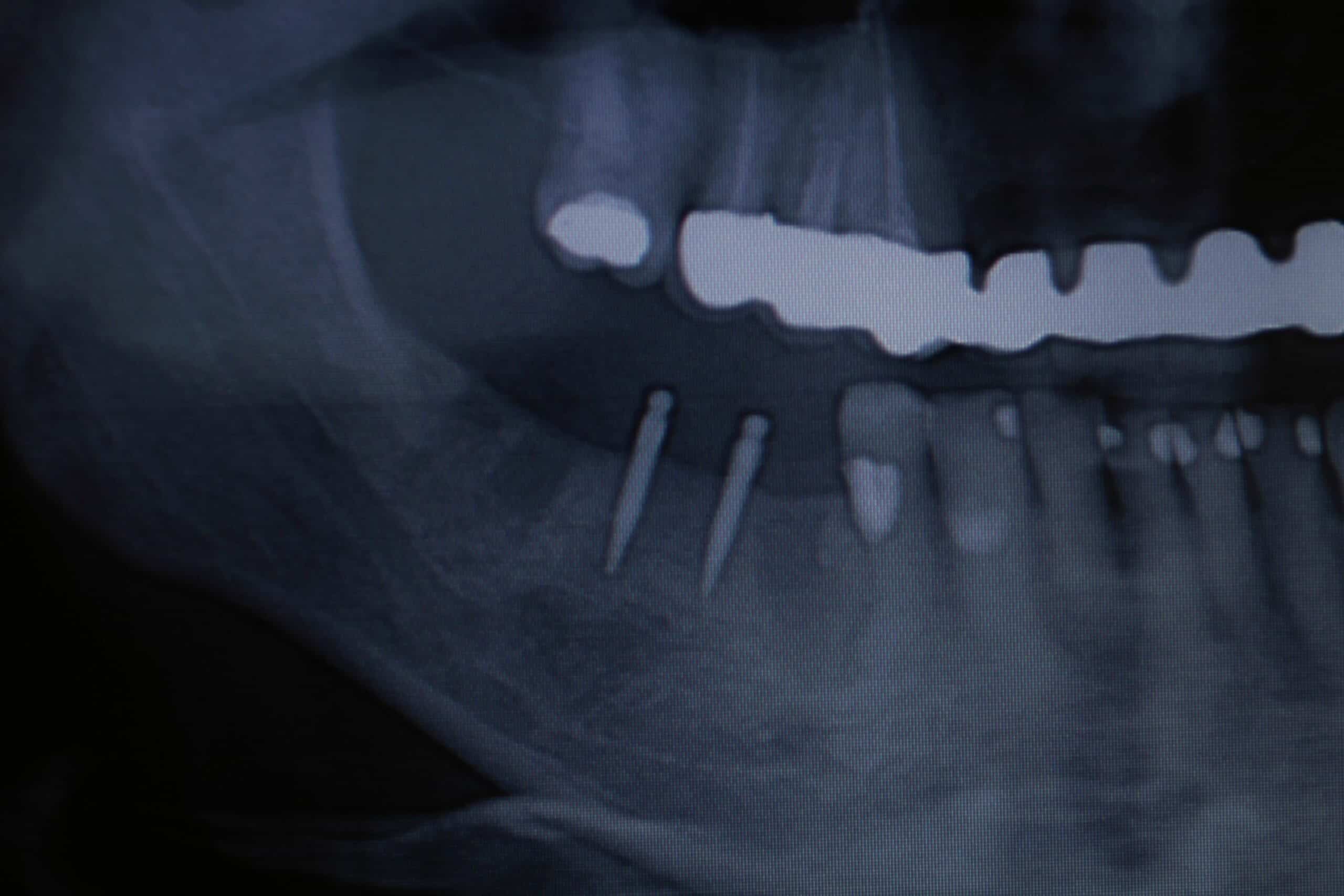
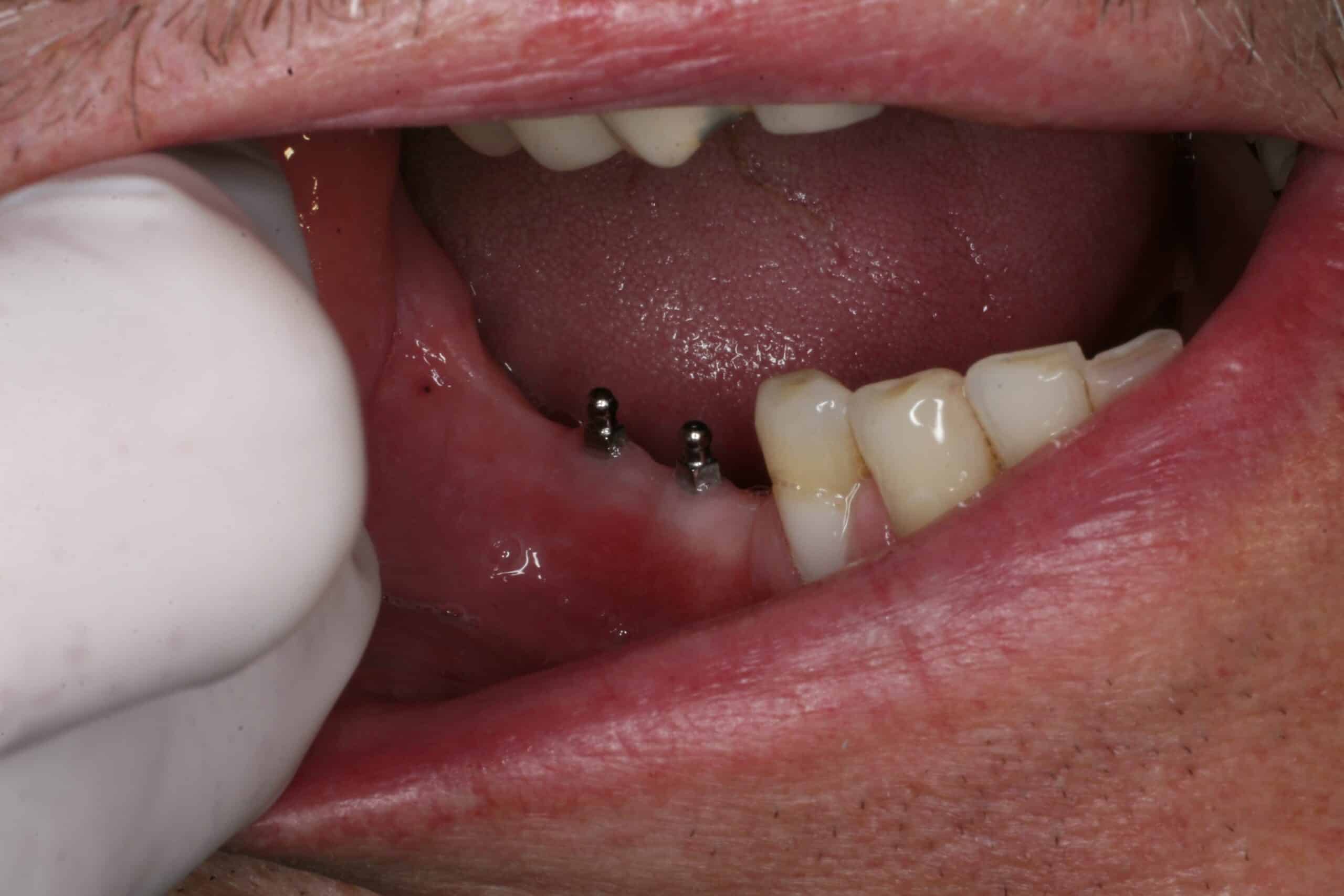
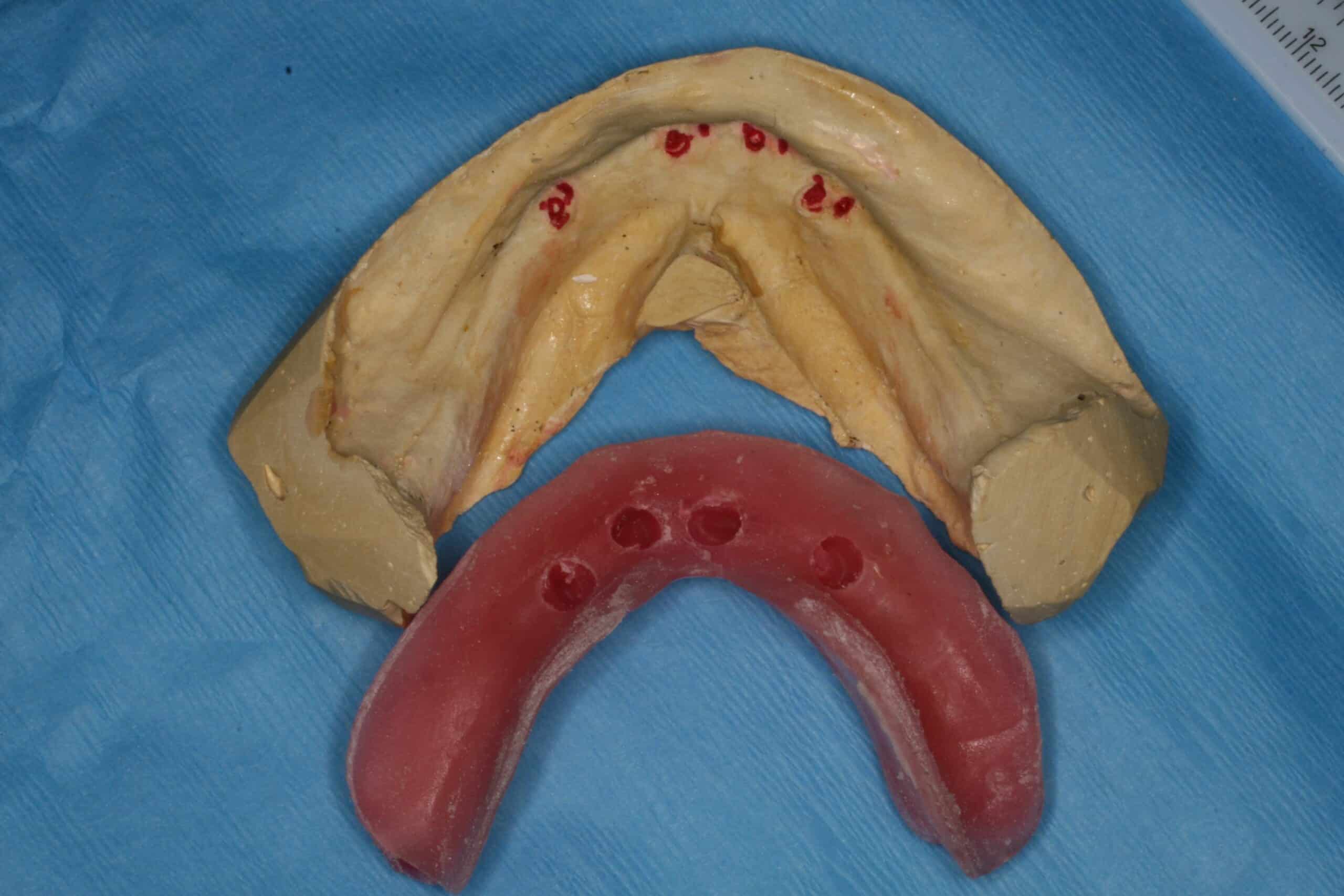
Since about 2008 we have still been placing 4 MDL on the lowers for /OD, but are placing the regular cylinder implants everywhere else. My reasoning for this is that they are placed in 1 day and the patient love them. During the initial exam we take a panograph with two 5mm measuring balls on the patients old denture around the mental foramen (we have recently switched to CBCT). A prescription for antibiotics and pain medication are written and they start taking the antibiotic the day before. Most of the time they do not need to take any pain medication at all, but feel comfortable just having it just in case. The patient is then reappointed for an 8:00am 1 ½ hr appointment with no sides. At that appointment the patient is prep’d and 4 MDL are placed in the anterior mandible between the mental foramen. Their lower complete denture is then hollowed out over the MDL heads sticking out of the gingival and a polyvinyl siloxane reline wash impression is taken to pick-up an impression of the implant heads. The denture is sent to our local lab along with 4 