“Nothing personal doc, but I hate dentists.”
“When I was a child, I had a dentist that hurt me so bad I never got over it.”
“I’d rather have a baby than get dental work.”
“I have a really high pain tolerance for everything but dental work.”
“Can you just put me out, I really cannot stand that needle.”
“Doctor, do you have gas?”
Every dentist’s nightmare is that patient who has a fear of the local anesthetic needle. We inject patients all day long, over and over again, exactly the same way, in exactly the same spots. Most of the injections slip in without any pain at all, and you are a hero. Others sting like heck. Go figure.
The mandibular block slides in ¾ of an inch deep without any trouble, and the long buccal hurts like crazy just 2mm under the skin. Sometimes you can place a local injection under the nose, and nothing is felt. Other times it feels like you had punched them in the nose.
I always thought it was a factor of how fast you put the anesthetic into the tissue so we went out and bought a CompuDent (Wand) to help our pediatric patients. It actually works great. I call it God’s gift to the pediatric dentist. But the tubing costs a lot more than the carpule/needle of regular anesthetic, so we reserve it for only those real cry-babies.

Now there is a new way to make that needle slide in like butter without pain and it is called Onset from Onpharma. I first heard about this new product from Dr. Mark Colonna during my Lares Dental Research PowerLaser AT training. He had someone from the company at one of his classes as a student, and he put on a small presentation of this new product for everyone during a break. He told the class that Dr. Stanley Malamed said this was the greatest advancement in dental local anesthesia in 40 years. He also said that if I called and told them that I had heard about this product from Dr. Colonna, I’d be put on the priority list to receive the product. That was in October 2010 and I was promised a shipment around December 1. Then they contacted me saying it wouldn’t be until January 1. I finally received it on January 12th. I wanted to try this product so badly I didn’t even ask them how much it was going to cost. The starting package cost for me was $723.40. Individual costs are:
1 Onset Mixing Pens $299.00 each
1 Onset Cartridge connectors $49.80 (box of 4)
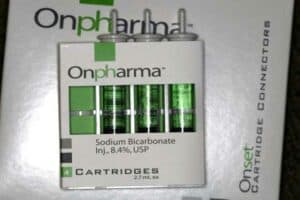
1 Bicarb 8.4% $210.10 (box of 4)
This is how the amps of bicarb come. Just push down and turn top knob and it slides out easily.
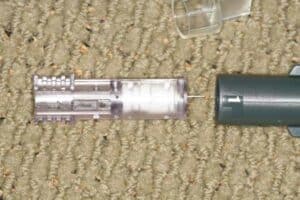
Unscrew the middle of the device to insert the amp of bicarb. The red piece screws the black plunger back to the rest position.
The black numbered dial is used to place the exact amount of bicarb into the carpule. I use to dial it to 18 which means 0.18ml of bicarb, but now I only use it dialed to 10 or 0.10ml (SEE BELOW).
This is the end that the carpule of anesthetic goes into. It has a a sponge in the middle of it to absorb the replaced anesthetic solution that is removed for the bicarb to enter. This is disposable after the amp of bicarb is empty.
It is not as expensive as the CompuDent, but it does increase your overhead a little.
At first the contraption looks pretty complicated. Lots of little parts to put together and step by step instructions to help you fumble through the process of loading your first carpule for your first test shot. But after you read the instructions, and go through the process once, it is a piece of cake. It is really pretty cool. You slide in the bulk bicarb in one end and the anesthetic carpule in the other, dial in the amount of bicarb to be mixed, push a button, and viola! Because the Henderson/Hasselbalch equation waits for no one, the carpule must be used immediately before the NaHCO3 + HCl -> H2O +CO2 allows all the CO2 to dissolve away. It was described to me as being about 30 seconds to a minute.
