Practically every week of the year at Cape Dental Care we will have someone come in with a toothache that ends up being diagnosed sinusitis. Their symptoms include:
- Sore upper posterior teeth (percussion, usually more than one)
- Feeling sensitive/swollen to the touch on their cheek
- Headaches
- Stuffy nose (runny nose, possibly green or yellow discharge)
- Earache
- Malaise
- Post nasal drip (halitosis)
- Fever(viral)
- History of recent upper respiratory infection
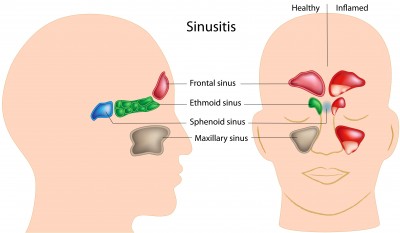
- Maxillary sinuses – They are by far the largest paranasal sinuses in the body. They are golf ball size boney air pockets found in the cheek area. They are believed to serve several purposes including to help warm and humidify the air entering your lungs, add pitch to your voice, lighten the head so it is easier to juggle on top of your spine, and absorb trauma to the face to protect the brain and eyes. Having the maxillary sinus directly below the eye socket protects the eye from being crushed in an accident. Instead, the eyeball can be forced into the maxillary sinus relatively undamaged (blow-out fracture of the eye). This is why the eye can hurt with a maxillary sinus infection.
- Frontal sinuses – These sinuses are above the eyeballs and when infected can give you a forehead headache.
- Ethmoid sinuses – They are usually referred to as the ethmoid air cells and are divided into anterior, middle and posterior air cells. They are located between the eye sockets and the nasal cavity. Another reason why the eyes hurt with ethmoid sinus infections.
- Sphenoid sinuses – They are located far back in the nasal cavity and are closely associated with the base of the brain (pituitary gland) superiorly and the nasopharynx inferiorly. Problems with these sinuses are difficult to diagnoses and treat.
- Mastoid air cells – Although not categorized as paranasal sinuses nor have the same functions, they are air fill chambers in the head that can become infected and cause considerable discomfort and morbidity. They are an interesting group of cavities in the temporal bones (around the ears) that fill with air shortly after birth through the eustachian tube via the middle ear. The normal function of these air cells are to aide in the normal functioning of the middle ear and vibration of the eardrum. They offer a reserve air supply to protect the eardrum from barotrauma and provides slow moving secretions that flush out the middle ear debris through the eustachian tube and out into the nose.
- Viral– This is usually of sudden onset and may last for up to a month. There is no other treatment than hydration, irrigation, and to treat the symptoms like you have a cold or flu. Antibiotics will not help this type of infection. Usually occurs after an upper respiratory infection. Unfortunately, most physicians/nurse practitioners and dentists improperly prescribe antibiotics as a first line treatment.
- Bacterial – This uncommon infection is a slower onset infection and may progress into chronic sinusitis. Fortunately, this infection responds well to various antibiotics (see below).
- Seasonal– This is our most common type of sinusitis. It can be caused by what you breathe in during the day like mold and pollen. Allergies are commonly accompanied with blocked/swollen sinuses. Can be exacerbated by a deviated septum and/or polyps. Consult an allergist/ENT.
- Fungal – This is a very difficult type of infection to treat and can last for many months or years. It is generally classified as allergic fungal sinusitis, acute invasive sinusitis, chronic invasive sinusitis, chronic granulomatous sinusitis, and sinus mycetoma. Fungal infections may develop in patients with poorly controlled diabetics or immunocompromised (leukemia, lymphoma, multiple myeloma, chemotherapy and AIDS). Diagnoses is usually made by a biopsy of the intranasal tissue. Treated with aggressive paranasal surgery is the primary treatment of choice. Anti-fungal drugs such as amphotericin B (1-1.5 mg/kg/d) are used if the fungal infection becomes invasive and moves from the sinus cavity to the adjacent deeper tissues. However, due to the unfavorable long term prognosis and limited treatment options, better therapeutic strategies are currently being explored such as a combination of surgery and a new anti-fungal drug called voriconazole.
- Polyps– Blockage or filling normal sinus structures with diseased tissue. Diagnosed with CAT Scan. Treatment: surgery.
- Deviated septum – This is where the center nasal bone is crooked and doesn’t allow the air to flow unhindered through the nasal passages.
- Irritants– Smoking, air pollution, noxious vapors. Remember smoking while driving in a car with children can be considered child abuse.