analogs and 4 snaps where they place the implant snaps in a full reline of the lower and return it back for delivery before 4:00pm that very same day. Most doctors pick up the snaps in the chair with acrylic themselves instead of adding the extra lab bill expense, but I find this way cuts down on the difficulty/stress, and presents to the patient with a beautiful looking, easy to clean, relined case that fits great. At that point we deliver the denture, the bite is adjusted, give oral hygiene instructions that include not taking the denture out of the mouth for 5 days and to go home and eat! At the 5 day recall the denture is removed, cleaned and the patient is coached on how to place/remove the overdenture. An Access toothbrush is issued along with a fixodent  denture cleaning kit (minus the tube of Fixodent). We see them again at 1 week, and then prn with 6 month recalls. One con to this is that we are usually using the patients old denture, and the denture is usually already old by the time we reline the snaps into them. The patient is always informed that the denture will have to be remade at some point in the future.
denture cleaning kit (minus the tube of Fixodent). We see them again at 1 week, and then prn with 6 month recalls. One con to this is that we are usually using the patients old denture, and the denture is usually already old by the time we reline the snaps into them. The patient is always informed that the denture will have to be remade at some point in the future.
Most oral surgeons/periodontists/general dentist implantologists don’t like to place mini dental implants. They all have their different reasons. Some such reasons include they haven’t been trained, they tried some and broke an implant upon placement, and they are inferior to regular implants. I think it is harder for someone to begin placing MDI after they have learned to place the larger regular implants. They like the force and torques you can achieve with the large implants and don’t develop the feel you need to successfully place the MDI without breaking them. Also lining up the MDI within 10-15 degrees of each other free hand is very challenging without a guide. They would rather place 2 , 3 or 4 regular sized implant in the lower anterior mandible to fixate the lower denture to the mandible. I agree, regular sized implants are great to fix a lower complete denture