There are really two general actions that happen when you mix bicarb with local anesthetic:
- All amide local anesthetics are acidic. Lidocaine with epinephrine has a pH of 3.9. The normal physiological pH of the human body is 7.4. This difference in hydrogen ions are what researchers think causes the sting some patients feel when local anesthetics are injected into the body. Therefore, the slower you inject the anesthetic solution into tissue, the less pH shock the surrounding nerves sustain by neutralizing the acid with naturally occurring bicarbonates. Local anesthetics have to de-ionize for it to work. At a pH of 3.9, a typical cartridge of anesthetic contains only a small ratio of de-ionize to ionized molecules of anesthetic solution. Once the solution is buffered to a physiologic pH of 7.4 (SEE PART 2 of this blog for number to dial into to get a neutral pH), there are 2,500X more de-ionized molecules, and is much more effective.
- CO2, that comes out of the Henderson/Hasselbalch equation, possesses an independent anesthetic effect, and may provide the most immediate form of anesthesia. It can quickly diffuse into the surrounding tissues, and enter the nerves providing anesthesia within seconds after an injection. This is why it is very important to place the anesthetic as soon as possible after using the Onset mixing pen.
Practical Application
I’m just as skeptical about stuff like this as the next guy. Dentists have been stung so many times in the past from products that suddenly show-up on the news channels claiming to be the “must have” dental wonder drug/device/technique, then purchase the product, try it out, and find it is not so. I can remember the electronic anesthesia I used to use on my patients in the 1990’s. Now that I think about it, that product was one of the craziest products I had ever tried.
This is why I approached this new anesthetic buffering system with a little trepidation. The mixing pen was surprisingly simple to use. It is a really well thought out product. Place the carpule of anesthetic into the Onset Mixing Pen, and dial in the amount of bicarb you want to add. I dialed in the recommended amount of bicarb, 0.18ml (now I use 0.0 to 0.05ml), and pressed in into the carpule of anesthetic. I then popped it out of the mixing pen, into the syringe, and quickly placed bilateral mandibular blocks (½ carpule in each side). Quickly reloaded the mixing pen with another carpule, and quickly hydraulically elevated the lingual tissue of the lower mandible so I could remove tori. Then I sat back in my chair, and observed the patient for a second. He look totally undisturbed. I asked him on a scale of 1-10 with 10 being the worst how did he rate the injections I just gave him. I was honestly surprised at his reaction. He said, “What injections”. Everyone of my staff who were present for this inaugural event opened their eyes big and raised their eyebrows. As did I. Then he said, “You must have because my chin is totally numb”. This was about 1 minute after the injection. So I started working!
I proceeded throughout my day (Friday we work a half day) and numbed 7 patients with this technique. Each time I asked them to rate their experience from 1-10 and consistently got a pain ratings from 0-1 or 2. That was until this redheaded female patient came in. I gave an infiltration injection under the upper lip and she gave me a pain rating of a 6. I have to admit that by the time I saw her I was getting pretty cocky. Maybe I went to fast and this disturbed her? Maybe the bicarb didn’t have time to mix? Maybe it was because she was redheaded? Who is to know.
Of course, this formulary will not prevent the shock of hitting the mandibular or lingual nerve, nor prevent pain when forcing anesthetic solution into an abscess that is already hurting the patient. These discomforts are not due to the chemistry of the anesthetic solution.
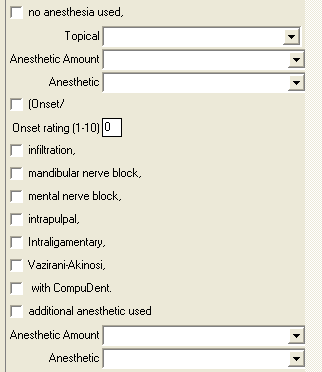
So this prompted me to write into my ordinary anesthetic note on Carestream/Kodak PracticeWorks a pain rating with the Onset technique.
After the end of the day I noted that the 3.0ml vial of bicarb was about ½ way full which made sense since the manufacture said each vial was enough to mix into 16 carpules of anesthetic. At the regular price that comes out to about $5 per injection, which is inside my comfort zone. Oraverse should take a lesson from these guys! If you only dial it to 5 (0.05ml) it will cost around $1 per injection.