- Foreign object – Children can put the darndest things up their nose. Food inside the nasal passages eventually decay and can trigger a foreign body response which could include swelling, purulence and secondary infections.
- Airplane flight – If you are unfortunate to fly when experiencing a cold or sinus infection, you may have a bad flight! Pressure equilibration between blocked paranasal passageways and the middle ear can be a painful experience. Nasal decongestants work well if taken properly. Not taking enough may allow the congestion to return before the flight is over and defeat the purpose of taking medications in the first place (rebound rhinorrhea). Another interesting phenomenon occurs at high cruising altitudes. At sea level the body is not crushed by the weight of the atmosphere because of the sum of partial pressure gases dissolved inside of our bodies counteract the weight of the over head atmosphere (15 pounds per square inch). However, during high altitude flights the pressure of the cabin is approximately ½ that of sea level. That means air has to rush out of the paranasal sinuses and middle ear’s eustachian tube during ascent so the pressure would not cause discomfort. Recycled air inside pressurized cabins is not very pure (dust, body odor, perfumes, coughing/sneezing residue/germs, flatus, dry humidity) and can irritate many passenger’s sinus membranes. On descent, the air now has to rush back into the paranasal sinuses and eustachian tube or a vacuum sinusitis and/or middle ear pain will begin to form. The vacuum will draw transudate from the mucous membranes and fill the sinuses and middle ear causing congestion and possible infection for several days post-flight. (See Vacuum Sinusitis below)
- Wash hands frequently
- Avoid cigarette smoke (second hand too!)
- Be on the lookout for sick looking friends and family (no kissing, hugging or shaking hands – sorry)
- Clean house filters and humidifiers. Houses today are made like ice chests. Very little air exchange with the outside world is a key to energy conservation, but could be a recipe for runny noses. Stale air, dust mites, cooking exhaust, and other occupants contagions can be difficult to avoid if the air conditioner’s air circulation is hindered by dirty filters. Likewise, if you do not clean out old water leftover from the humidifiers, unwanted bacteria/fungus can accumulate and become a chronic source of irritation to the nasal passages.
- Keep up with the families vaccinations
Home Remedies:
- Drink plenty of fluids. This increases the fluids in your bloodstream and moistens the phlegm inside your nose/sinuses.
- Humidification: Increasing the humidity in the room will help moisten the phlegm inside your nose as well. Hot baths/showers will provide much relief from sinus congestion. Over-the-counter humidifiers work well if the house is equipped with an air conditioning system that will allow high humidity, otherwise the moisture will be continually removed by the condensator of the air conditioner. Tenting a small environment or shutting the bathroom door and running the hot shower may work better.
- Over-the-counter (OTC) remedies work well. Antihistamines and decongestants can relieve symptoms of cold/flu, but can leave you with side effects of rebound runny nose, wired or sleepy days and sleepless night. Some people can actually become addicted to nasal sprays. This is when someone has to use a nasal spray several times a day to clear their sinuses/nasal passages in the absences of an infection/irritant. This is called rebound rhinorrhea. The only cure for this addiction is cold turkey. This will result in days of a stopped up nose, but it will soon resolve and breathing will return to normal unless their is a physical obstruction that is hindering your breathing. In this is the case, consult your physician.
- Nasal Irrigation: This is the best kept secret to treating sinusitis. Flushing out the accumulated days nasal filtration is the key to good sinus health. Not only does it flush out pollen, dust, dirt, molds, chemicals, occupational/recreational airborne particulate and environmental pollutants, but it also removes leftover nasal prescription/OTC spray residue. This should become as ritualistic as brushing and flossing your teeth and using xylitol sugar at bedtime. Neti pots and squeeze bottle irrigators are sold at every pharmacy in the USA. Use as directed. Neti pots are harder to use and squeeze bottles can create too much force if not careful. Too much force can push saline solution into the eustachian tubes and possibly push an infection into the middle ear.
- Always consult your physician if the congestion lasts more than a week and/or a fever greater than 100℉.