to the lower mandible, no question about that. It is just that with MDI the patient can use their old denture, they can have them place in the same day at about ? the cost of regular implant fixtures. Also if a regular implant was to fail, then it can be a difficult extraction, bone graft and new implant that will take time to heal and expense to have re-fitted under the denture. If a MDI fails, then another can be quickly placed a few millimeters away and a new snap can be processed into the denture, all in the same day at minimal expense.
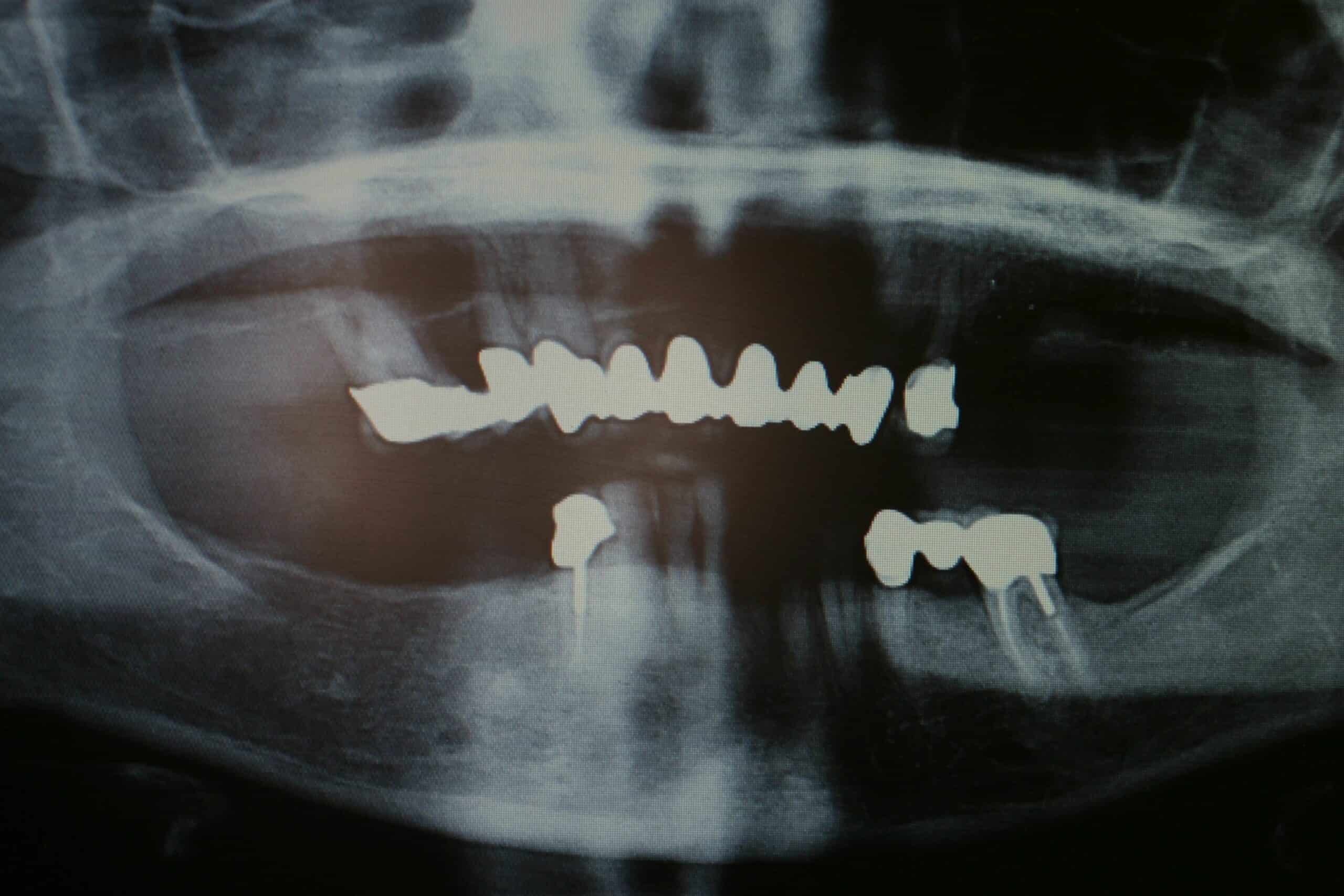
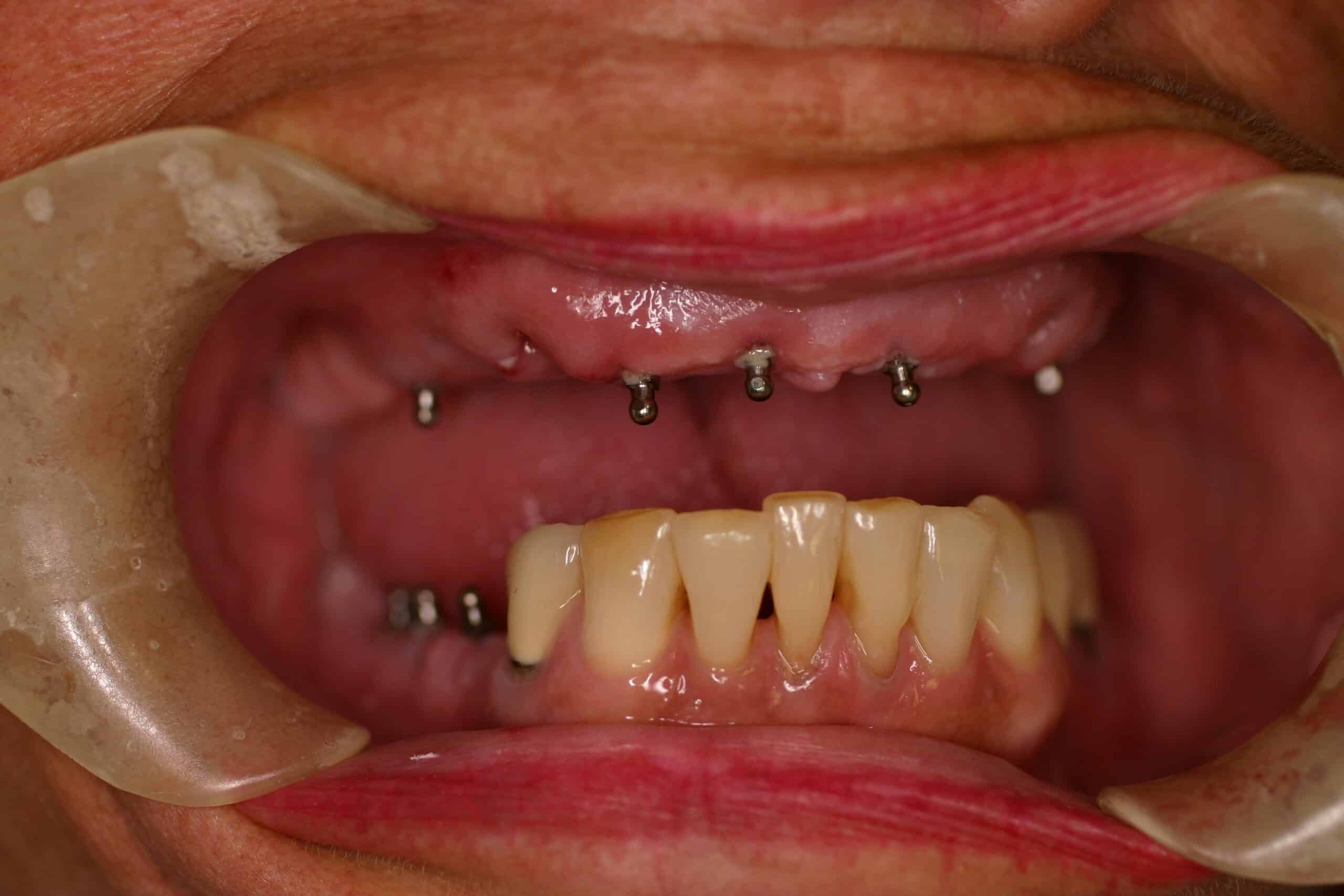
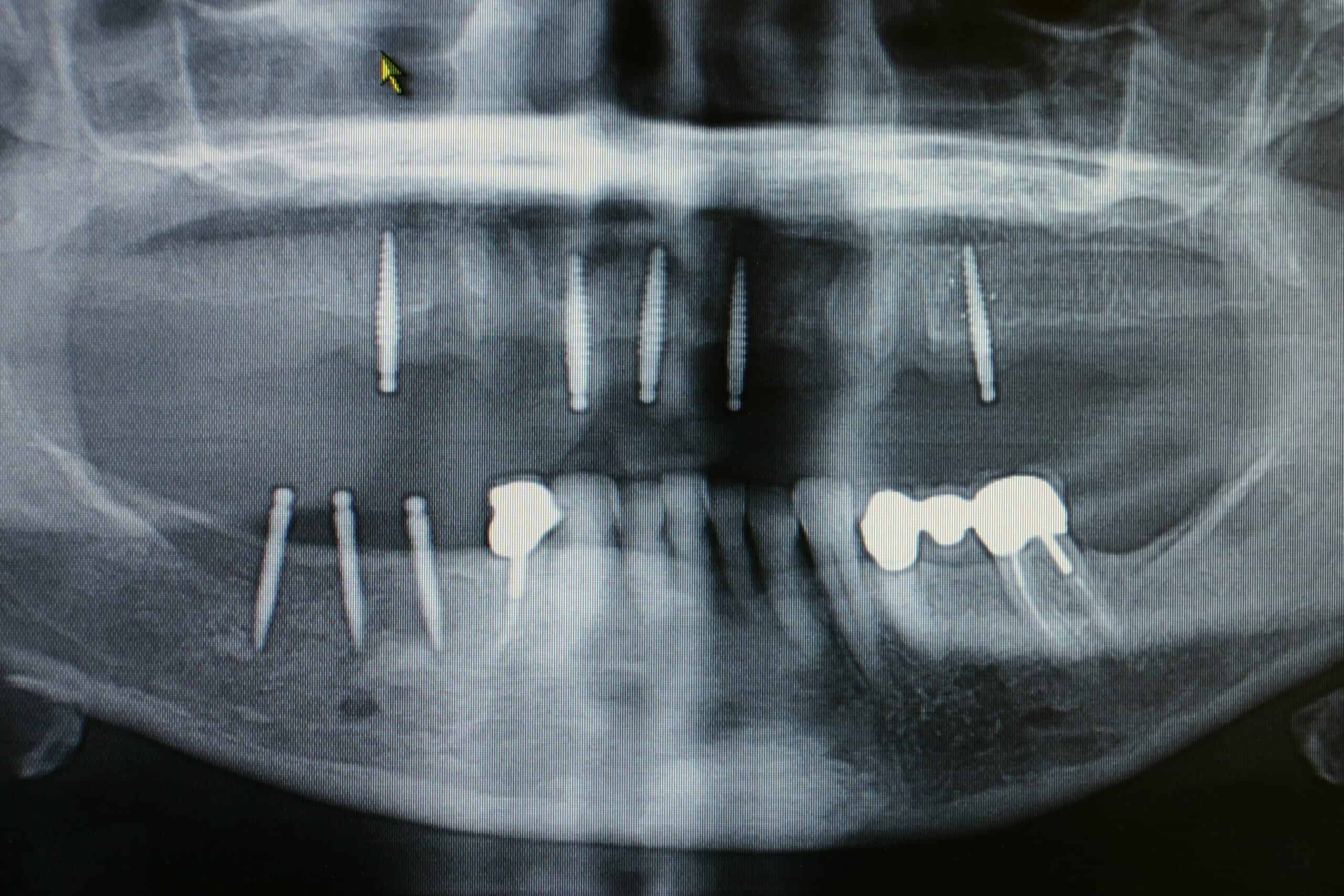
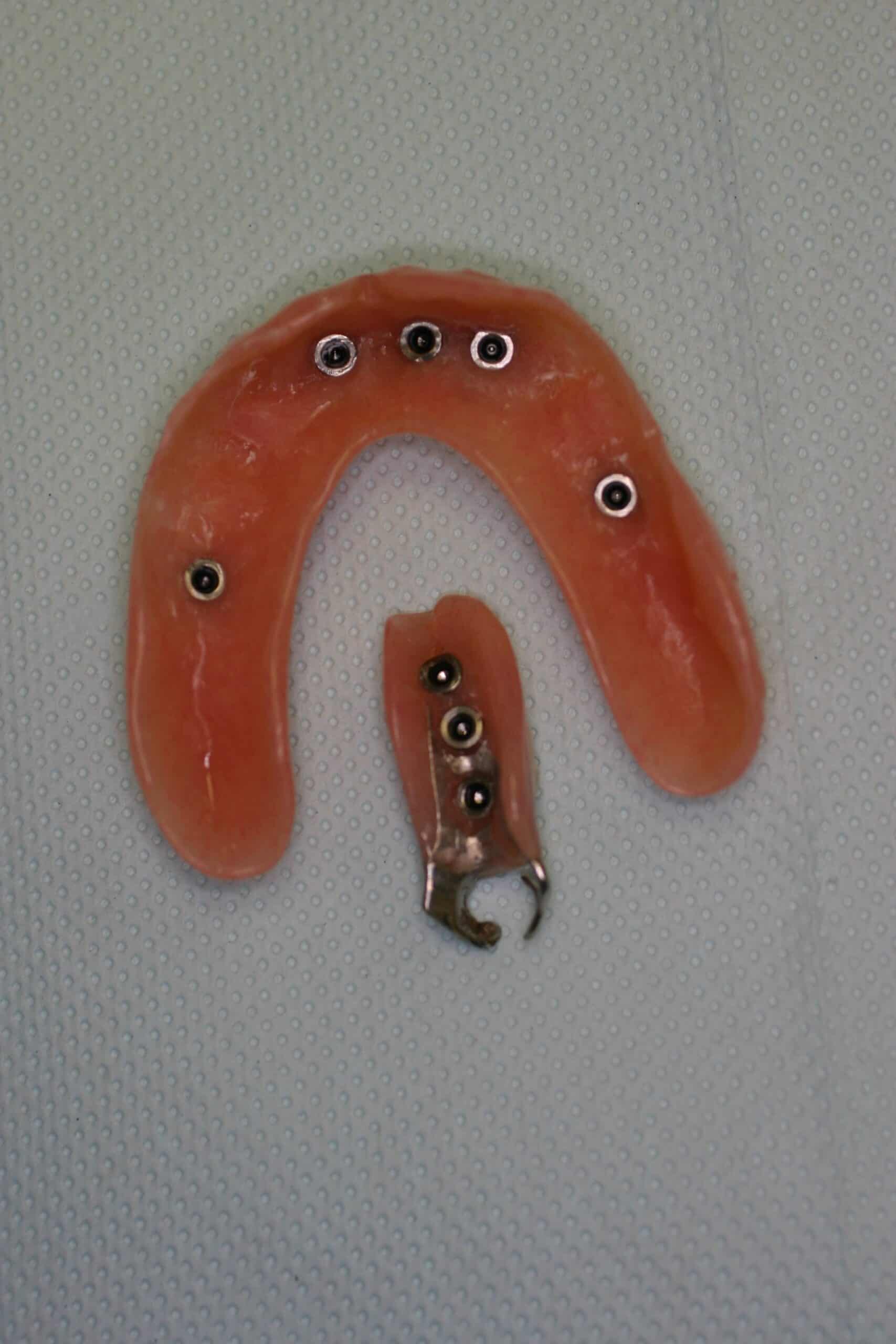
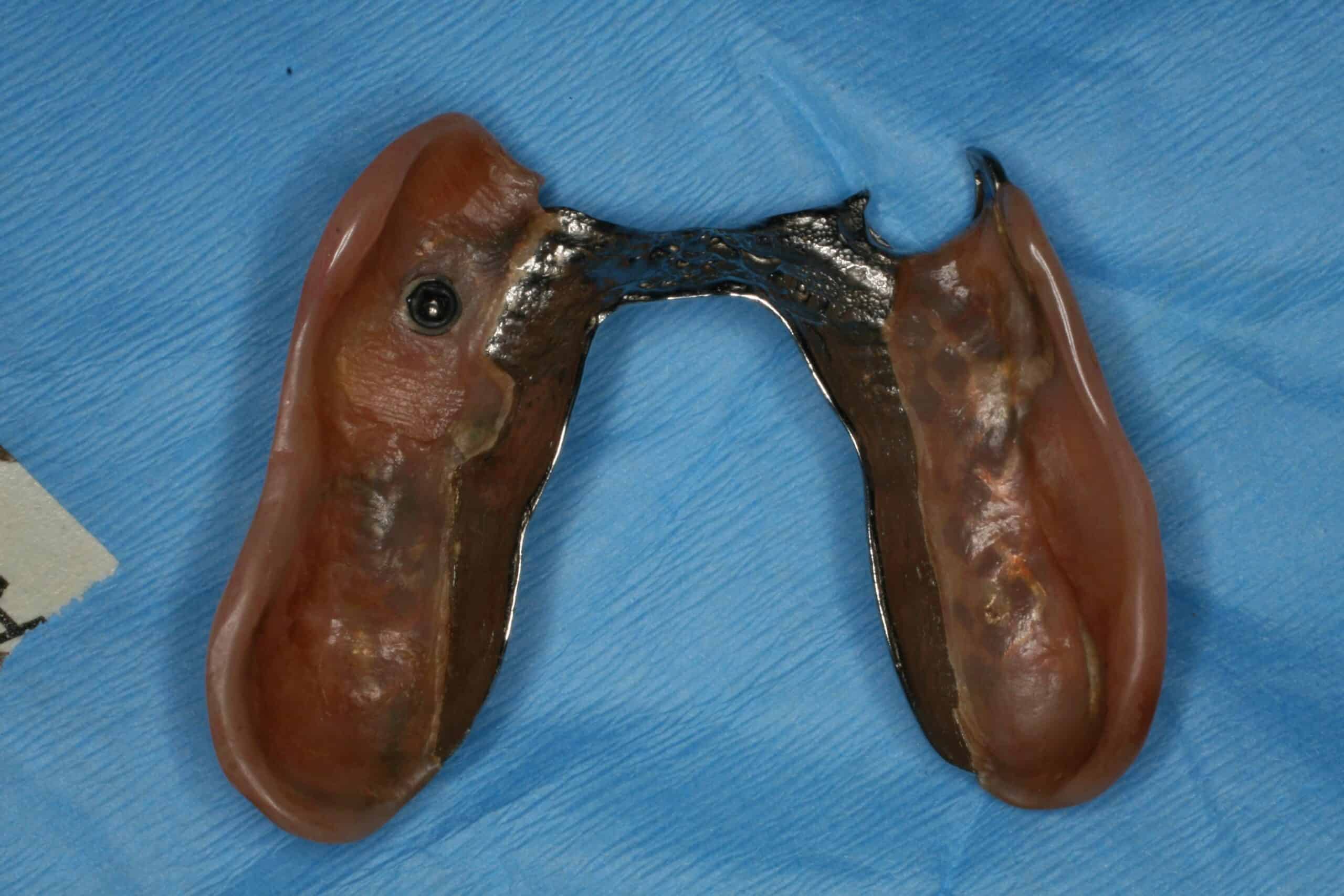
Not only was an immediate upper denture placed with MDI’s, but the lower partial denture was sectioned and made into a unilateral partial, all in one day. I don’t do anymore unilateral removable partial denture like these in this blog ( last one done about 4-5 years ago), and I understand they are actually illegal in some States because of a choking hazard. I can remember that they were not allow in the USAF either. Each one that I