I will continue to use this product on every patients for two very good reasons:
- My patients like it, and I like it, too!
- I spend a lot of money every year advertising my practice in the Yellow Pages, NewsPress, and TV ads, but one method consistently stands out more than all the others combined, word of mouth.
Onpharma’s Onset Mixing Pen is definitely a product you need to get for your dental practice. You can also get set-up with a standard monthly order to make sure you do not ever run out of this product. Phone number: 1.877.336.6738
I have now gone through several months of injections, and have had an average pain rating (0-10) of 1 (with the majority being 0).
Places that still have trouble with Onset local anesthetic are:
- Injecting right into a painful abscess (expansion of an already painful situation)
- Hitting the lingual nerve (direct mechanical stimulation)
- The very tight tissue on the palate (pressure pain of expanding/tearing the tissue)
- The very excitable patient who may need IV sedation
- The actual anesthetic carpules are not the same size all the time. This makes it difficult at times to insert the carpule into the mixing pen.
Troubleshooting:
- Stuck injector button: After using the Onset Mixing Pen for several weeks it may begin to have bicarbonate/anesthetic crystals build up inside the pen. This will cause the pen to freeze and not inject properly. The easiest remedy I have found is to remove the injector dial part of the mixing pen, use a suitable water filled container, hold the pen underwater, and open it up all the way to 60. Let it soak then push the button in and out a few time (under water) and within a few seconds it will work just fine.
- The center piece can split in half with heavy usage. I do the simplest repair possible by wrapping identification tape around the pens that have not split and a zip tie around the ones that have split.
- The carpule of anesthetic is hard to push into the mixing pen: Occasionally, one of the carpule insert ends will be very tight and the carpule is hard to push all the way in. The only thing I do is get a better grip and push really hard. Once the first one goes in all the way the second one is usually easier. This is because the manufactures of the actual dental anesthetic carpules are not consistent in their diameters (from Onpharma).
- The bicarbonate doesn’t inject into the carpule. This is actually very hard to detect. Unfortunately, you usually find this out by having the patient feel your injection more than usual. The only answer I have found to this problem is replacing the cartridge connector due to the needles inside being plugged or bent. Look at the end of the carpule to see if the connector needles are centered enough to penetrate the rubber of the anesthetic carpule and not trying to penetrate the metal ring.
- Keep a spare mixing pen so you can immediately use it if you ever experience technical difficulty or run out of bicarb.
- I will have to say that this design flaw has been addressed by the manufacture and a new stronger weld has been used. Also a soon to be implemented “ferrule” band will be placed over any potential weak points in the plastic welds (from Onpharma).
Areas for Further Research:
- What is the minimal bicarb dose needed? For the first 8 months I used a “dialed-in” number of 18 which I correspond to 0.18ml. However, I had recently dialed it back to 10 (.10ml) during a time when our shipment was delayed and have had the very same if not better results. This brought our price down to approximately $2 per injection. Next, I am going to dialing it to 5 (0.05ml) to see what happens (so far looking good, but I will be testing the pH to find out what is actually going on before I recommend this dose; SEE BELOW pH TEST).
- Tissue toxicity? Especially with Articaine 4% with 1:100,000 epi. The percentages of the different local anesthetics have been research extensively to give us safe doses. Are we not changing the chemistry and actions of these drugs by “boosting” them into a different performance level inside the tissue?
- Please report any adverse side effects seen with this product in the comment section of this blog so these problems (such as tissue necrosis and cellulitis), if any, can be addressed.
Go to Part 2 of this blog
References
1 Momsen OH, Roman CM, Mohammed BA, Andersen G, Neutralization of Lidocaine-Adrenaline, A Simple Method for Less Painful Application of Local Anesthesia, Ugeskr Laeger, Vol. 162, No. 33, P. 4391 (2000).
2 Bowles WH, Frysh H, Emmons R, Clinical Evaluation of Buffered Local Anesthetic, General Dentistry, Vol. 43, No. 2, P. 182 (1995).