Systemic Etiology:
Acute sinusitis usually follows a recent upper respiratory infection (rhinitis, flu, common cold). This infection can be either bacterial or viral. Infection can affect the upper airway passageways and the associated swelling can occlude the openings to the various sinus cavities. Blocking off a sinus cavity can cause a painful condition called vacuum sinusitis. This is a condition where the oxygen inside the trapped air, inside the blocked sinus, is absorb into the surrounding blood vessel filled mucous membranes. This resulting negative pressure can be intolerable. If the negative pressure is sustained over a period of time, then it may pull fluid from the mucous membrane subsequently filling the sinus with a transudate liquid that is a good bacteria growth media. The body will respond to any sinus infection by pouring into the sinus compartment white blood cells (leukocytes) and other blood products to fight the infection. The resulting cellulitis/infection creates positive pressure inside the sinus, edema and pain. If tooth nerves are flowing through the infected sinus area, they will enviably be affected. Going to your dentist to differentiate between an actual toothache and a sinusitis is a good way to begin the treatment for this condition. The dentist will see no abscess and a “whited-out” sinus and refer you to your primary care physician or an ENT if you do not currently have a physician.
Dental Etiology:
In about 25% of the cases of maxillary sinusitis the cause is from a tooth borne infection. When bacteria invades the inner pulp chamber of a tooth an infection ensues. The cardinal signs of an infection include: pain, redness, heat and swelling. The tooth’s pulp chamber is known as a solid terminal blood supply. This means blood vessels only go in and out of a small area at the apex of the tooth’s root. In additions, the inside of the tooth is solid as a rock. Meaning it will not allow for any swelling at all. When bacteria enter the pulp chamber (decay, trauma, periodontal disease, crack) and swelling ensues, there is no place for the swelling to expand. Thus the blood coming in gets backed up by the swelling and cannot flow out. If no more blood can flow freely into the inside of the tooth then no more oxygen. If no oxygen, then the pulp tissue inside of the tooth dies. This dead tissue inside the pulp chamber is a good bacterial growth media. Bacteria grow to large numbers before pushing out the tip of the tooth to cause what is seen on the dental radiograph as an abscess. The tips of the upper back teeth are in very close association with the maxillary sinus. In some cases the infection from a tooth can spill over into the sinus causing a sinus infection. The treatment for this type of sinusitis is either a root canal or extraction.
Treatment:
(Always consult your physician before treating a sinusitis lasting more than 1 week and fever of >100℉)
Vacuum Sinusitis (acute): Nasal irrigation, decongestants, nasal sprays. Definitive diagnosis is made by an in-office antroscopy. Surgical treatment is a middle or inferior meatal antrostomy which is basically opening another hole into the maxillary sinus to relieve the vacuum.
Viral Sinusitis: Nasal irrigation, cold and flu OTC medications
Bacterial Sinusitis (pressure): Antibiotics are now being questioned as an appropriate primary treatment for sinusitis.
Primary therapy: Amoxicillin 500mg PO q8hr X 10 days with or without clavulanate. If allergic to penicillin then erythromycin 250mg PO q6hr X 10 days or trimethoprim/sulfamethoxazole 80/400mg PO q6hr X 10 days.
Second-line therapy: Cefuroxime 500mg PO q12hr X 10 days or moxiflorxacin 400mg PO qd X 10 days.
Pediatric note: Do not use fluoroquinolones due to concerns of premature epiphyseal growth plate closure (stunted growth of long bones).
References:
1. Br Dent J. 2011 Feb 12;210(3):113-8. Maxillary sinus disease: diagnosis and treatment. Bell GW, Joshi BB, Macleod RI. Dumfries & Galloway Royal Infirmary, Dumfries.
2. Postgrad Med. 2009 Nov;121(6):121-39. Diagnosis and management of chronic rhinosinusitis in adults. Marple BF, Stankiewicz JA, Baroody FM, Chow JM, Conley DB, Corey JP, Ferguson BJ, Kern RC, Lusk RP, Naclerio RM, Orlandi RR, Parker MJ; American Academy of Otolaryngic Allergy Working Group on Chronic Rhinosinusitis.
3. Auris Nasus Larynx. 2012 Jun;39(3):257-60. Epub 2011 Aug 20. Primary headache syndromes and sinus headache: An approach to diagnosis and management.Cashman EC, Smyth D. Dana-Farber Cancer Institute/Harvard Medical School, Longwood Avenue, Boston, MA, USA.
4. Laryngoscope. 2012 Feb;122(2):467-72. doi: 10.1002/lary.22398. Epub 2012 Jan 17. Microbiome complexity and Staphylococcus aureus in chronic rhinosinusitis. Feazel LM, Robertson CE, Ramakrishnan VR, Frank DN. Division of Infectious Diseases, University of Colorado School of Medicine, Aurora, Colorado, USA.