did was a modification of an existing partial that the patient could not tolerate crossing over to the other side of the mouth. They are actually hard to get out of the mouth with all the “O” ring retention.
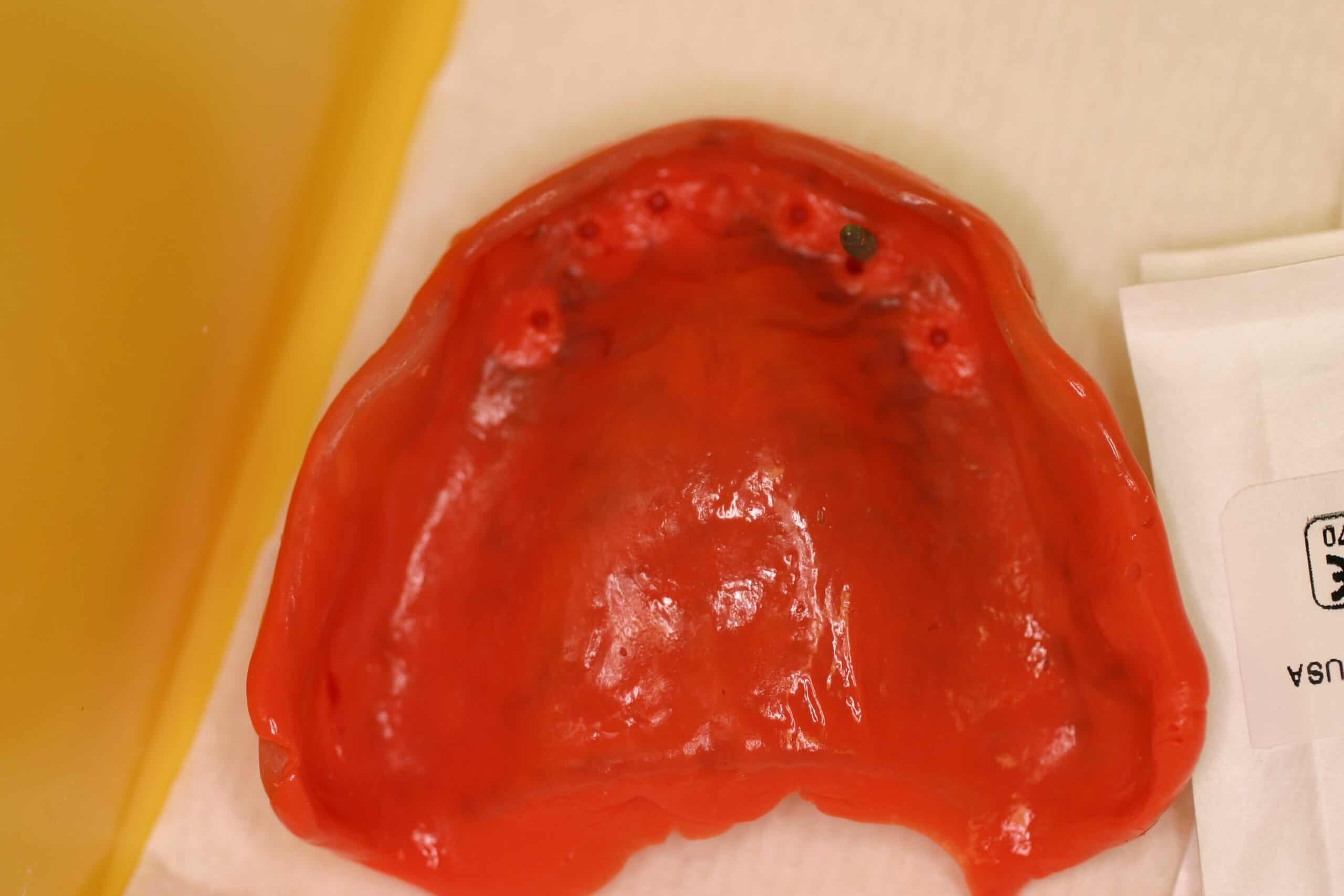
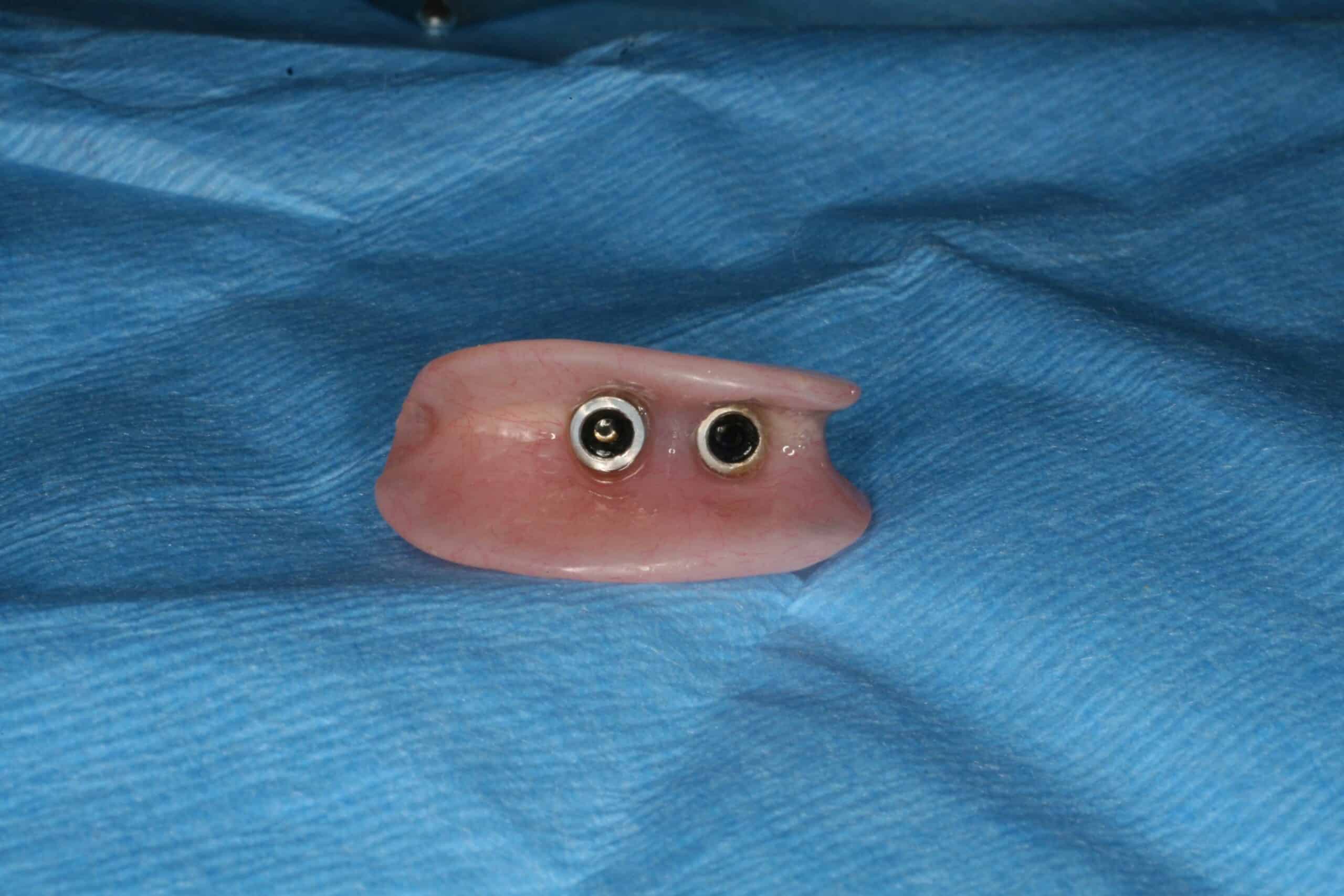
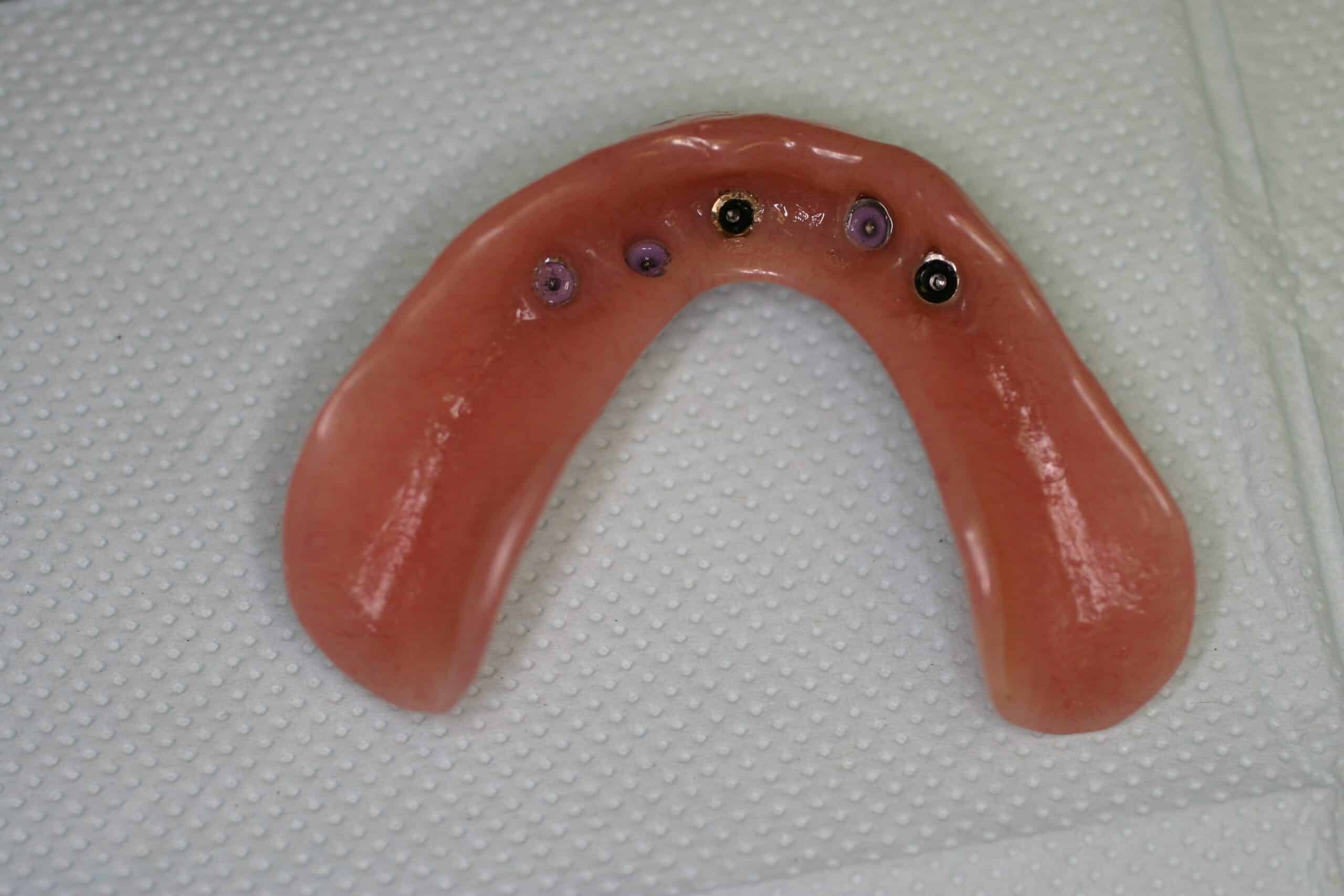
This is a simple straight forward case on the maxillary complete denture. Minimum of 5-6 MDI’s placed and relined with PVS impression material and this last photo has just one analog placed inside the impression for the placement of micro housing MDI snaps inside the denture.
This was a case where the patient recently lost a LR FPD and wanted something to replace it. We placed a lower transitional partial denture and he could not tolerate the acrylic behind his lower front teeth. Told him we could do a cast metal partial or regular cylinder implants but he didn’t want the RPD for the same reasons he didn’t like the /F and didn’t want to afford the implant/crowns to replace the old FPD. He did like the idea of the MDI supported unilateral transitional partial denture. I told him this would not be my first choice to restore his mouth, but he liked it.