3 Lugo-Janer G, Padial M, Sanchez JL, Less Painful Alternatives for Local Anesthesia, J Dermatol Surg Oncol, vol. 19, pp. 237-40 (1993).
4 Christoph RA, Buchannan L, Begalla K, Schwartz S, Pain Reduction in Local Anesthetic Administration Through pH Buffering, Annals of Emergency Medicine, Vol. 17, No. 2, P 117 (1988).
5 Vossinakis IC, Stavroulaki P, Paleochorlidis I, Badras LS, Reducing the Pain Associated with Local Anesthetic Infiltration for Open Carpal Tunnel Decompression, British Journal of Hand Surgery, Vol. 4, No. 29B, P. 399 (2004).
6 Samdahl F, Arctander K, Skollborg K, Amland PF, Alakalization of Lignocane-Adrenaline Reduces the Amount of Pain During Subcutaneous Injection of Local Anesthetic, Scandanavian Journal of Plastic and Reconstructive Hand Surgery, Vol. 28, P. 33 (1994).
7 Martin AJ, pH-Adjustment and Discomfort Caused by the Intradermal Injection of Lignocaine, Anesthesia, P. 975, Vol. 45 (1990) (pH 3,76).
8 Masters JE, Randomized Control Trial of pH-buffered Lignocaine with Adrenaline in Outpatient Operations, British Journal of Plastic Surgery, P. 385, Vol. 51 (1998) (pH 3.51).
9 McKay W, Morris R, Mushlin P, Sodium Bicarbonate Attenuates Pain on Skin Infiltration, Anesth Analg, vol. 66, pp. 572-74 (1987).
10 Younis I, Bhutiani RP, Taking the ’Ouch’ Out – Effect of Buffering Commercial Xylocaine on Infiltration and Procedure Pain – a Prospective, Randomised, Double-Blind, Controlled Trial, Annals of the Royal College of Surgeons of England, Vol 86, P. 213 (2004).
11 Fitton AR, Ragbir M, Milling AP, The Use of pH Adjusted Lignocaine in Controlling Operative Pain in the Day Surgery Unit: A Prospective, Randomized Trial, British Journal of Plastic Surgery, Vol. 49, P. 404 (1996).
12 Metzinger SE, Rigby PL, Bailey DJ, Brousse RG, Local Anesthetic in Blepharoplasty, A New Look?, Southern Medical Journal, Vol. 87, No. 2, P. 225 (1994).
13 Carvalho B, Fuller A, Brummel C, Cohen SE, Local Infiltration of Epinephrine-Containing Lidocaine with Bicarbonate Reduces Superficial Bleeding and Pain During Labor Epidural Catheter Insertion: A Randomized Trial, Intern J Obstetric Anesth, Vol 16, P. 116 (2007).
14 Yuen VH, Dolman PJ, Comparison of Three Modified Lidocaine Solutions for Use in Eyelid Anesthesia, Ophthalmic Plastic and Reconstructive Surgery, Vol. 15, No. 2, P 143 (1999).
15 Talu H, Elibol O, Yanyali A, Karabas L, Alp B, Caglar Y, Effect of Warming and Buffering Lidocaine on Pain During Facial Anesthesia, Annals of Ophthalmology, vol. 33, no. 1, pp. 43-47 (2001).
16 Burns CA, Ferris G, Feng C, Cooer JZ, Brown MD, Decreasing the Pain of Local Anesthesia: A Prospective, Double-Blind Comparison of Buffered Premixed 1% Lidocaine with Epinephrine Versus 1% Lidocaine Freshly Mixed with Epinephrine, Journal of the Am. Academy of Derm., Vol. 54, No. 1, P. 128 (2006).
17 Stewart JH, Cole GW, Klein JA, Neutralized Lidocaine with Epinephrine for Local Anesthesia, J Dermatol Surg Oncol, vol. 15, no. 10, p. 1081 (1989).
18 Primosch RE, Robinson L, Pain Elicited During Intraoral Infiltration with Buffered Lidocaine, American Journal of Dentistry, Vol. 9, No. 1, P. 5 (1996).