5. Emerg Med Clin North Am. 1999 Feb;17(1):153-87, ix. Evaluation of the patient with sore throat, earache, and sinusitis: an evidence based approach. Stewart MH, Siff JE, Cydulka RK. Case Western Reserve University School of Medicine, Department of Emergency Medicine, Metro Health Medical Center, Cleveland, Ohio, USA.
6. Clin Evid (Online). 2011 Dec 21;2011. pii: 0511. Sinusitis (acute). Ah-See K. Aberdeen Royal Infirmary, Aberdeen, UK.
7. Clin Evid (Online). 2008 Jul 17;2008. pii: 1305. Halitosis. Scully Cbe C, Porter S. UCL – Eastman Dental Institute, London, UK.
8. J Pediatr Orthop. 2009 Mar;29(2):189-95. The effect of fluoroquinolone antibiotics on growing cartilage in the lamb model. Sansone JM, Wilsman NJ, Leiferman EM, Conway J, Hutson P, Noonan KJ. Department of Orthopedics, School of Medicine and Public Health, University of Wisconsin-Madison, Madison, WI, USA.
9. JAMA. 2012 Feb 15;307(7):685-92. Amoxicillin for acute rhinosinusitis: a randomized controlled trial. Garbutt JM, Banister C, Spitznagel E, Piccirillo JF. Division of General Medical Sciences, Washington University School of Medicine, Campus Box 8005, 660 S Euclid Ave, St Louis, MO 63110, USA.
10. Eur Arch Otorhinolaryngol. 2012 Jul 6. Different types of fungal sinusitis occurring concurrently: implications for therapy. Rupa V, Thomas M. Department of ENT, Christian Medical College, Vellore, 632004, Tamil Nadu, India
11. Am J Rhinol Allergy. 2012 Mar-Apr;26(2):141-7. Antifungal therapy in the treatment of chronic rhinosinusitis: a meta-analysis. Sacks PL 4th, Harvey RJ, Rimmer J, Gallagher RM, Sacks R. St. Vincent’s Clinical School, St. Vincent’s Hospital, University of New South Wales, New South Wales, Sydney, Australia.
12. Otolaryngol Head Neck Surg. 2012 Jun;146(6):880-6. Epub 2012 Feb 1. Evidence of maxillary sinus inflammation in seasonal allergic rhinitis. Baroody FM, Mucha SM, deTineo M, Naclerio RM. Section of Otolaryngology-Head and Neck Surgery, The Pritzker School of Medicine, University of Chicago, Chicago, Illinois 60637, USA.
13. Rhinology. 2011 Jun;49(2):131-8. Mechanisms of the symptoms of rhinosinusitis. Eccles R. Common Cold Centre and Healthcare Clinical Trials Cardiff School of Biosciences, Cardiff University, United Kingdom.
14. Environ Health. 2012 Apr 10;11:25. Exposures to fine particulate air pollution and respiratory outcomes in adults using two national datasets: a cross-sectional study. Nachman KE, Parker JD. Department of Environmental Health Sciences, Johns Hopkins Bloomberg School of Public Health, Baltimore, MD, USA
15. Allergy Asthma Proc. 2012 May-Jun;33 Suppl 1:22-3. Chapter 7: Nasal polyps. Georgy MS, Peters AT. Division of Allergy-Immunology, Department of Medicine, Northwestern University Feinberg School of Medicine, Chicago, Illinois, USA.
16. Med J Malaysia. 2011 Aug;66(3):191-4. The prevalence of anatomical variations in osteomeatal unit in patients with chronic rhinosinusitis. Azila A, Irfan M, Rohaizan Y, Shamim AK. Department of Otorhinolaryngology-Head & Neck Surgery, School of Medical Sciences, Universiti Sains Malaysia Health Campus, 16150 Kota Bharu, Kelantan, Malaysia.
17. Ned Tijdschr Tandheelkd. 2012 Apr;119(4):199-204. [Diseases of the maxillary sinus: an overview]. [Article in Dutch] Baart JA, Bretschneider JH, de Visscher JG, van der Waal I. Uit de afdeling Mondziekten, Kaak- en Aangezichtschirurgie en Oorheelkunde/Hoofd-halschirurgie van het VUmc Amsterdam.
18. J Fam Pract. 2012 Jun;61(6):330-5. Acute respiratory tract infection: a practice examines its antibiotic prescribing habits. Grover ML, Mookadam M, Rutkowski RH, Cullan AM, Hill DE, Patchett DC, Simon EO, Mulheron M, Noble BN. Department of Family Medicine, Mayo Clinic, Scottsdale, AZ 85260, USA.