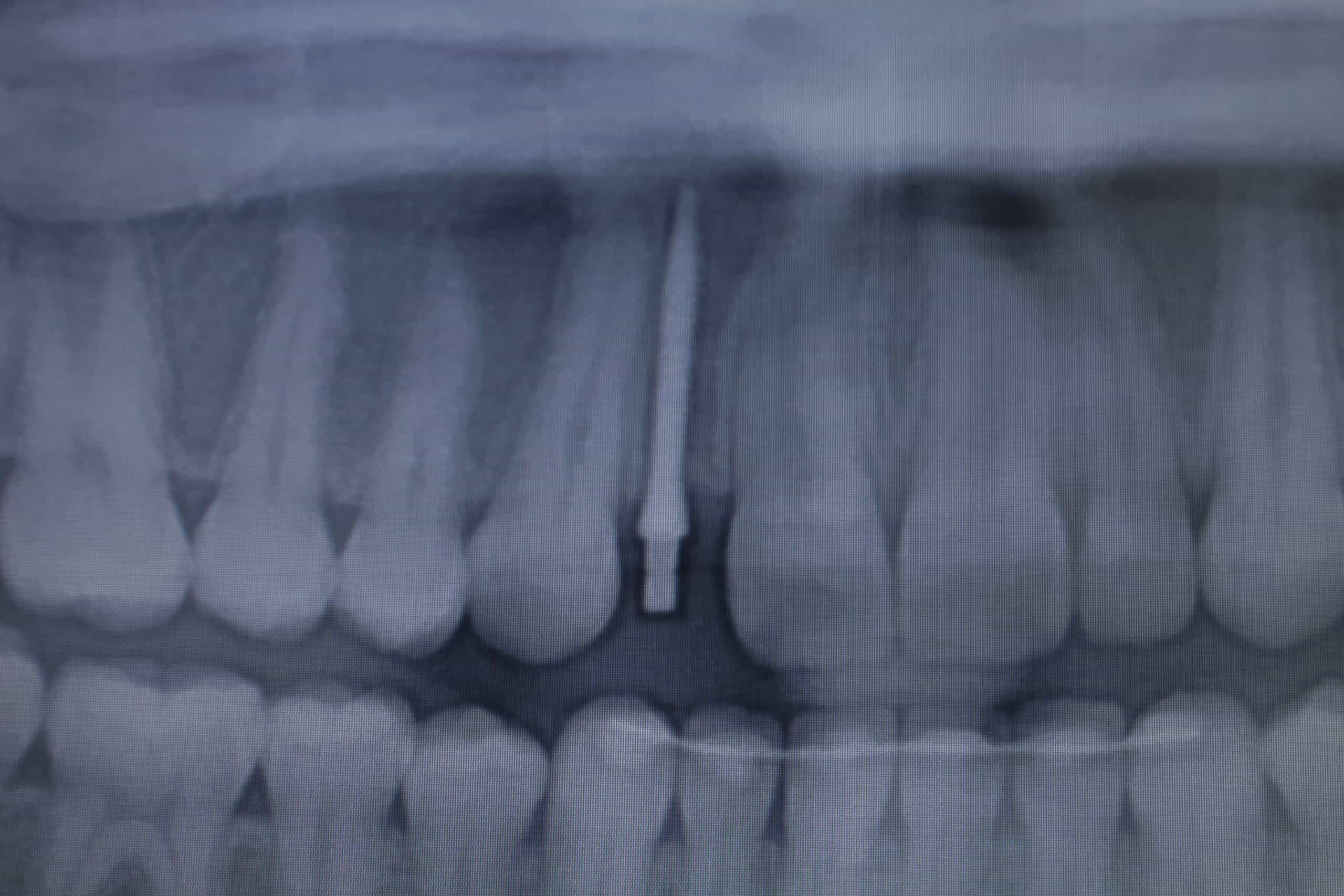
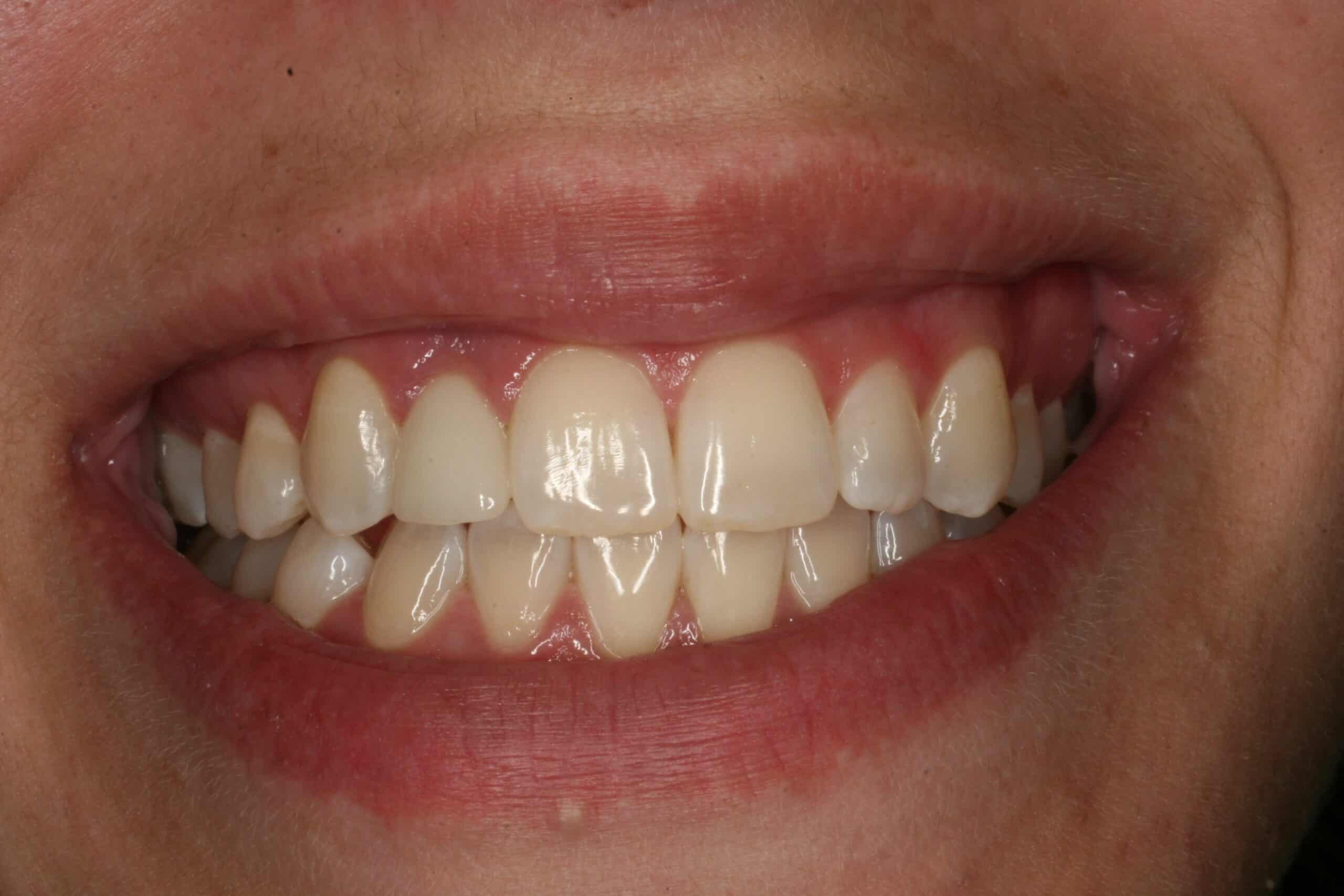
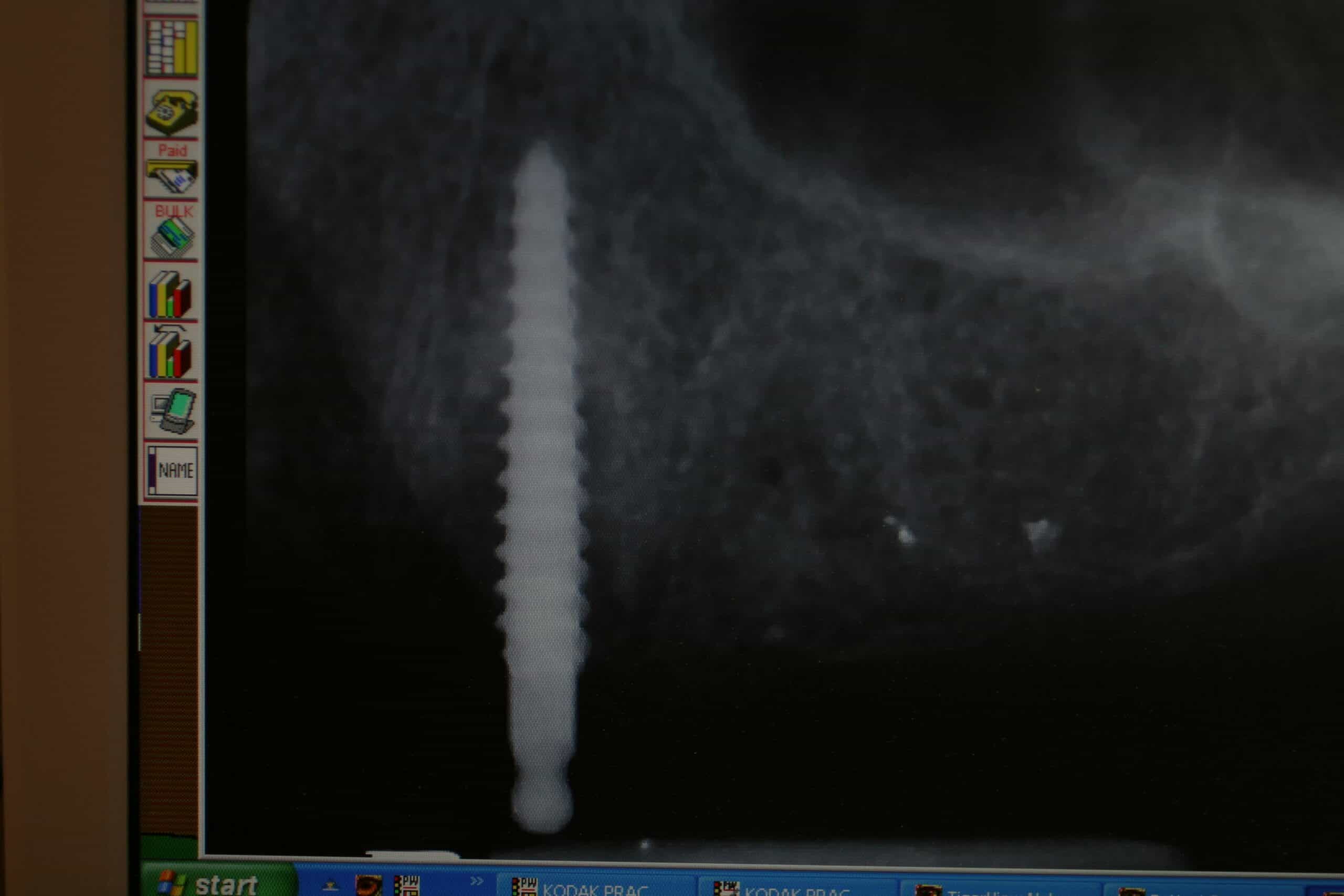
This is one of those case that the orthodontist opened a space for a congenitally missing lateral incisor, but neglected to torque the central incisor enough to a accommodate a regular implant. This was before Astra came out with their 3.0mm. A square headed MDI was placed and a PFM crown was manufactured. Note: It is very important for the patient to use their retainers properly or they will get a poor longer term result with any implant replacement.