19 Whitcomb M, Drum M, Reader A, Nusstein M, Beck M, A Prospective, Randomized, Double-Blind Study of the Anesthetic Efficacy of Sodium Bicarbonate Buffered 2% Lidocaine with 1 : 100,000 Epinephrine in Inferior Alveolar Nerve Blocks, Anesthesia Progress, Vol. 57, P. 59 (2010).
20 Nuttal GA, Barnett MR, Smith RL, Blue TK, Clark KR, Payton BW, Establishing Intravenous Success, a Study of Local Anesthetic Efficacy, Anesth Analg, vol. 77, pp. 950-53 (1993).
21 Erramouspe, Buffering Local Anesthetic Solutions with Sodium Bicarbonate: Literature Review and Commentary, Hosp Pharm, vol. 31, no. 10 (1996).
22 Ruegg TA, Curran CR, Lamb TL, Use of Buffered Lidocaine in Bone Marrow Biopsies: A Randomized, Controlled Trial, Oncology Nursing Forum, Vol. 39, No. 1, P. 52 (2009).
23 Masters, et al, Randomized Control Trial of pH-buffered Lignocaine with Adrenaline in Outpatient Operations, supra.
24 Hinshaw KD, Fiscella R, Sugar J, Preparation of pH Adjusted Local Anesthetics, Ophthalmic Surgery, P. 194, Vol. 26, No. 3, (1996)(pH 3.74).
25 Martin AJ, pH-Adjustment and Discomfort Caused by the Intradermal Injection of Lignocaine, Anesthesia, P. 975, Vol. 45 (1990) (pH 3,76).
26 Ikuta Pt, Raza SM, Duranni Z, Vasireddy AR; Winnie AP, Masters RW, pH Adjustment Schedule for the Amide Local Anesthetics, Regional Anesthesia, P. 229, Vol. 14, No. 5 (1989) (pH 3.9).
27 Joseph RS, McDonald SB, Facilitating the Onset of Regional Blocks, Techniques in Regional Anesth and Pain Mgmt, P. 110, Vol. 8, No. 3 (2004) (pH 4.1).
28 Crews JC, Clark RB, Effect of Alkalinization on the pH of Local Anesthetic Solutions, Anesthesia and Analgesia, P. 1196, Vol. 66 (1987) (pH 4.16).
29 Kennedy RM, Luhman JD, The ‘Outchless Emergency Department’, Getting Closer: Advances in Decreasing Distress During Painful Procedures in the Emergency Department, Pediatric Clinics of North America, Vol. 46, No. 6, P. 1220 (1999).
30 Bartfield, Buffered Lidocaine as a Local Anesthetic: An Investigation of Shelf Life, Annals of Emergency Medicine, , Vol. 21, No. 1, P. 24 (1992).
31 Gupta RP, Kapoor G, Safety and Efficacy of Sodium Bicarbonate Versus Hyaluronidase in Peribulbar Anesthesia, Medical Journal Armed Forces India, Vol. 62, P. 116 (2006).
32 Burmeister CH, A Practical Method for the Extemporaneous Preparation of a Buffered Anesthetic Solution, Journal of the American Dental Association, Vol. 22, P. 1514 (1935), citing Laewen A, München Med. Wchnschr., P. 2044 (1910).
33 Hille B, The pH Dependent Rate of Action of Local Anesthetics on the Node of Ranvier, The Journal of General Physiology, Vol. 69, P. 475 (1977).
34 Mehta R, Verma DD, Gupta V, Gurwara AK, The Effect of Alakalinization of Lignocaine Hydrochloride on Brachial Plexus Block, Indian Journal of Anesthesia, Vol. 47, No. 4, (2003). See also, Difazio CA, Carron H, Grosslight KR, Moscicki JC, Bolding WR, Johns RA, Comparison of pH-Adjusted Lidocaine Solutions for Epidural Anesthesia, Anesthesia and Analgesia, Vol. 65, P. 760 (1986); Fitton et al, supra.