19. Oral Maxillofac Surg Clin North Am. 2012 May;24(2):285-93, ix. Epub 2012 Feb 29. Revision sinus surgery. Govindaraj S, Agbetoba A, Becker S. Department of Otolaryngology, The Mount Sinai Medical Center, New York, NY 10029, USA.
20. Oral Maxillofac Surg Clin North Am. 2012 May;24(2):191-6, vii-viii. Epub 2012 Feb 14. Microorganisms of the nose and paranasal sinuses. Haug RH. Carolinas Center for Oral Health, Charlotte, NC 28209, USA
21. Am J Rhinol Allergy. 2012 Mar-Apr;26(2):117-9. The significance of computed tomographic findings in the diagnosis of fungus ball in the paranasal sinuses. Chen JC, Ho CY. Department of Otolaryngology, Taipei Veterans General Hospital, and School of Medicine, National Yang-Ming University, Taipei, Taiwan
22. Cent Eur J Public Health. 2012 Mar;20(1):38-44. Parental education and family status–association with children’s cigarette smoking. Zaloudíková I, Hrubá D, Samara I. Department of Psychology, Faculty of Education, Masaryk University, Brno, Czech Republic.
23. Pediatr Emerg Care. 2008 Nov;24(11):785-92; quiz 790-2. Nasal foreign body removal in children. Kiger JR, Brenkert TE, Losek JD. Pediatric Department, Medical University of South Carolina, Charleston, USA.
24. J Allergy Clin Immunol. 1992 Sep;90(3 Pt 2):478-95. Prospects for ancillary treatment of sinusitis in the 1990s. Zeiger RS. Department of Allergy, Kaiser Permanente Medical Center, San Diego, Calif. 92111.
25. Int Forum Allergy Rhinol. 2012 Jun 13. doi: 10.1002/alr.21054. Impact of tobacco smoke on chronic rhinosinusitis: a review of the literature. Reh DD, Higgins TS, Smith TL. Johns Hopkins Sinus Center, Johns Hopkins Medicine, Baltimore, MD.
26. Chest. 2006 Jan;129(1 Suppl):138S-146S. Postinfectious cough: ACCP evidence-based clinical practice guidelines. Braman SS.Division of Pulmonary and Critical Care Medicine, Rhode Island Hospital, 595 Eddy St, Providence, RI 02903, USA.
27. Pneumologie. 1991 Oct;45(10):794-8. [Diagnosis of humidifier lung–comparison of various serologic procedures]. [Article in German] Baur X, Richter G, Pethran A, Czuppon AB, Fruhmann G. Berufsgenossenschaftliches Forschungsinstitut für Arbeitsmedizin, Ruhr-Universität Bochum.
28. Yonsei Med J. 2010 Nov;51(6):918-23. Effect of an air cleaner with electrostatic filter on the removal of airborne house dust mite allergens. Agrawal SR, Kim HJ, Lee YW, Sohn JH, Lee JH, Kim YJ, Lee SH, Hong CS, Park JW. Division of Allergy and Immunology, Institute of Allergy, Department of Internal Medicine, Yonsei University College of Medicine, Seoul, Korea.
29. Prim Care. 2002 Jun;29(2):231-61. Respiratory and allergic diseases: from upper respiratory tract infections to asthma. Jaber R. Division of Wellness and Chronic Illness, Department of Family Medicine, University Hospital and Medical Center, Health Sciences Center, State University of New York at Stony Brook, Stony Brook, NY 11794-8461, USA.
30. Arch Otolaryngol Head Neck Surg. 2008 Sep;134(9):931-5. Nasal-air conditioning in patients with chronic rhinosinusitis and nasal polyposis. Papp J, Leiacker R, Keck T, Rozsasi A, Kappe T. Department of PediatricOncology, University Children’sHospital, University of Ulm, Ulm, Germany.
31. Rhinology. 2012 Jun;50(2):157-64. Numerical simulation of humidification and heating during inspiration within an adult nose. Sommer F, Kroger R, Lindemann J. Department of Otorhinolaryngology, Head and Neck Surgery, University Hospital Ulm, Ulm, Germany.
32. Fed Regist. 2005 Oct 11;70(195):58974-7. Cold, cough, allergy, bronchodilator, and antiasthmatic drug products for over-the-counter human use; amendment of final monograph for over-the-counter nasal decongestant drug products. Final rule. Food and Drug Administration, HHS.<
33. J Fam Pract. 2002 Dec;51(12):1049-55. Efficacy of daily hypertonic saline nasal irrigation among patients with sinusitis: a randomized controlled trial. Rabago D, Zgierska A, Mundt M, Barrett B, Bobula J, Maberry R. Department of Family Medicine, University of Wisconsin, Madison, 53715, USA.