This next case is a failure due to not enough support.
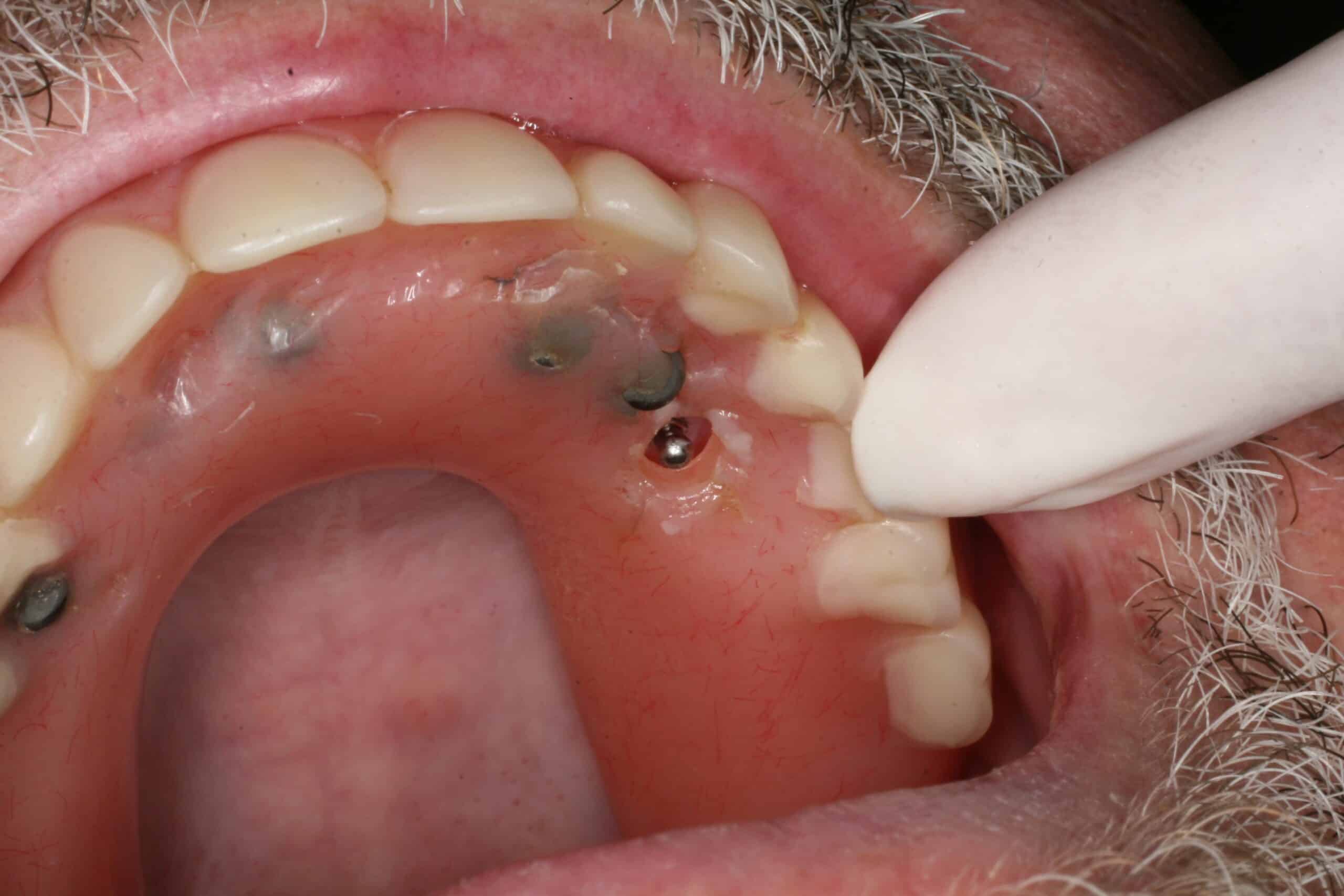
This MDI Max was placed to retain the upper partial after loosing a critical clasped tooth#11. However, the lone MDI was over powered by occlusal forces and failed needing to be replaced after 1 year. This is why I like to place larger cylinder implants in the maxilla whenever possible. The only problem is that once they have a MDI, the patients doesn’t want the larger more involved implant ( because of extended amount of time and extra cost). They usually want another MDI to replaced the lost one even though it may fail again.
Even though the MDI placement when well, you still have to have enough room in the old dentures VDO for the snaps to fit. In this case a new denture was needed to be made, but wasn’t totally realized until it was being delivered. Fortunately, we had mentioned that the denture would have to be remade eventually before we started the case. As a short term solution, more acrylic was placed to build up the VDO and the patient accepted the addition very well.
I recently had one of our very first mandibular MDI patients come back from living up North for 10 years. He is now a 93 y/o/w/m and he told me in a waving voice, “This was the best money I’ve ever spent in my entire life”. They still fit well with good bone. He just needed new “O” rings placed which were done in about 5 minutes by my assistant, and some calculus removed from around the MDI necks by one of our hygienists.
If the denture needs to have a reline, I usually replace all the snaps at the same time. Just reduce the denture flanges as usual, remove the “O” rings from the existing denture snaps and paint adhesive. Wash a PVS impression and instruct the lab to reline and replace the old snaps with new ones. Some doctors will tell the lab to just use the old snaps, and this is usually just fine to do. The “O” ring are easy to replace.
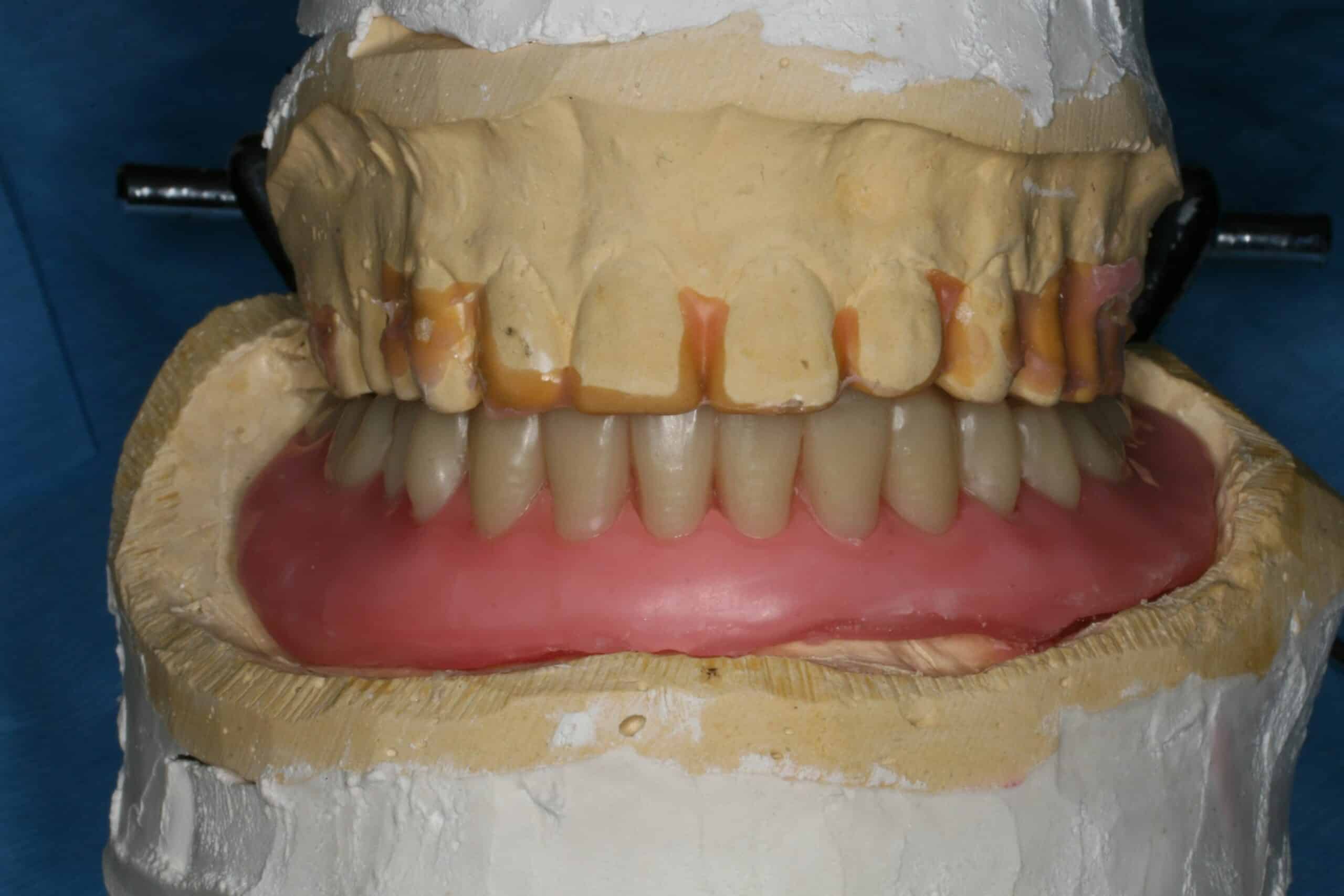
When it is time for the patient to have a new MDI overdenture a master cast is made with a custom tray and polyvinyl siloxane. A record base (master cast poured up with analogs in place) and occlusion rim is manufactured with holes cut out to accommodate the MDI heads. The denture teeth are set/waxed-up and tried in as usual. Once the aesthetics/occlusion are approved, another PVS wash is done inside the record base for maximum fit. The lab then processes and finishes the case ready for delivery. Bam!
