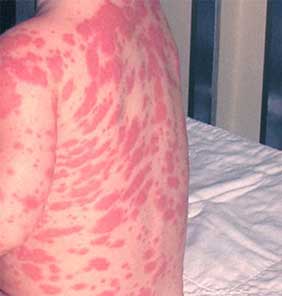
Practically every week we have a new patient come into our office who should be pre-medicating for dental treatment who are not, nor do they have any idea that they should. Just today a lady called our office for a cleaning and exam. Our front desk asked if she had any recent surgeries or heart problems for which she answered, “Oh yes honey. I had my knee replaced about 9 months ago.” When asked if she had a prescription for her premedication, she answered back, “What are you talking about?”
Premedication:
Artificial Joints:
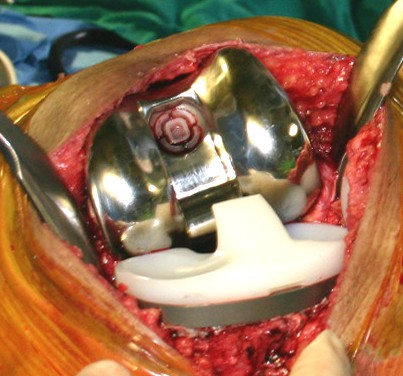 Humans are living longer lives today than ever before. Not only are some people living longer than their teeth, but they are living longer than some of the major joints inside their bodies. It is not uncommon to hear of someone who has had a joint or two actually replaced. Knees and hips seem to be the most popular joints to replace.
Humans are living longer lives today than ever before. Not only are some people living longer than their teeth, but they are living longer than some of the major joints inside their bodies. It is not uncommon to hear of someone who has had a joint or two actually replaced. Knees and hips seem to be the most popular joints to replace.
Having one of your joints replaced is no picnic. The orthopedic surgeon basically saws off the natural joint, and replaces it with a titanium substitute. The natural joint was composed of living cells. Those cells require oxygen and that oxygen is supplied by blood vessels. The new titanium joints are artificial and do not require blood vessels to nourish it. And here lies the problem. The artificial joint has a lot of free space inside of it that fills up with interstitial fluid which is the fluid found between cells or roughly equivalent to blood plasma. If a bacteria finds its way into this space, then it is a very, very long distance for a white blood cell to travel without oxygen to fight, eat and then remove the bacteria. After about two years post-op there is usually enough scarring around the artificial joint to make an adequate barrier to protect the joint from bacterial invasion. This is why the American Association of Orthopaedic Surgeons have the guide lines of only premedicating an artificial joint for two years post-op (unless immune compromised). After that point, the antibiotics are more of a risk to the patient’s health (allergic reaction) than the chance for joint infection.
Heart:
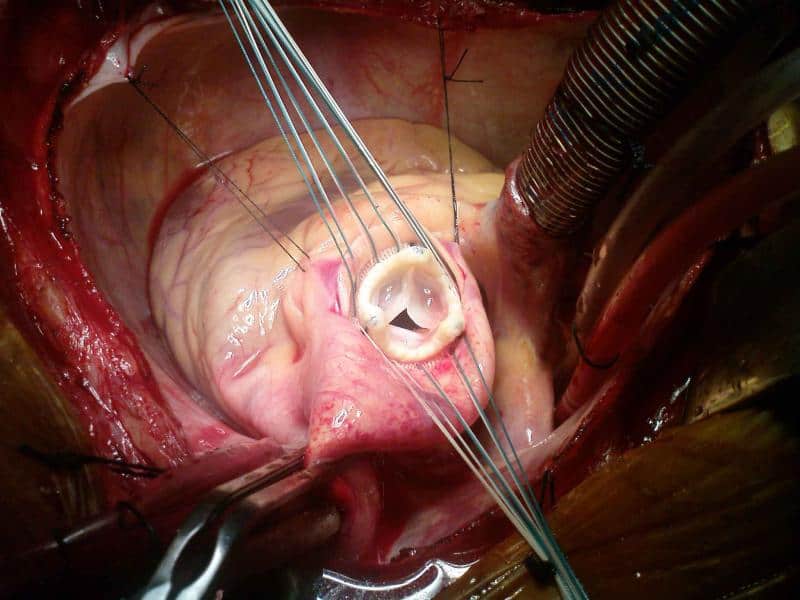 We have been premedicating the heart for various ailments for decades. In the past, anyone with a heart murmur received antibiotics one hour before their dental appointment. Then the American Heart Association (AHA) said mitral valve prolapse needed to be premedicated. Then it was mitral valve prolapse with regurgitation. Now the newest guidelines: (AHA, 2007)
We have been premedicating the heart for various ailments for decades. In the past, anyone with a heart murmur received antibiotics one hour before their dental appointment. Then the American Heart Association (AHA) said mitral valve prolapse needed to be premedicated. Then it was mitral valve prolapse with regurgitation. Now the newest guidelines: (AHA, 2007)
- Artificial heart valve (and valves repaired with artificial material).
- History of bacterial endocarditis.
- Heart transplant (with abnormal heart valve function)
- Congenital heart defects:
- Congenital heart birth defects with low oxygen levels (not totally repaired), including surgical shunts and conduits.
- Six months after a congenital heart defect repaired with artificial material.
- Defective repairs of a congenital heart disease.
Amoxicillin:
Adults: 2 grams (500 mg X 4) one hour before dental appointment
Children: 50 mg/kg one hour before dental appointment
Patients allergic to penicillin: Clindamycin, Cephalexin, Cefadroxil, Azithromycin or Clarithromycin is given one hour before the procedure. (noting that Cephalexin and Cefadroxil are closely related to penicillin and should not be used in patients with an immediate/severe allergic reaction to penicillins.)