34. Adv Physiol Educ. 2006 Mar;30(1):30-2. Resorption of gas trapped in body cavities: comparison of alveolar and pleural space with inner ear and paranasal sinuses. Ivezić Z, Kurbel S, Skrinjarić-Cincar S, Radić R. Osijek Medical Faculty, University of Osijek, Osijek, Croatia.
35. Laryngoscope. 2012 Sep;122(9):1910-4. doi: 10.1002/lary.23427. Epub 2012 May 29. Otolaryngologists’ perceptions of odontogenic maxillary sinusitis. Longhini AB, Branstetter BF, Ferguson BJ. School of Medicine, University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania, U.S.A..
36. Otolaryngol Head Neck Surg. 1992 Jul;107(1):21-8.Infraorbital nerve dehiscence: the anatomic cause of maxillary sinus “vacuum headache”? Whittet HB. ENT Department, Radcliffe Infirmary, Oxford, England.
37. Curr Opin Otolaryngol Head Neck Surg. 2004 Feb;12(1):27-9. Chronic sinusitis: symptoms versus CT scan findings. Stewart MG, Johnson RF. The Bobby R. Alford Department of Otorhinolaryngology and Communicative Sciences, Baylor College of Medicine, Houston, Texas 77030, USA
38. Otolaryngol Clin North Am. 2012 Jun;45(3):631-42, viii. Allergic fungal sinusitis in children. Thorp BD, McKinney KA, Rose AS, Ebert CS Jr. Department of Otolaryngology-Head and Neck Surgery, University of North Carolina School of Medicine, Campus Box #7070, Chapel Hill, NC 27599-7070, USA.
39. J Allergy Clin Immunol. 2012 Feb;129(2):321-6. Epub 2011 Dec 28. Fungal disease of the nose and paranasal sinuses. Thompson GR 3rd, Patterson TF. Department of Medical Microbiology and Immunology, Coccidioidomycosis Serology Laboratory, University of California-Davis, Davis, Calif 95616, USA.
40. Lin Chung Er Bi Yan Hou Tou Jing Wai Ke Za Zhi. 2011 Oct;25(20):916-9. [Clinical study of chronic invasive sinusitis caused by dematiaceous fungi]. [Article in Chinese] Fang G, Zhang Q, Zhu L, Li D. Department of Otolaryngology, the Third Hospital, Peking University, Beijing, 100191, China.
41. Auris Nasus Larynx. 2010 Apr;37(2):244-9. Epub 2009 Jun 23. New treatment for invasive fungal sinusitis: three cases of chronic invasive fungal sinusitis treated with surgery and voriconazole. Nakaya K, Oshima T, Kudo T, Aoyagi I, Katori Y, Ota J, Hidaka H, Oda K, Kobayashi T. Department of Otolaryngology-Head and Neck Surgery, Tohoku University Graduate School of Medicine, 1-1 Seiryo-cho, Aoba-ku, Sendai, Miyagi, Japan.
42. Curr Opin Otolaryngol Head Neck Surg. 2009 Feb;17(1):23-7. Granulomatous disorders of the nose and paranasal sinuses. Fuchs HA, Tanner SB. TN Valley Healthcare System, Nashville Campus, Department of Veterans Affairs Medical Center, and Division of Rheumatology, Vanderbilt University School of Medicine, Nashville, Tennessee, USA.
43. Kulak Burun Bogaz Ihtis Derg. 2011 Nov-Dec;21(6):338-40. doi: 10.5606/kbbihtisas.2011.052. Two cases with unusual mycetoma localizations in upper respiratory system. Bektaş D, Ural A, Caylan R, Bahadır O, Kul N, Caylan R. Department of Otolaryngology, Medicine Faculty of Karadeniz Technical University, Trabzon, Turkey.
44. Aerosp Med. 1972 Sep;43(9):1031-3. Aeromedical considerations in the management of paranasal sinus barotrauma. Smith JP, Furry DE.
45. J Laryngol Otol. 2011 Feb;125(2):188-92. Epub 2010 Nov 17. ENT morbidity at high altitude. Prasad BK. Department of ENT and Head and Neck Surgery, Command Hospital (Eastern Command (EC)), Kolkata, West Bengal, India.