There are new Zest  snaps that are said to accommodate a 30 degree angulation between the MDI’s and we will be investigation them in the near future as soon as we deplete our current supply of micro housing snaps that we have from Imtec and Intra-Lock.
snaps that are said to accommodate a 30 degree angulation between the MDI’s and we will be investigation them in the near future as soon as we deplete our current supply of micro housing snaps that we have from Imtec and Intra-Lock.
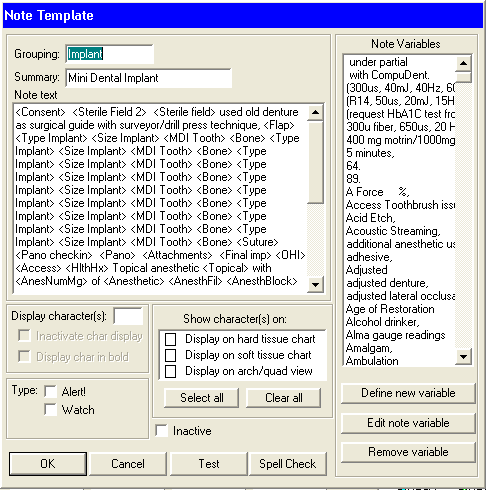
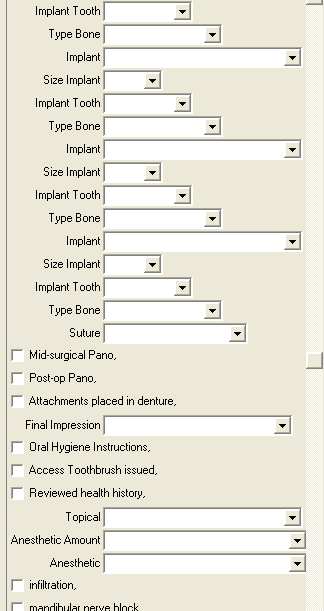
I made a Carestream/Kodak PracticeWorks note for placing MDI:
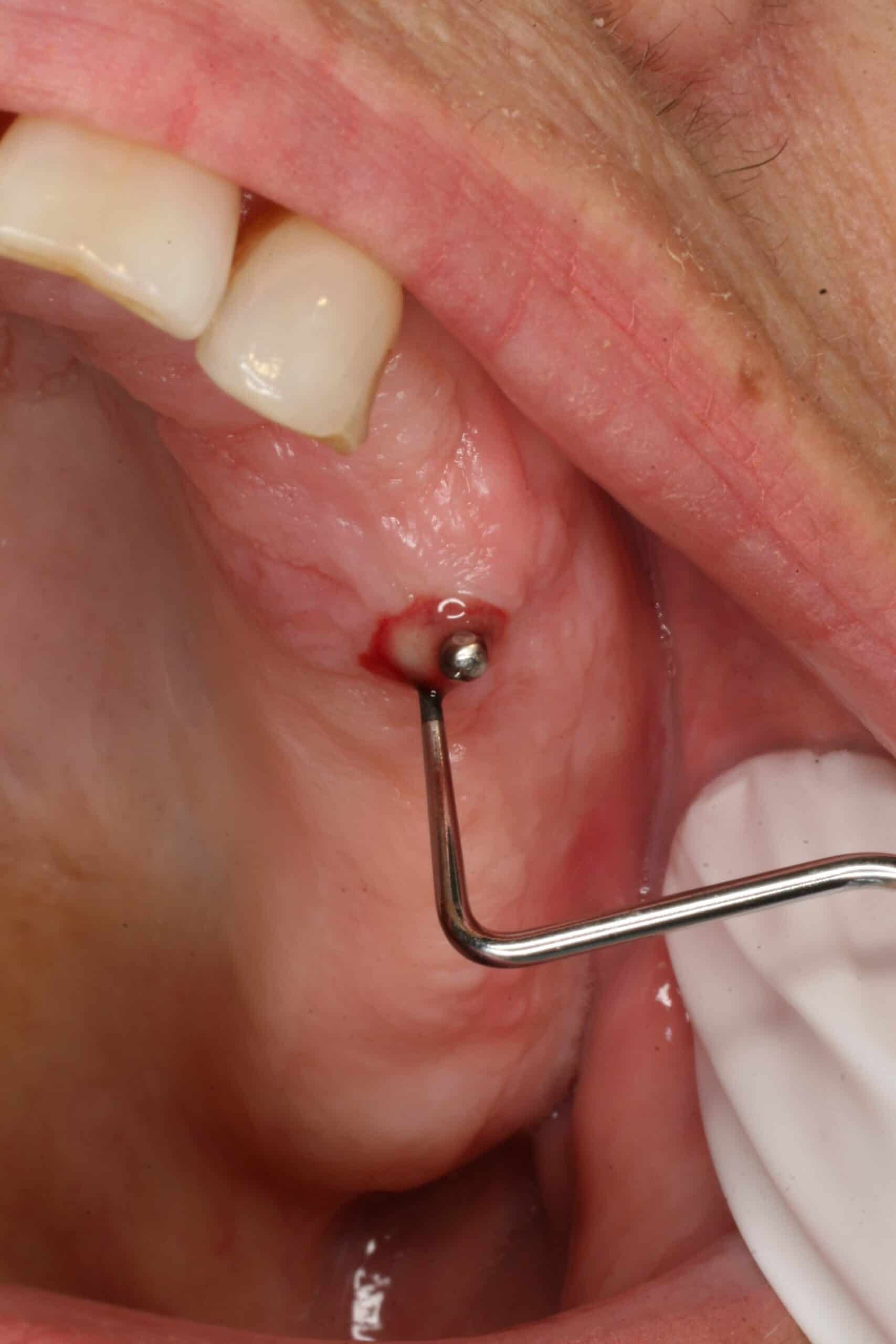
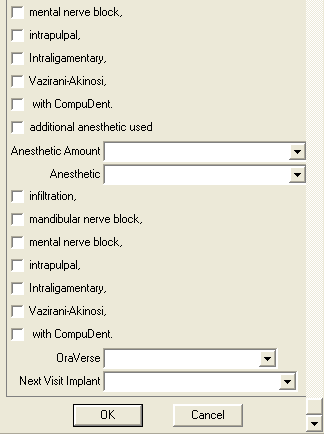
This is the note filled out for a typical 4 lower MDI to secure a lower denture to the mandible. I are experimenting with using a drill press to make a surgical guide so to line up the individual MDI when they are placed. Sometimes I open a small observation flap to visualize the bone, especially when there is a knife edge ridge. CBCT is very useful in determining where to place the MDI’s.
Informed Consent, Sterile Field Established, Skin/Mouth Prep-betadine & peridex, used old denture as surgical guide with surveyor/drill press technique, small observation flap elevated, Intra-Lock 2.0 15mm in #21 area, Type 3 bone, Intra-Lock 2.0 13mm in #23 area, Type 2 bone, Intra-Lock 2.0 13mm in #26 area, Type 2 bone, Intra-Lock 2.0 15mm in #28 area, Type 3 bone, Post-op Pano, Poylvinyl Siloxane Impression, Oral Hygiene Instructions, Reviewed health history, Topical anesthetic 20% lido/4% Tetra/2% phenylephrine with 1 carpule (68mg/1.7ml) of 4% Articaine w/1:100000 epi infiltration, Pt informed not to eat food, bite or chew on lips or tongue while anesthetic is still working. OraVerse 0.4mg. Next Visit: Del Dent w/ processed attachments in PM today.
The patient was informed that if we used their old denture that teeth may break off and/or the denture base could fracture due to inadequate thickness of material and/or old brittle denture(s).
5 days post-op note:
Healing within normal limits, OHI, issued access Toothbrush, adjusted denture, instructed the patient on how to place and remove the overdenture, issued a fixodent cleaning kit (without fixodent denture adhesive), Treatment was tolerated well. Next Visit: Post-op
We are currently using Astra![]() everywhere for implant restorations, and only place MDI in the lower anterior to secure complete dentures. The micro-threading around the neck of the Astra implants, and built-in platform switching make them osseous integrate very well. We just purchased the Vatech PaX-Duo3D CBCT, and are looking forward to getting it installed before the end of 2010 (since the U.S. Congress finally got their act together and stopped the tax increase).
everywhere for implant restorations, and only place MDI in the lower anterior to secure complete dentures. The micro-threading around the neck of the Astra implants, and built-in platform switching make them osseous integrate very well. We just purchased the Vatech PaX-Duo3D CBCT, and are looking forward to getting it installed before the end of 2010 (since the U.S. Congress finally got their act together and stopped the tax increase).