35 Bonhomme L, Postaire E, Touratier S, Benhamou D, Martre-Savageon H, Preaux N, Chemical Stability of Lignocaine (Lidocaine) and Adrenaline (Epinephrine) in pH Adjusted Parenteral Solutions, Journal of Clinical Pharmacy and Therapeutics, Vol. 13, P. 257 (1988).
36 Gardner JH, Semb J, The Relation of pH and Surface Tension to the Activity of Local Anesthetics, Journal of Pharmacology and Experimental Therapeutics, Vol. 54, P. 309 (1935).
37 Tuckley JM, The Pharmacology of Local Anesthetics, Update in Anesthesia, Vol. 4, No. 7 (1994).
38 Mehta et al, The Effect of Alakalinization of Lignocaine Hydrochloride on Brachial Plexus Block, supra; see also, Difazio et al, Comparison of pH-Adjusted Lidocaine Solutions for Epidural Anesthesia, supra; and Fitton et al, The Use of pH Adjusted Lignocaine in Controlling Operative Pain in the Day Surgery Unit: A Prospective, Randomized Trial, supra.
39 Talu, et al, Effect of warming and buffering lidocaine on pain during facial anesthesia, supra.
40 Richtsmeier, et al, Buffered Lidocaine for Skin Infiltration Prior to Hemodialysis, J Pain and Sympt Man, vol 10(3), p.198 (1998).
41 Burns et al, Decreasing the Pain of Local Anesthesia: A Prospective, Double-Blind Comparison of Buffered Premixed 1% Lidocaine with Epinephrine Versus 1% Lidocaine Freshly Mixed with Epinephrine, supra.
42 Ackerman WE, Ware TR, Juneja M, The Air-Liquid Interface and the pH and PCO2 of Alkalinized Local Anaesthetic Solutions, Canadian Journal of Anaesthesiology, Vol. 39, No. 4, P. 387 (1992).
43 Catchlove RFH, The Influence of C02 and pH on Local Anesthetic Action, The Journal of Pharmacology and Experimental Therapeutics, Vol. 181, No. 2, P. 208 (1972).
44 Condouris GA, Shakalis A, Potentialtion of the Nerve-Depressant Effect of Local Anesthetics by Carbon Dioxide, Nature, Vol. 204, No. 4953, P. 57 (1964).
45 Otsuguro K, Yasutake S, Yoshihiko Y, Ban M, Ohta T, Ito S, Why Does Carbon Dioxide Produce Analgesia? AATEX, Vol. 14, P. 101 (2007).
46 Catchlove, The Influence of C02 and pH on Local Anesthetic Action.
47 Talu, et al, Effect of Warming and Buffering Lidocaine on Pain During Facial Anesthesia, supra.
48 Richtsmeier, et al, Buffered Lidocaine for Skin Infiltration Prior to Hemodialysis, supra.
49 Burns et al, Decreasing the Pain of Local Anesthesia: A Prospective, Double-Blind Comparison of Buffered Premixed 1% Lidocaine with Epinephrine Versus 1% Lidocaine Freshly Mixed with Epinephrine, supra.
50 Ikuta PT, Raza SM, Durrani Z, Vasireddy AR, Winnie AP, Masters R, pH Adjustment Schedule for the Amide Local Anesthetics, Regional Anesthesia, Vol. 14, No. 5, P. 232 (1989).
51 Christoph RA, Buchanan L, Begalla K, Schwartz S, Pain Reduction in Local Anesthetic Administration Through pH Buffering, Emergency Medicine, Vol. 17, No. 2, P. 27 (1988). For other articles recommending immediate of local anesthetic use after buffering, see: Erramouspe J, Buffering Local Anesthetic Solutions with Sodium Bicarbonate, Literature Review and Commentary, Hospital Pharmacy, Vol. 31, No. 10, P. 1275 (1996); Armel HE, Horowitz M, Alkalinization of Local Anesthesia with Sodium Bicarbonate – Preferred
Method of Local Anesthesia, Urology, Vol. 43, No.1, P. 101 (1994).