Clindamycin:
Adults: 600 mg (150 mg X 4)one hour before dental appointment
Children: 20 mg/kg one hour before dental appointment
Cephalexin/Cefadroxil
Adults: 2 grams (500 mg X 4) one hour before dental appointment
Children: 50 mg/kg one hour before dental appointment
Azithromycin/Clarithromycin:
Adults: 500 mg one hour before dental appointment
Children:15 mg/kg one hour before dental appointment
Anaphylactic Shock:
Anaphylactic shock is systemic vasodilation with low blood pressure, and severe bronchoconstriction to the point of being unable to breathe (as a result of an allergic reaction). If after taking a medication you either begin to get hives/rash, your throat begins to swell and/or you have difficulty breathing, then go to the EMERGENCY ROOM IMMEDIATELY. Failure to do so may end in DEATH.
References:
1. Srp Arh Celok Lek. 2010 Nov-Dec;138(11-12):714-20. [Are new recommendations on the prevention of infective endocarditis applicable in our environment?]. [Article in Serbian] Ivanovi? B, Mati? S, Pavlovi? M, Tadi? M, Simi? D.
2. Methodist Debakey Cardiovasc J. 2010 Nov-2011 Jan;6(4):48-52. Antibiotic prophylaxis for infective endocarditis: ethical care in the era of revised guidelines. Bach DS. University of Michigan, Ann Arbor, Michigan, USA.
3. Heart Lung Circ. 2010 Sep;19(9):566-71. Epub 2010 Jun 11. A case of intra-cardiac right-sided mural infective endocarditis associated with ventricular septal defect despite prophylactic antibiotics: a case report. Lin T, Santos M, Aboltins C, Chiu H, Van Gaal W, Wong C. Department of Cardiology, Northern Health, 185 Cooper Street, Epping, Victoria 3076, Australia. tina9989@gmail.com
4. Infect Disord Drug Targets. 2010 Feb;10(1):59-64. Current indications for infective endocarditis antibiotic prophylaxis. Valle-Caballero MJ, Muñoz-Calero B, Araji OA. Department of Cardiology, University Hospital Virgen Macarena, Seville, Spain. dra.mjvc@gmail.com
5. Heart Lung. 2010 Jan-Feb;39(1):64-72. Epub 2009 Jul 10. Viridans streptococcal (Streptococcus intermedius) mitral valve subacute bacterial endocarditis (SBE) in a patient with mitral valve prolapse after a dental procedure: the importance of antibiotic prophylaxis. Cunha BA, D’Elia AA, Pawar N, Schoch P. Infectious Disease Division, Winthrop-University Hospital, Mineola, New York 11501, USA.
6. J Evid Based Dent Pract. 2009 Dec;9(4):183-93. Implementation of clinical practice guidelines in dental settings. Soheilipour S, Dunne SM, Newton JT, Jabbarifar SE. Department of Oral Health Services Research & Dental Public Health, King’s College London, London, United Kingdom. shimae.soheilipour@kcl.ac.uk
7. Cardiovasc Hematol Disord Drug Targets. 2009 Dec;9(4):231-5. Odontogenic infections in the etiology of infective endocarditis. Bascones-Martínez A, Muñoz-Corcuera M, Meurman JH. Facultad de Odontología, Universidad Complutense de Madrid, Spain. antbasco@odon.ucm.es
8. Spec Care Dentist. 2009 Jul-Aug;29(4):175-8. Knowledge and practices of dentists in preventing infective endocarditis in children. Coutinho AC, Castro GF, Maia LC. Post-graduate Student, Department of Pediatric Dentistry and Orthodontics, School of Dentistry Federal University of Rio de Janeiro, Brazil.
9. Int J Oral Maxillofac Surg. 2009 Jun;38(6):626-31. Epub 2009 May 20. Infective endocarditis and antibiotic prophylaxis prior to dental/oral procedures: latest revision to the guidelines by the American Heart Association published April 2007. Farbod F, Kanaan H, Farbod J. St. John Health, Department of Oral and Maxillofacial Surgery, Warren, MI 48093, USA. frankfbd@yahoo.com
10. Bol Asoc Med P R. 2008 Oct-Dec;100(4):25-8. Prevention of infective endocarditis: a review of the American Heart Association guidelines. Sanchez-Rodriguez F, Rivera R, Suarez-Gonzalez J, Gonzalez-Claudio G. Cardiology Section, Department of Medicine, VA Caribbean Healthcare System, San Juan, Puerto Rico, USA.
11. J Oral Maxillofac Surg. 2010 Apr;68(4):949. Antibiotic prophylaxis in artificial joint patients. Wahl MJ.
12. Instr Course Lect. 2003;52:223-45. The infected total hip arthroplasty. Salvati EA, González Della Valle A, Masri BA, Duncan CP. Hip and Knee Service, Hospital for Special Surgery, Cornell University, New York, New York, USA.
13. J Arthroplasty. 2002 Jan;17(1):111-3.Joint arthroplasty, dental treatment, and antibiotics: a review. Curry S, Phillips H. The Old Rectory, Wivenhoe, Essex, United Kingdom. SeanCurry@dial.pipex.com
14. American Academy of Orthopaedic Surgeons
15. Transient Bacteremia Induced by Toothbrushing: A Comparison of the Sonicare Toothbrush With a Conventional Toothbrush by Shamsi Bhanji, Bryan Williams, Barbara Sheller, Thomas Elwood, Lloyd Mancl